Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Erythroderma is the term used to describe inflammatory skin disease affecting the entire skin surface. It may be acute or chronic. It often precedes or is associated with exfoliation when it may also be known as exfoliative dermatitis.
Causes include:
Erythroderma Erythroderma Erythrodermic psoriasis Erythroderma Erythroderma 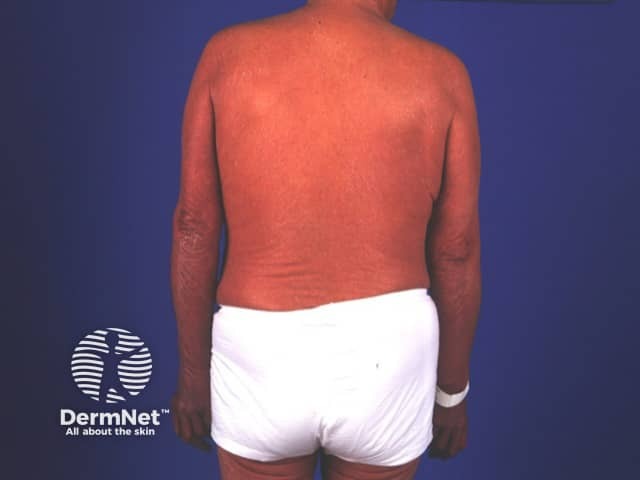
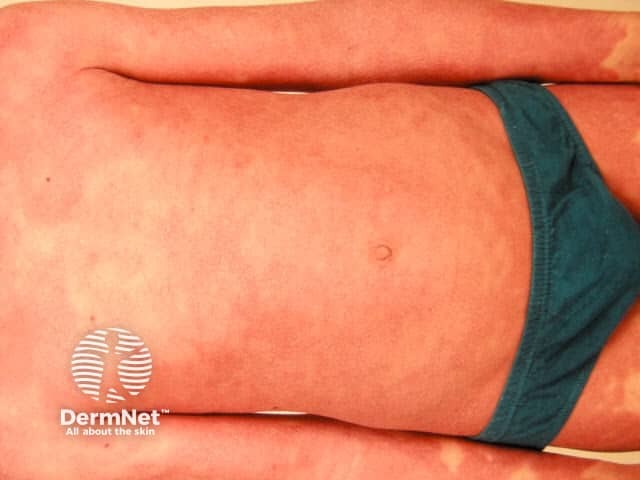
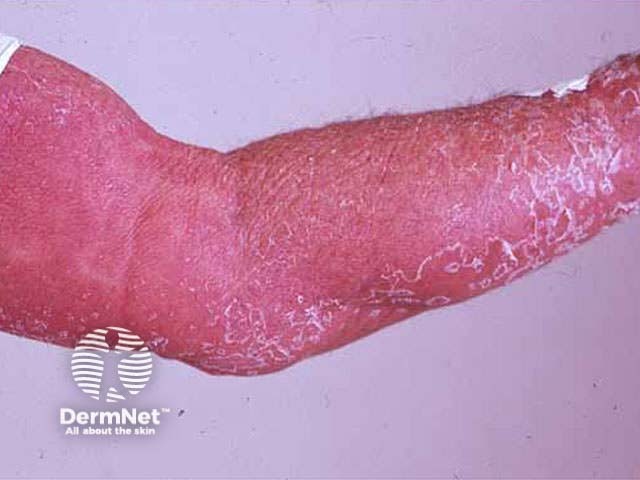
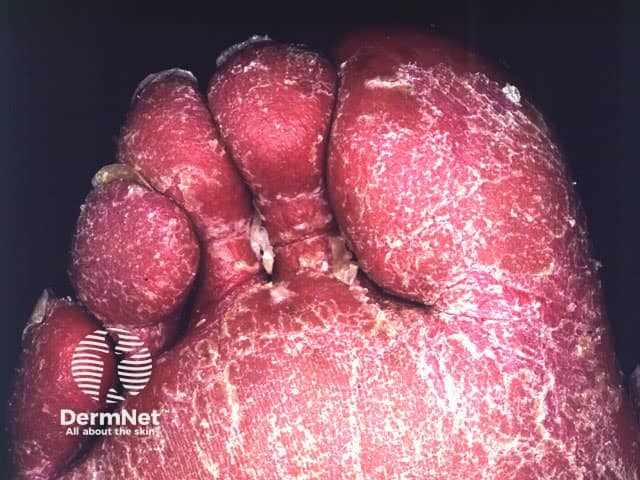
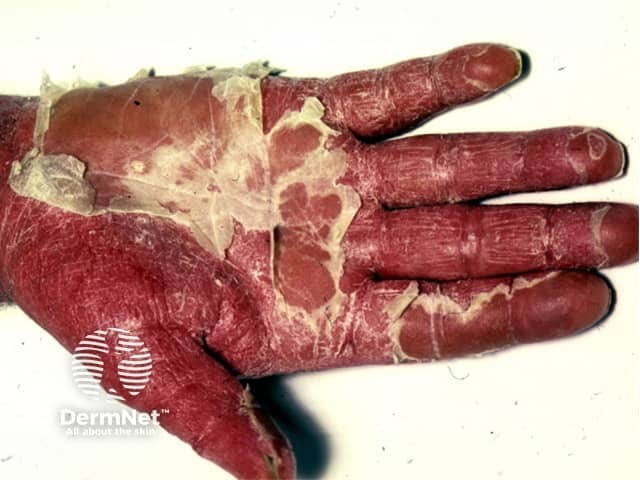
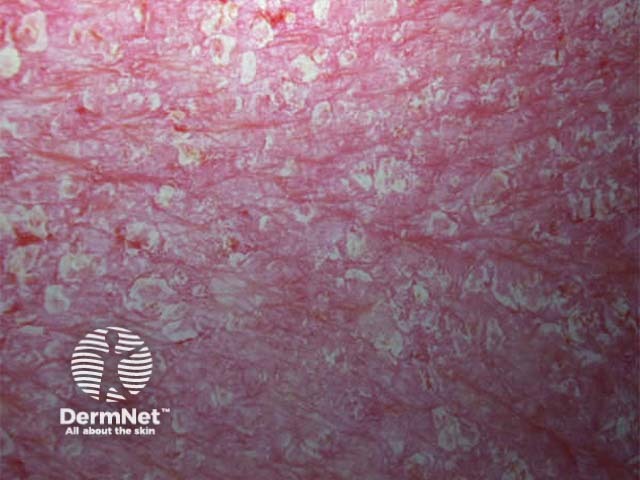
Clinical features depend on the underlying cause. Generalised skin redness (erythema) may be accompanied by oedema (especially if due to eczema or drugs), serous exudate (eczema), scaling (eczema, psoriasis). Degree of itch varies from none (PRP) to intolerable (eczema, bullous diseases). Other features include:
Complications may include:
Investigations should be performed to identify underlying causes and complications. They may include:
The underlying cause of erythroderma should be established if possible. Most patients with acute erythroderma require hospitalisation to restore fluid and electrolyte balance, circulatory status and body temperature. However, erythroderma may also be relatively asymptomatic and managed as outpatient.
Where relevant:
Systemic treatment depends on the underlying cause and should be directed by a dermatologist.
Compare erythroderma arising in childhood with that occurring in the elderly.
Information for patients
See the DermNet bookstore