Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2009.
If an adult or child presents with an acquired predominantly scaly eruption, the most likely explanation is psoriasis, which is estimated to affect 1-4% of the population. Itching may be absent but tends to be mild to moderate. Psoriasis is a chronic dermatosis of genetic origin, often precipitated by an event such as an infection, an injury or psychological stress. It is associated with inflammatory arthropathy.
Genetic predisposition
There appear to be at least seven psoriasis susceptibility genes. Abnormal expression of one or more of these leads to infiltration of psoriatic plaques by Th1 or cytotoxic lymphocytes and subsequent overproduction of certain pro-inflammatory cytokines, particularly tumour necrosis factor-alpha (TNF-α), interferon-gamma (IFN-γ), interleukins 2 and 12.
The cytokines stimulate keratinocyte proliferation. Epidermal cells take about a week instead of the normal month or two to transit through the skin, with an increased number of actively dividing cells and an increased rate of reproduction. This is a similar pattern to healing wounds.
Precipitating causes
Although there is often no obvious cause, the following may induce or aggravate psoriasis:
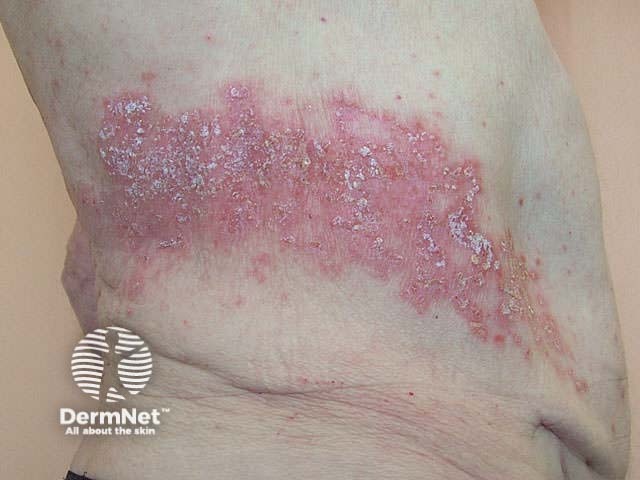
