Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2002. Updated by Dr Jannet Gomez, August 2016.
Introduction
Causes
Prevalence
Spread
Signs and symptoms
Diagnosis
Treatment
Complications
Prevention
Rubella is a viral disease characterised by rash, swollen glands and fever. The disease is usually mild and of little significance unless you are pregnant. Infection of a pregnant woman (congenital rubella syndrome) commonly results in miscarriage, stillbirth, or birth of an infant with major birth abnormalities.
Rubella is also known as German measles or three-day measles.
Rubella is caused by the rubella virus, in the Rubivirus genus.
Rubella is now rarely seen in countries where rubella vaccination is part of their routine immunisation programme. In countries that do not have immunisation programmes in place, rubella continues to be a mild childhood illness that may even pass un-noticed. The major burden is congenital rubella syndrome and its devastating effects to the unborn fetus.
Rubella is spread from person to person through direct contact with nasal or throat secretions of infected individuals. An infected person is contagious from 7 days prior to the rash appearing until 7 days later. Patients are most contagious when the rash is erupting. Children and adults with rubella should avoid attending childcare facilities, school, work or other public places during their infectious period. An acute infection of rubella almost always confers lifelong immunity.
In 25-50% of rubella cases the disease is usually so mild there may be few or no signs or symptoms. In typical cases the incubation period is between 12-23 days, most people show symptoms within 16-18 days after exposure. Common symptoms include:
Other symptoms include pain and swelling in joints (arthralgia and arthritis). This is more common in adults, particularly women, and may persist longer than 2 weeks. The arthritis may become chronic and persist for months or years.
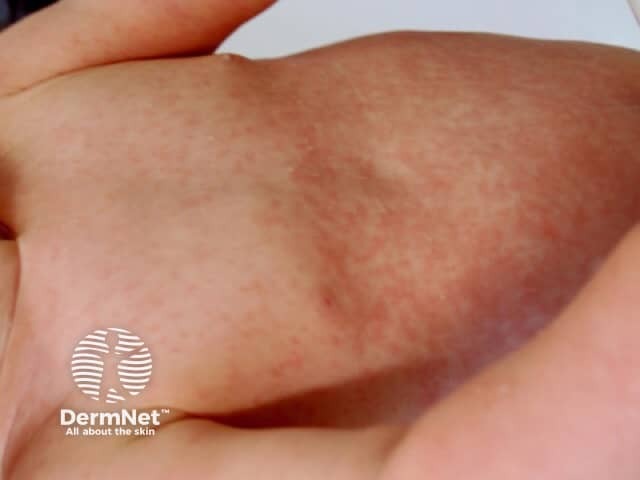
Rubella rash
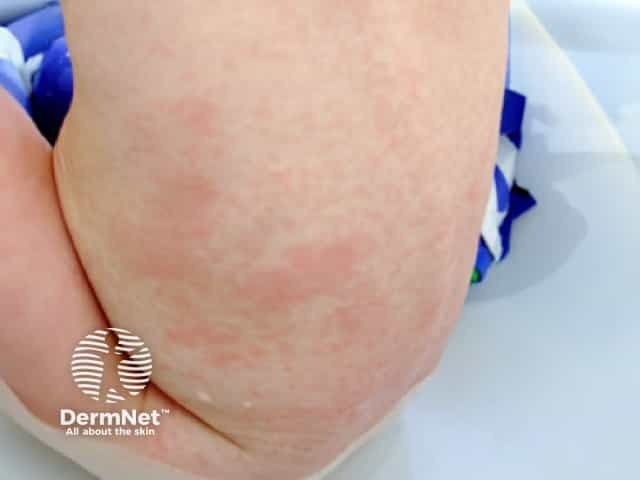
Rubella rash
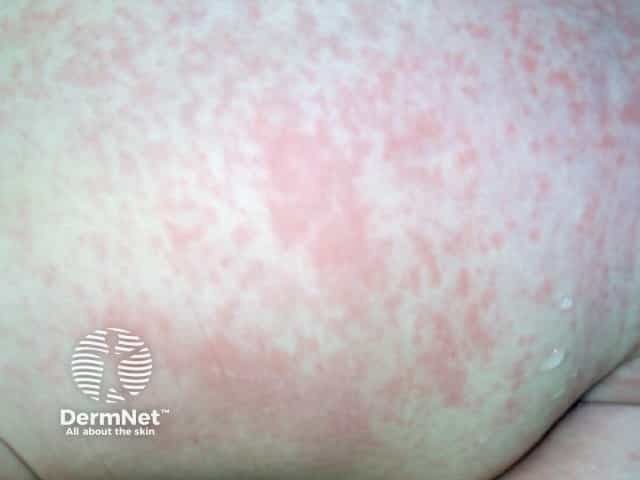
Rubella rash
Because rubella is usually mild and self-limiting, diagnosis in healthy children is based on the characteristic history and physical examination.
Diagnosis of rubella in adults, particularly women of childbearing age, should be confirmed with laboratory testing, as one based on clinical presentation alone is unreliable. The most common test is IgG and IgM serology. Rubella virus can be isolated from throat swabs, blood, urine and spinal fluid by polymerase chain reaction (PCR) testing and molecular typing.
Other tests include CBC, to detect thrombocytopenia and leucopenia, and LFT, to detect viral hepatitis.
There is no specific treatment for rubella. The disease is usually mild and self-limiting. Rest, maintaining fluid intake and possibly taking paracetamol for fever, discomfort or joint pains, are all that is usually required.
Complications are rare with rubella in healthy infants and adults. Complications can include:
Rubella is part of the TORCH complex. Infection in the first trimester of pregnancy comes with a 50% chance of the infant being affected in some way, including miscarriage, fetal death/stillbirth and the congenital rubella syndrome. Features of the congenital rubella syndrome include:
Congenital rubella is one of the causes of the blueberry muffin syndrome, which presents with multiple blue or purple macules, papules and nodules.
Rubella and congenital rubella syndrome can be prevented by vaccination with live rubella vaccine. Combined measles, mumps and rubella (MMR) vaccine is currently part of routine immunisation programmes in most industrialised countries, including New Zealand.
Rubella vaccine induces long-term (probably life-long) immunity in most individuals. Vaccination schedules recommend a two-dose immunisation strategy, the first dose at 12-15 months, followed by a second dose at 4-6 years.
Women of childbearing age should have their immunity status determined by a blood test before attempting to conceive. Rubella vaccine should be given if they have no antibodies to rubella virus, after which there should be at least a 3-month period before trying to conceive.