Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2009.
Note. You should have already read the overview page about psoriasis.
Psoriasis affecting the dorsal or ventral surfaces of the hands and feet may resemble psoriasis in other sites, with well demarcated erythematous scaly plaques. Fissuring can be troublesome.
Chronic plaques of psoriasis Chronic plaques of psoriasis Chronic plaques of psoriasis 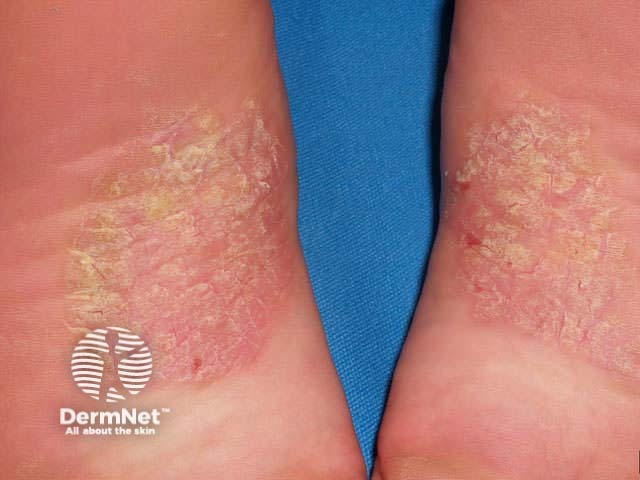
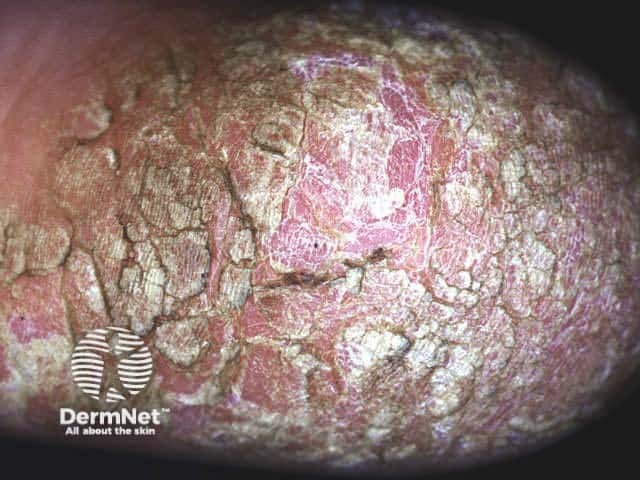
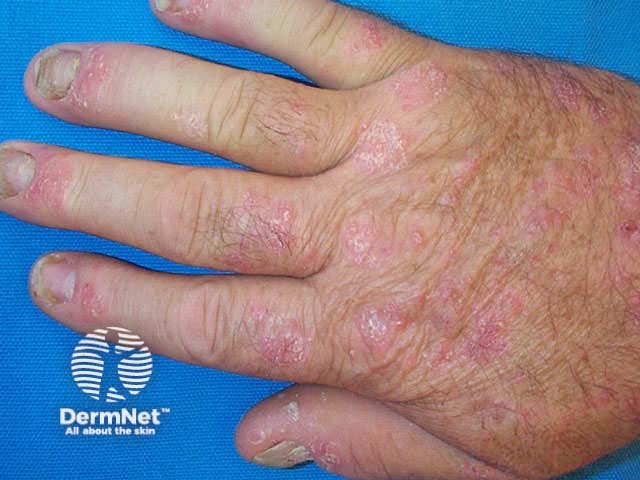
There are also distinct subtypes of palmoplantar psoriasis.
