Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2009.
Tinea unguium is most often due to Trichophyton rubrum and T. interdigitale. It should be distinguished from other causes of onychomycosis:
Tinea unguium is increasingly prevalent with increased age and spreads from tinea pedis or less often, tinea manuum. It may affect one or more toenails and/or fingernails and most often involves the great toenail or the little toenail. It is often confused with non-infected nail dystrophy due to skin disease, particularly psoriasis (also dermatitis, lichen planus, viral warts, ageing changes).
It can present as several different patterns:
Lateral onychomycosis Superficial white onychomycosis Total nail destruction due to fungal infection 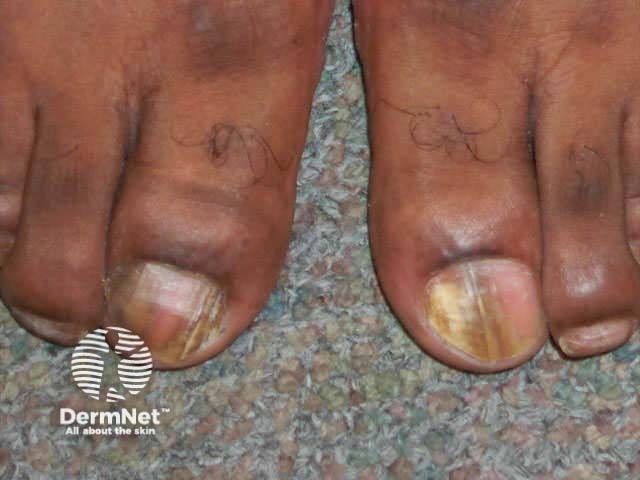
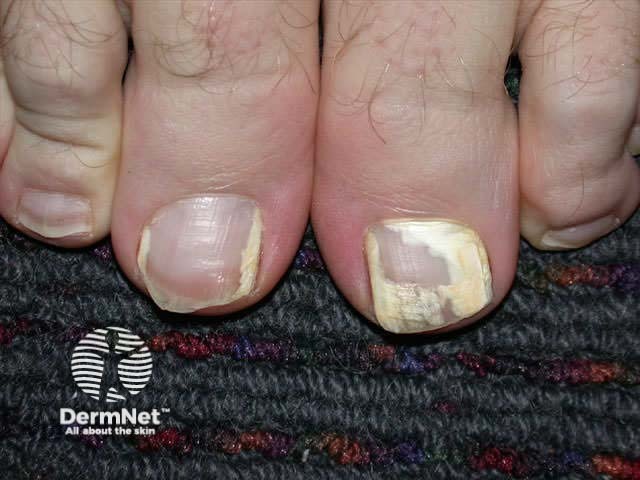
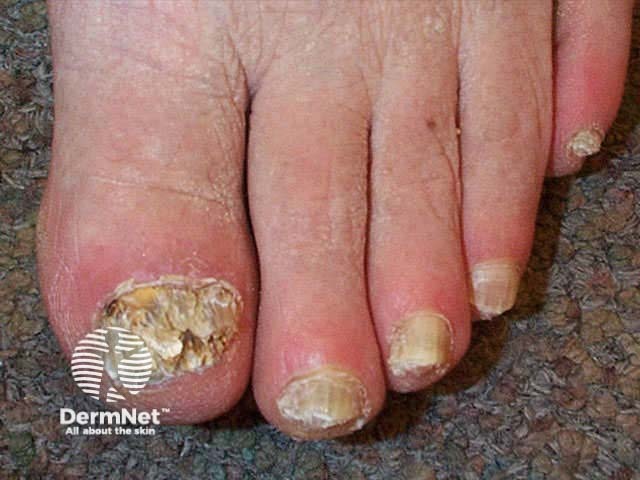
Onychomycosis may look similar to nail dystrophy due to trauma, psoriasis, lichen planus, aging changes and even melanoma. Fungal infection is quite common in damaged nails, so antifungal therapy does not always return the nail to normal even when culture is positive.
Clippings should be taken from crumbling tissue at the end of the infected nail. The discoloured surface of the nails can be scraped off. The debris can be scooped out from under the nail.
Previous treatment can reduce the chance of growing the fungus successfully in culture so take the clippings before treatment is commenced:
Mild infections affecting less than 80% of one or two nails may respond to topical antifungal medications but cure usually requires an oral antifungal medication. Fingernail infections are usually cured more quickly and effectively than toenail infections.
Effective drugs are expensive and treatment is not always indicated:
Topical antifungals are used twice weekly for 6 -12 months for nail plate infections:
Azole oral antifungals require specialist approval for subsidy. They should be avoided in pregnancy. The duration of therapy ranges from 6-12 weeks (fingernails) or 3-6 months (toenails):
Removal of the nail is rarely necessary but may be considered if there is total nail destruction. Surgical removal is unpleasant and painful. Chemical evulsion can be performed by applying urea paste under occlusion and repeating every few days as necessary. It may take many months for the nail to regrow.
Determine the prevalence of fungal infection of the toenails in your patients. Examine the feet of the next 20 adults that you see.
Information for patients
See the DermNet bookstore