Characteristics of psoriatic plaque
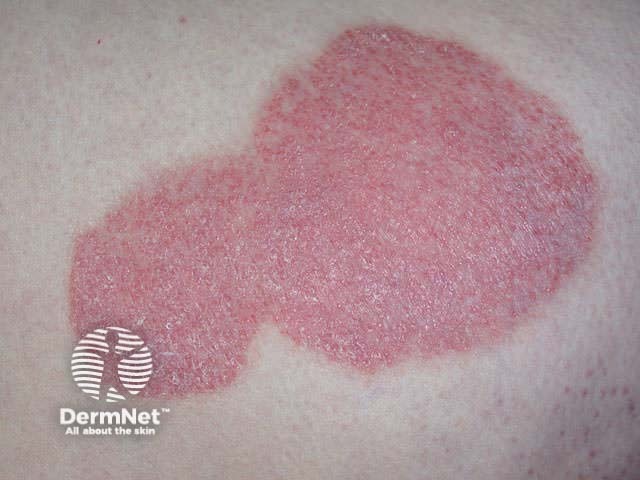
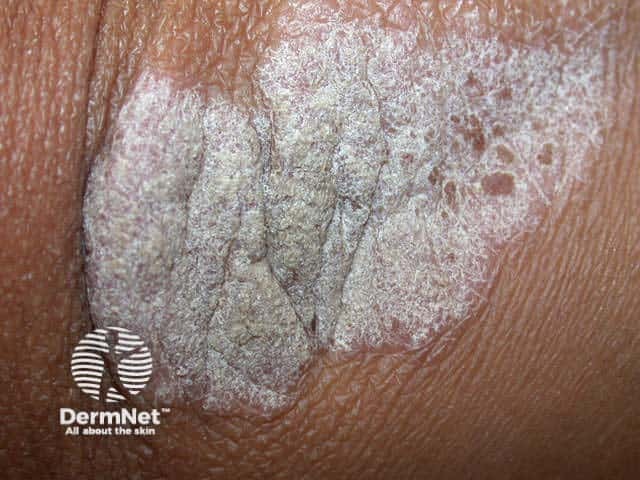
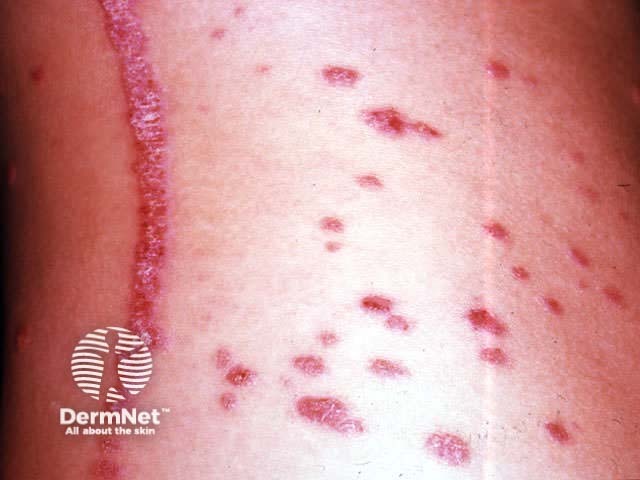
The PASI score (Psoriasis Area and Severity Index) is used to evaluate severity in plaque psoriasis and ranges from 0 to 72. The PASI evaluates the degree of erythema, thickness, and scaling of psoriatic plaques, and estimates the extent of involvement of each of these components in four separate body areas (head, trunk, upper and lower extremities). In general terms, PASI > 12 defines severe, PASI 7–12 moderate, and PASI < 7 mild chronic plaque psoriasis.
The PASI score is imprecise and there have been various attempts to improve on it. However, it remains the most commonly used assessment of the effectiveness of treatment by its ability to result in 75% or, more realistically, 50% reductions in PASI score at certain timepoints.
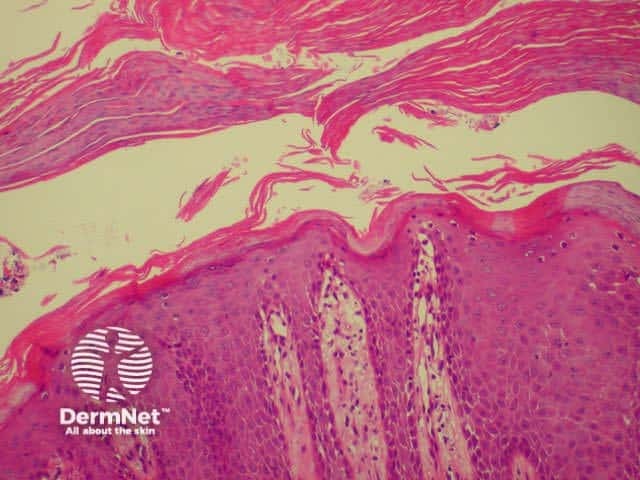
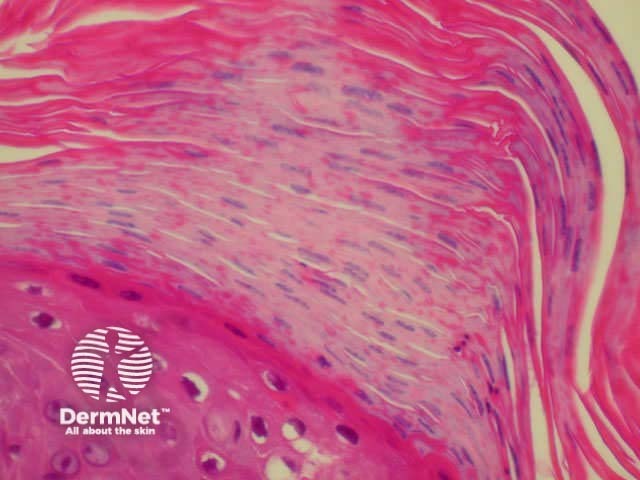
Histology of psoriasis is characterised by parakeratosis (cell nuclei within stratum corneum) and thickened projections of the prickle cell layer of keratinocytes (psoriasiform hyperplasia). There is no granular layer. Polymorphonuclear leukocytes and lymphocytes infiltrate dermis (CD8+) and epidermis (CD4+).