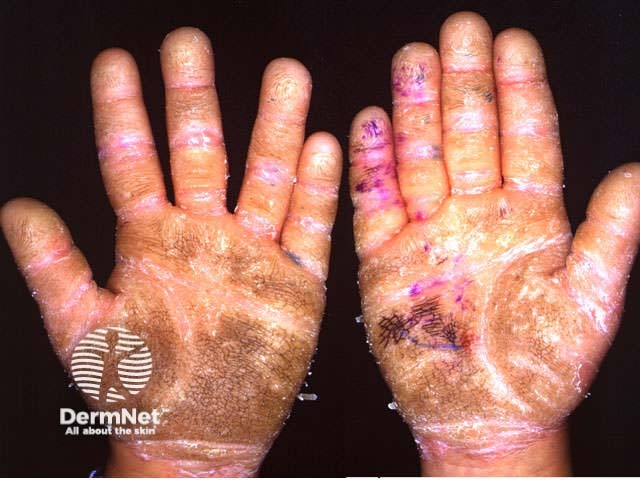
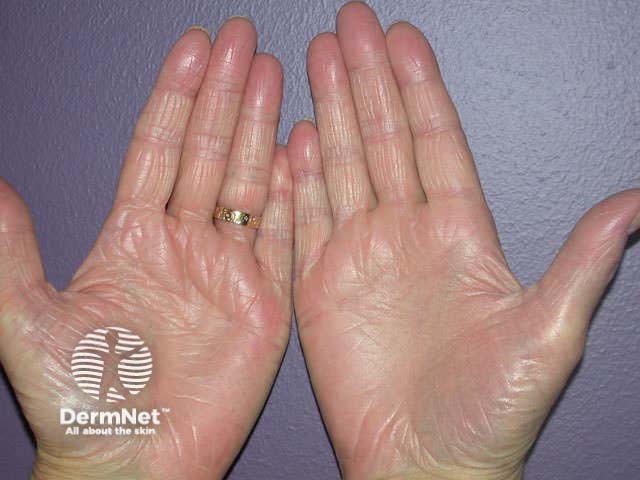
Palmoplantar keratoderma
Keratoderma refers to chronically thickened palms and soles and may be due to various inherited keratin gene disorders and acquired diseases. Psoriatic keratoderma is recognised by:
Keratoderma Keratoderma Keratoderma 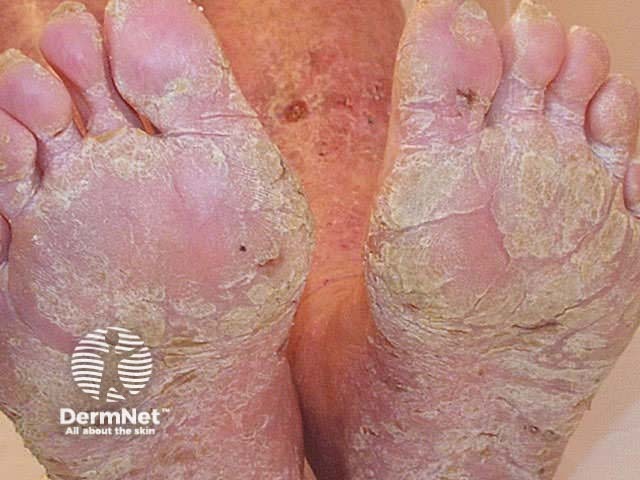
Nail psoriasis
Nails may be the only site affected by psoriasis and is frequently mistaken for onychomycosis (fungal infection), with which it may coexist. It is particularly common in those with psoriatic arthritis affecting the digits. It is usually asymptomatic but may be painful. It is very persistent and resistant to treatment, because it