Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Lesions (cancerous) Terminology
Author: Dr Diana Purvis, Paediatric Dermatologist, Starship Hospital, Auckland, 2010.
Introduction Causes Symptoms and signs Management Treatment and prognosis
‘Blueberry muffin syndrome’ is the descriptive term used for an infant born with multiple blue/purple marks or nodules in the skin. These are due to the presence of clusters of blood-producing cells in the skin (extramedullary erythropoiesis), or bleeding into the skin (purpura), or spreading cancer (metastases).
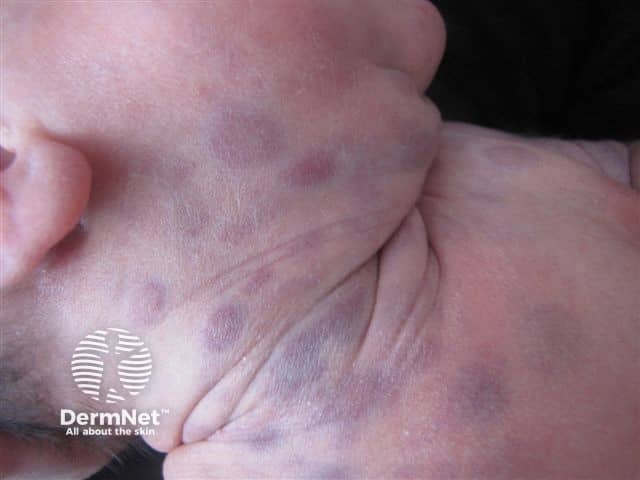
Blueberry muffin syndrome
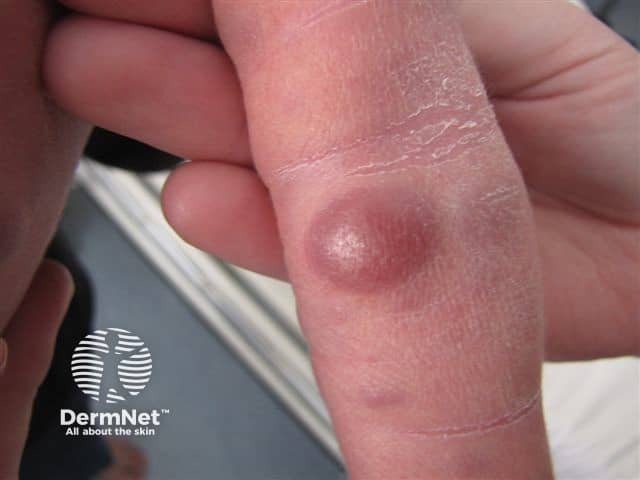
Blueberry muffin syndrome
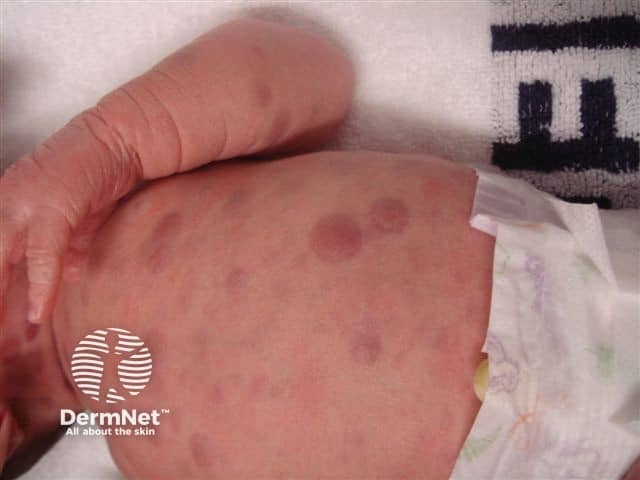
Blueberry muffin syndrome
There are many underlying causes that need to be considered when a baby presents with blueberry muffin syndrome. These include:
Tumours such as:
Blood disorders such as:
Congenital infections such as:
The TORCH complex is a medical acronym used for these serious congenital infections: Toxoplasmosis, Other infections, Rubella, Cytomegalovirus, Herpes simplex virus. The other infections are hepatitis B, coxsackie virus, syphilis, varicella-zoster virus and parvovirus/erythrovirus B19.
Frequently there may be associated anaemia and enlargement of the liver and spleen (hepatosplenomegaly).
Infants with congenital infection may show other features such as:
The investigation and management of an infant with blueberry muffin syndrome often involves many specialists:
Investigations may include:
The treatment and prognosis depends upon the underlying cause.