Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Toxic epidermal necrolysis (T.E.N.) is characterised by fever (>38C), widespread tender erythema affecting >30% skin surface associated with mucosal involvement. Erythema is followed by extensive full thickness cutaneous and mucosal necrosis and denudation within 2 or 3 days. Similar symptoms and signs involving less than 10% of the body surface are classified as Stevens-Johnson syndrome (SJS); if 10-30% of body surface area is affected it is classified as T.E.N. / SJS overlap.
The prodromal rash may be non-specific or there may be target lesions. Later, fluid filled blisters spread with lateral pressure (Nikolsky's sign) and peel off to reveal bright red oozing dermis. Hair and nails may be shed.
The mechanism is related to cell-mediated cytotoxic reaction against epidermal cells by activated lymphocytes and their cytokines.
T.E.N. is a medical emergency with significant mortality and should be managed in a burns unit or intensive care facility. Luckily it is rare, with an annual incidence of one per million.
Drugs are responsible for more than 80% of cases of T.E.N., most often begun one to three weeks prior to presentation. A patient with a history of T.E.N. is at serious risk of recurrence if exposed to the same drug or another drug in the table below. Family members are also at increased risk compared to the normal population.
Acute graft versus host disease may also result in T.E.N. and is usually fatal.
| The most common drugs causing T.E.N. |
|---|
|
Toxic epidermal necrolysis Toxic epidermal necrolysis Toxic epidermal necrolysis Toxic epidermal necrolysis Toxic epidermal necrolysis Toxic epidermal necrolysis 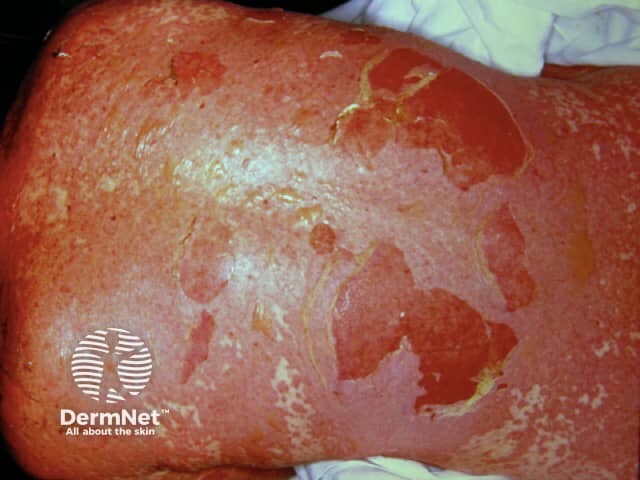
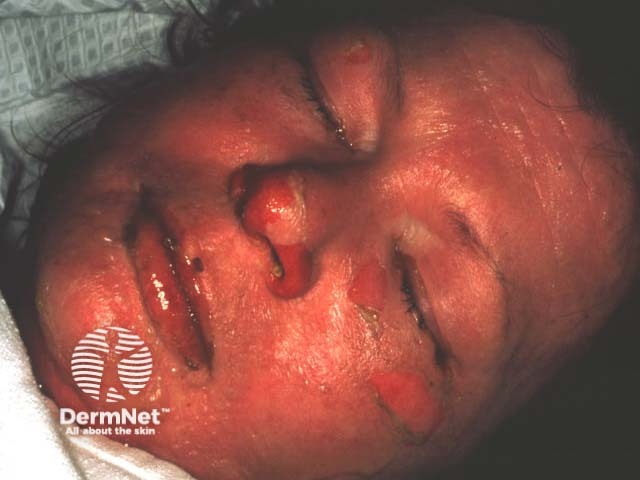