takes a year or so for new cells produced at the matrix to reach the distal edge of the nail plate. Signs affecting one or more nails may include:
Nail psoriasis Nail psoriasis Nail psoriasis Nail psoriasis Nail psoriasis Nail psoriasis 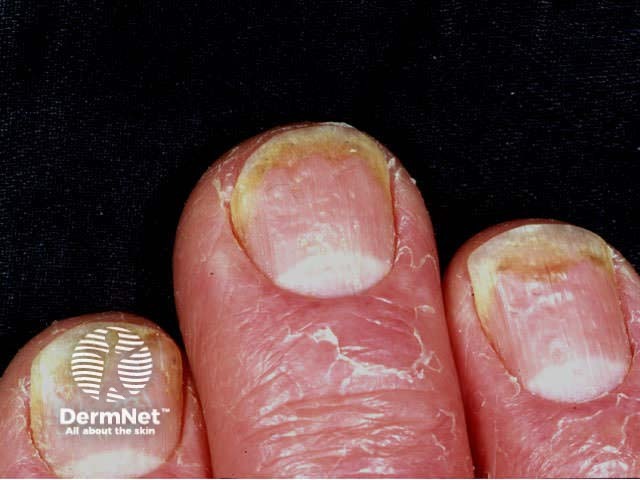
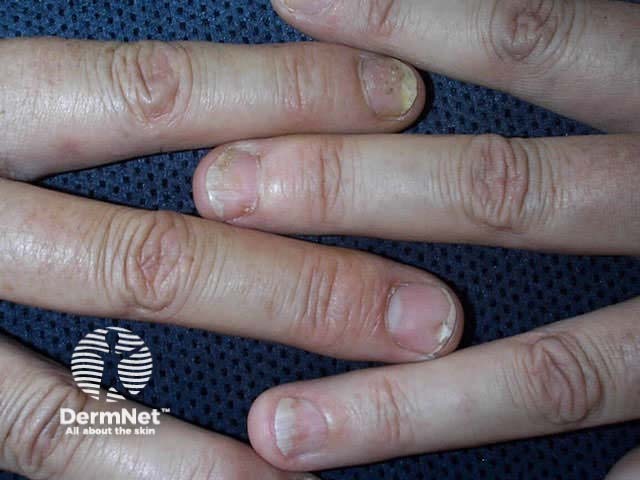

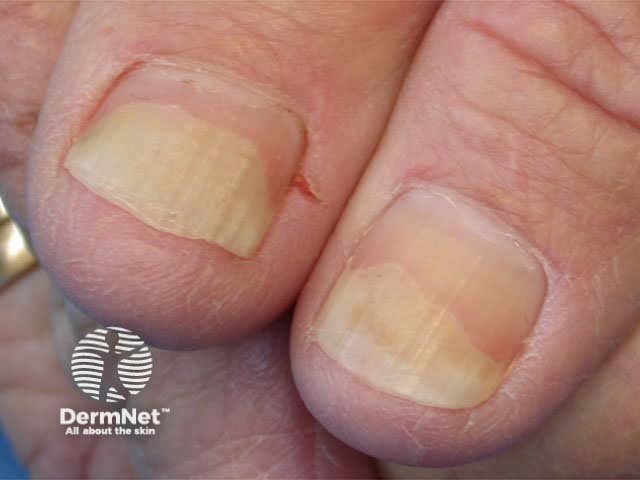
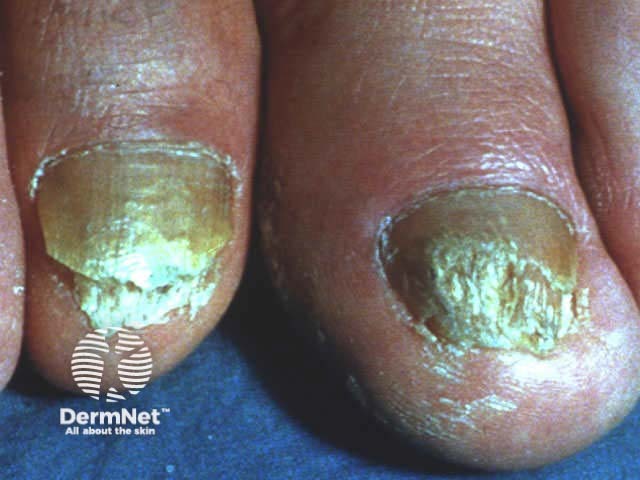
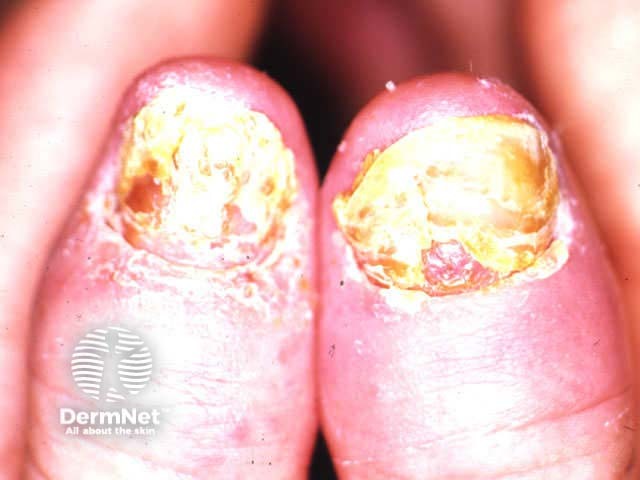
The nail psoriasis index was devised to evaluate the signs of nail psoriasis in each nail separately, each on a 1-3 scale: pitting, Beau's lines, subungual hyperkeratosis and onycholysis in the matrix, the subungual tissues distal to the lunula, or the whole nail unit.
