Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Mohamed Mahrous, Medical Writer, Ontario, Canada, and DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. February 2018.
TORCH infections
TORCH viral infections
Prevention of infection in pregnancy
Upper respiratory tract infections are common in pregnancy and are generally no more serious than when the mother is not pregnant. However, the infections listed here are important causes of maternal and fetal morbidity and mortality. The risk that the infection will harm the fetus is often greater if the mother is infected in early pregnancy.
(Refer also to listeriosis, a cause of fetal loss).
The acronym 'TORCH' has been used as a reminder of infections that cause congenital defects. The TORCH complex represents:
The 'Others' category includes represent syphilis, a bacterial infection; parvovirus B19 (B19V, cause of fifth disease); the cause of erythema infectiosum (also known as fifth disease); varicella zoster virus (VZV) cause of chickenpox measles virus enteroviruses; lymphocytic choriomeningitis (LCM) virus, human immunodeficiency virus (HIV); and Zika virus. Other viruses suspected of causing intrauterine infection are West Nile virus, adenovirus, and hepatitis E virus.
The TORCH viral infections are listed alphabetically below.
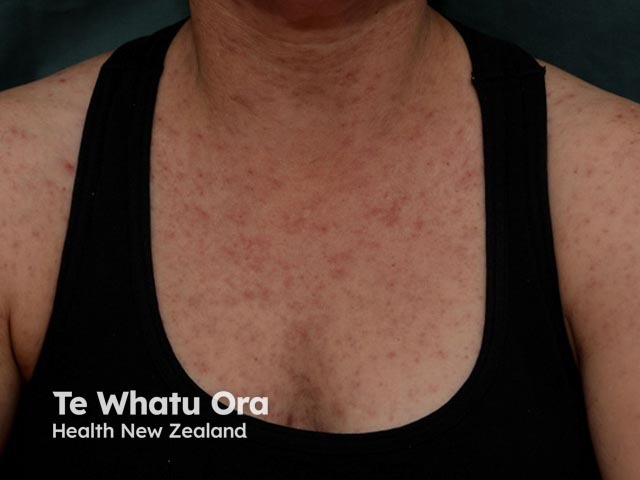
Measles
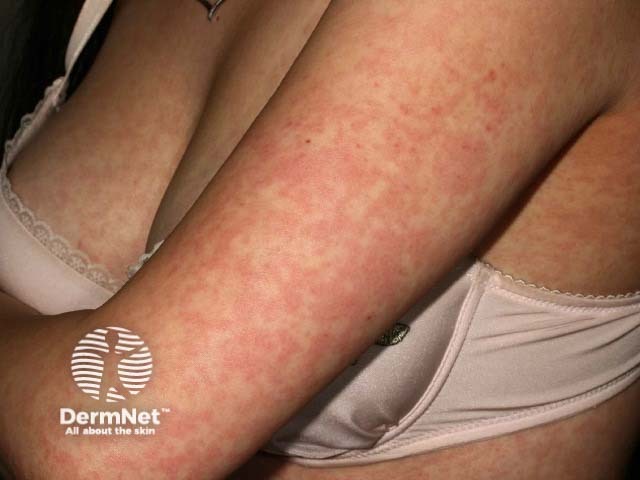
Parvovirus
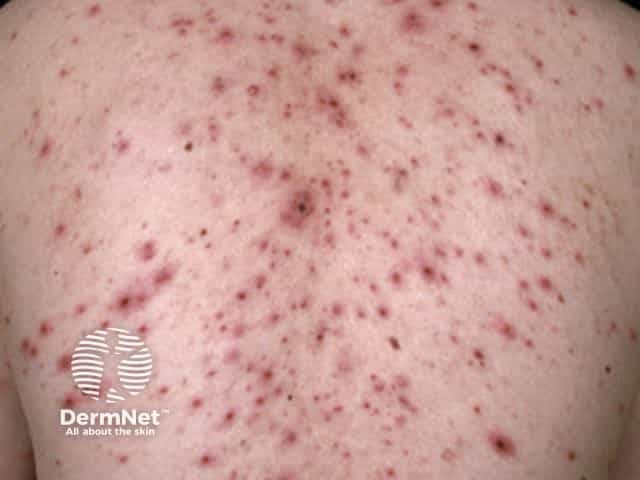
Varicella
It is very important to educate women of childbearing age about the importance of vaccination against measles, rubella, and VZV.
Pregnant women should take care to avoid contact with persons with viral infections and to wash hands frequently when handling food, animals, and children. If exposure to TORCH infections does occur, the patient should seek immediate medical assistance. Pregnant women should also be warned about the risks of travel to regions where these infections are endemic.