Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Impetigo is due to localised, superficial and non-follicular infection with Staphylococcus aureus &/or Streptococcus pyogenes. Ecthyma is a deeper infection due to the same organisms.
Staphylococcal impetigo is characterised by surface honey-yellow crusting or blisters. It tends to be itchy. Streptococcal impetigo is characterised by crusts and ulceration. Ecthyma results in scabs covering full skin thickness ulceration. These deeper infections may be painful.
Bullous impetigo is due to S. aureus that produces an exfoliative exotoxin, exfoliatin. This cleaves desmoglein 1 complex and produces a split between stratum granulosum and stratum spinosum within the epidermis.
Impetigo Impetigo Bullous impetigo Ecthyma 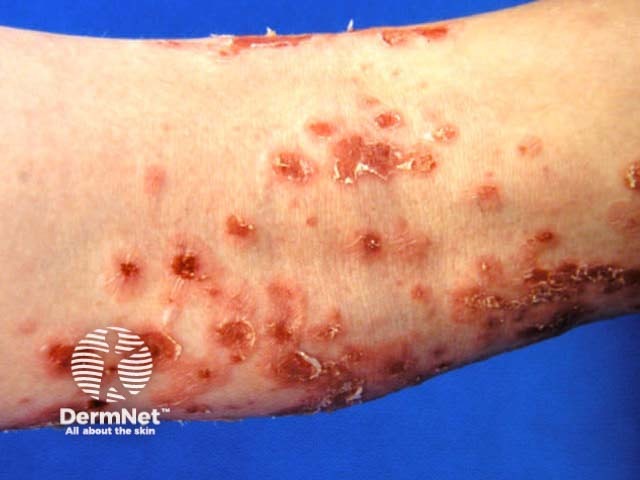
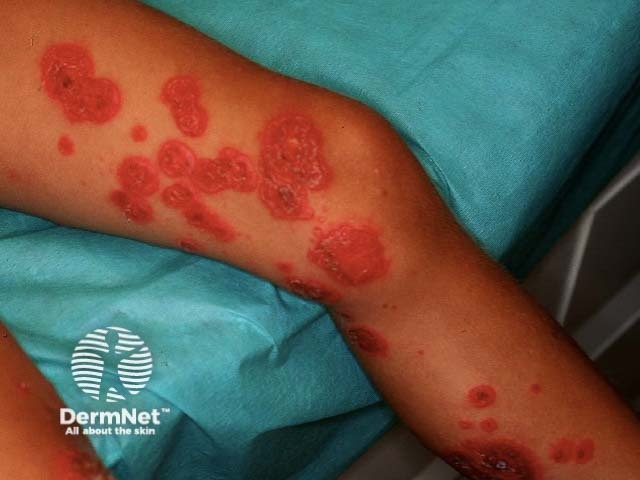
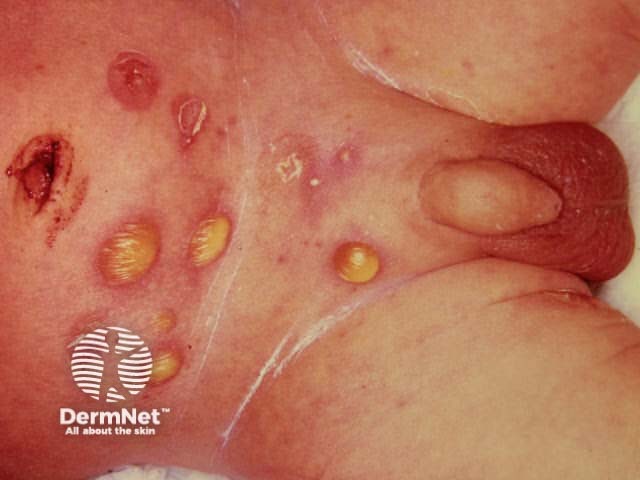
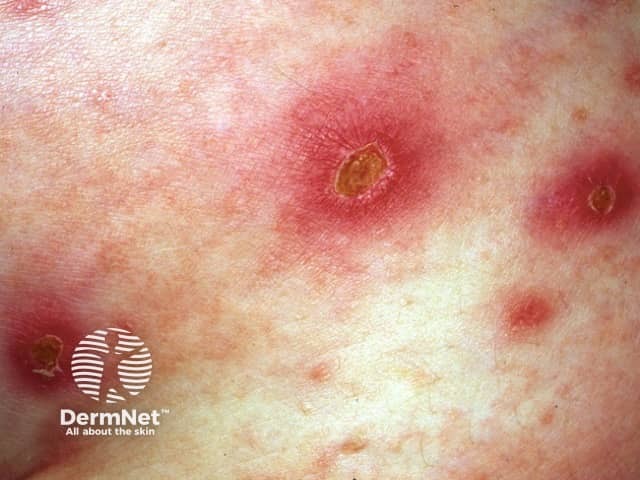
These infections may complicate wound healing, infestations and all forms of dermatitis. Infection may conversely precipitate or aggravate dermatitis.
Impetigo Impetigo Bullous impetigo Ecthyma 



Staphylococcal infections are contagious, requiring careful attention to hygiene.
Localised staphylococcal infections may be managed using meticulous wound care and antiseptics (povidone iodine, chlorhexidine, triclosan and others) as local application and cleanser. The routine use of topical antibiotics (particularly fusidic acid and mupirocin) is undesirable because of increasing prevalence of topical antibiotic-specific and methicillin-resistant strains of staphylococci.
Oral antibiotics may be prescribed for more extensive or recurrent infections but should not be prescribed for trivial reasons. Firstline treatment should be with flucloxacillin or dicloxacillin. In penicillin-allergic patients, erythromycin may be used but there is a higher rate of resistance.
In recurrent cases, take swabs from active lesions and nostrils to determine antibiotic sensitivity. Your local microbiologist may advise about which secondline antibiotic(s) to select. Choices include:
Consider predisposing causes:
1. Define community acquired methicillin resistance.
2. Investigate and summarise the infection control policy for management of methicillin-resistant Staphylococcus aureus in your region.
Information for patients
See the DermNet bookstore