Thick stratum corneum and projections of epidermis Note inflammatory infiltrate Parakeratosis (cell nuclei within thickened stratum corneum) 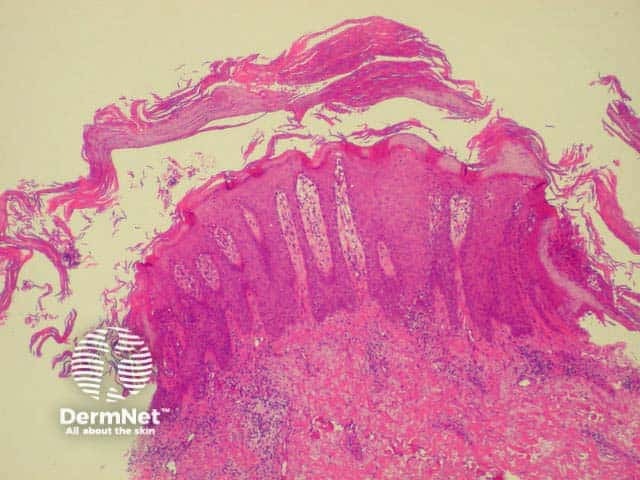
The skin disease may present as one or other form of acute psoriasis, chronic psoriasis or localised to hands and feet. These subtypes may overlap. Types of psoriasis include:
Koebner phenomenon
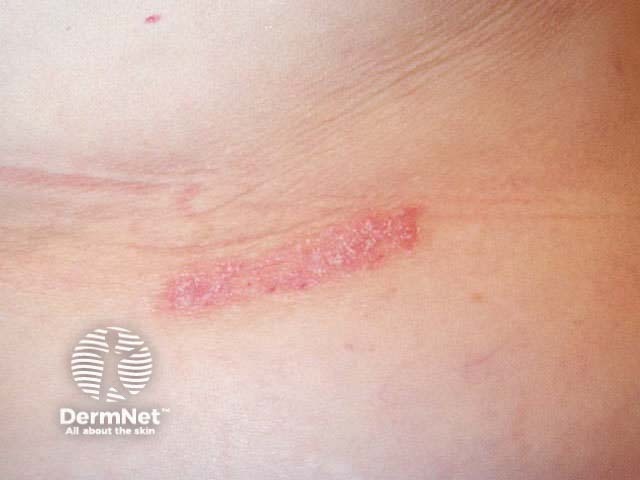

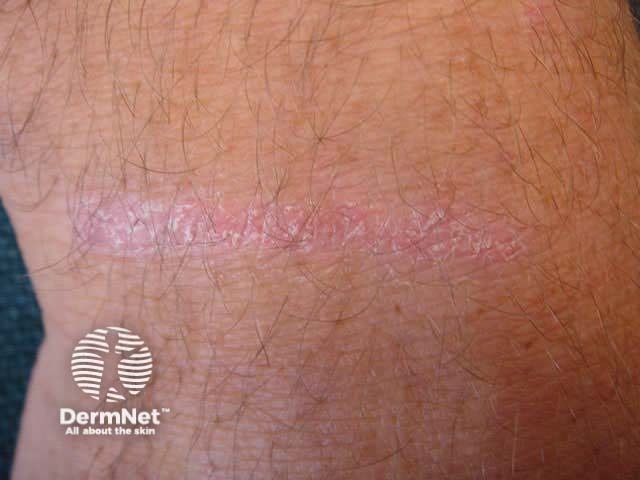
Psoriatic arthropathy
The PASI score is the ‘Psoriasis Area and Severity Index’, and is mainly used for evaluating the effect of interventions in clinical trials. It is calculated as follows:
Plaque psoriasis may be confused with:
Generalised pustular psoriasis may be confused with:
In most cases of psoriasis, no specific investigations are required. However, on occasion the following may be useful:
It is most important to explain the nature of psoriasis to the patient presenting with psoriasis for the first time. Provide them with written material and refer them to DermNet (http://www.dermnetnz.info/) for further information. They need to be aware that there is no known cure and that psoriasis may persist lifelong. Treatment rarely results in complete clearance but reduces the severity and extent of the disease.
Topical agents include:
Phototherapy may include:
Systemic agents include:
Oral corticosteroids are nearly always contraindicated.
Describe the impact of psoriasis on daily living activities and occupation.
Information for patients
See the DermNet bookstore