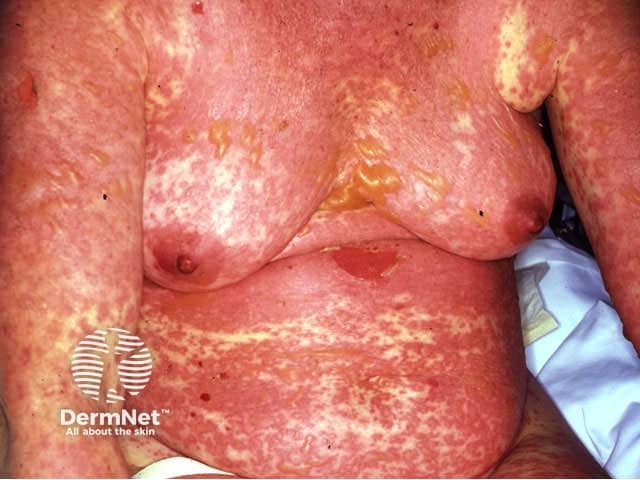
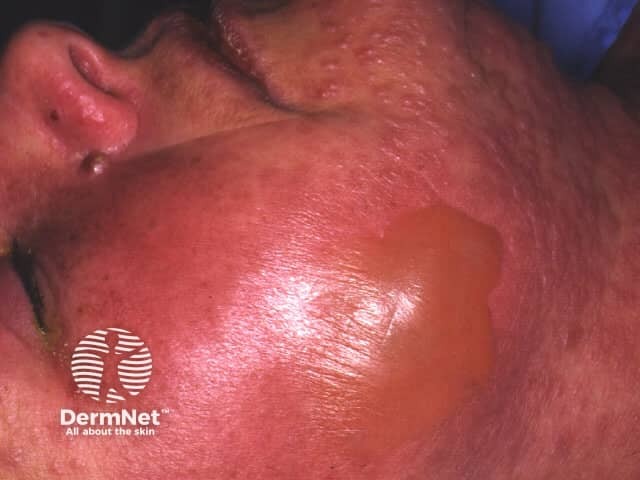
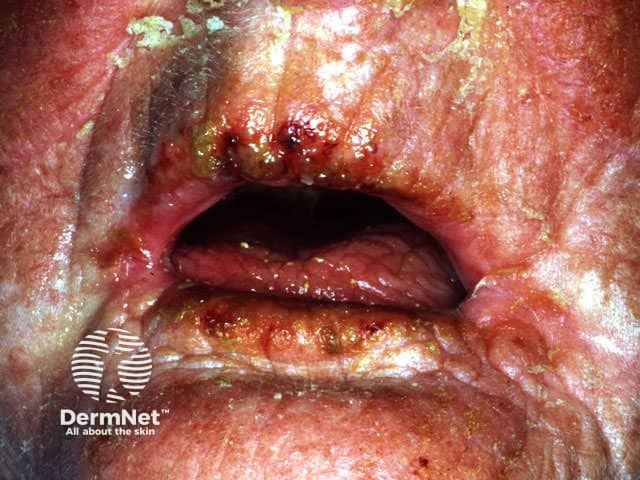
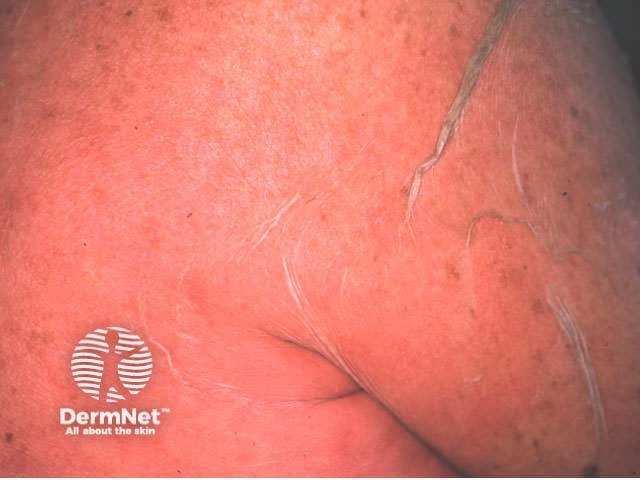
The differential diagnosis includes:
Look for underlying causes and complications of the disease.
The presence of Staphylococcus aureus does not prove infection or aetiology. Neutropaenia has a poor prognosis.
Skin biopsy findings are often diagnostic:
T.E.N. has significant morbidity as a result of dehydration, protein loss, thermoregulatory difficulties, renal tubular necrosis, eroded gastrointestinal tract, interstitial pneumonitis, neutropaenia, liver and heart failure. The mortality rate approaches 30%, most commonly from bacterial sepsis and T.E.N. is especially dangerous in those over 60.
SCORTEN is an illness severity score that has been developed to predict mortality in SJS and TEN cases. One point is scored for each of seven criteria present at the time of admission. These criteria are:
| Predicted mortality | |
|---|---|
| SCORTEN 0-1 | > 3.2% |
| SCORTEN 2 | > 12.1% |
| SCORTEN 3 | > 35.3% |
| SCORTEN 4 | > 58.3% |
| SCORTEN 5 or more | > 90% |
The most recently prescribed medications should be immediately discontinued and should never be readministered. The patient should wear a MedicAlert bracelet. Recurrent T.E.N. is more severe than the initial episode.
Management should be in an intensive care unit and may require:
Systemic corticosteroids may increase mortality and in general should be avoided. Their use is controversial.
Recovery takes 10 days to 3 weeks and may be followed by irregular pigmentation and mucosal scarring. Eye complications are relatively common.
Outline the evidence for and against a beneficial effect of intravenous immunoglobulins in T.E.N..
Information for patients
See the DermNet bookstore