Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu PhD. MD Candidate, Keck School of Medicine, Los Angeles, USA, Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, September 2015. DermNet Revision September 2021
Introduction Demographics Causes Clinical features Diagnosis Treatment Outcome
X-linked agammaglobulinaemia is an inherited genetic disorder characterised by the failure to produce mature B-lymphocytes and plasma cells. Affected patients have severe deficiencies in all immunoglobulins.
X-linked agammaglobulinaemia was first described in 1952 by Dr Ogden Bruton so is also called Bruton agammaglobulinaemia/hypogammaglobulinaemia.
Gamma globulins are also called immunoglobulins. They are proteins produced by plasma cells and are essential to the body’s immune defence system. Agammaglobulinaemia means the absence of gamma globulins.
The risk factors for X-linked agammaglobulinaemia include:
X-linked agammaglobulinaemia is caused by mutations on Bruton’s Tyrosine Kinase (BTK) gene, which was discovered in 1993. The gene normally promotes the maturation of B-lymphocytes. Since the BTK gene is found on the X-chromosome, X-linked agammaglobulinaemia presents exclusively in males. Females can present with an autosomal recessive version of agammaglobulinaemia.
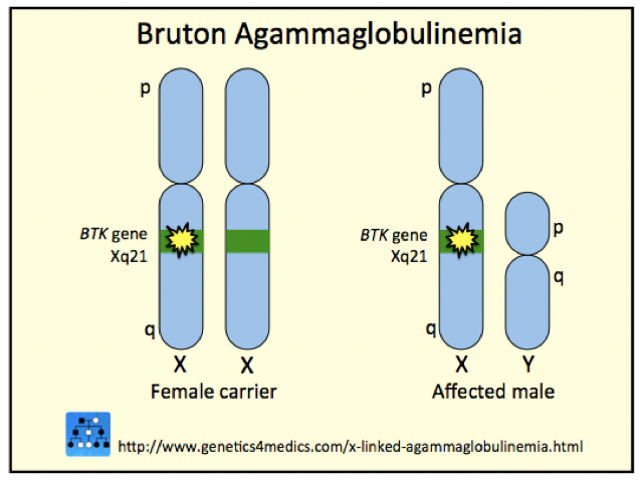
Genetics of X-Linked-agammaglobulinemia
Babies with X-linked agammaglobulinaemia appear healthy at first. They begin to have recurrent infections as the protection of their mother’s antibodies wears off.
X-linked agammaglobulinaemia can be diagnosed on investigations including:
There is no cure for X-linked agammaglobulinaemia. However, treatment can greatly improve quality of life for X-linked agammaglobulinaemia patients.
Immunoglobulin replacement therapy reduces the risk of invasive infection. Chronic lung disease still develops and overall survival is reduced.