Localised pustular psoriasis
Localised pustular psoriasis affects one or both palms and/or feet. When it arises in the absence of psoriasis elsewhere, it may be called ‘palmoplantar pustulosis’.
Localised pustular psoriasis Localised pustular psoriasis Localised pustular psoriasis 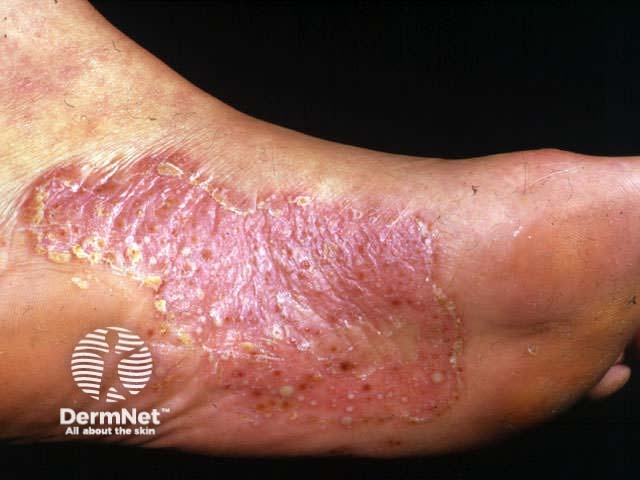
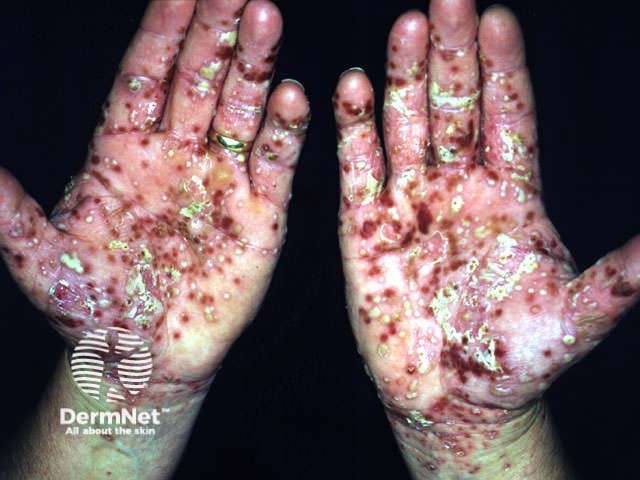
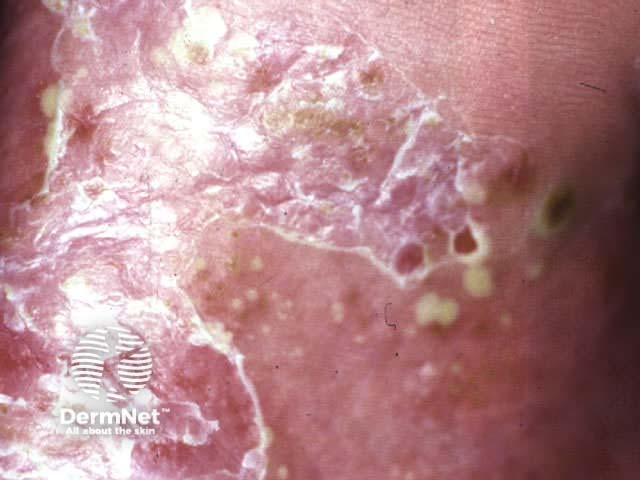
Acrodermatitis continua of Hallopeau
Acrodermatitis continua of Hallopeau is a chronic recurrent pustulation of nail folds, nail bed and distal fingers leading to loss of nails. it may occur alone or in association with chronic plaque psoriasis, psoriatic arthropathy, palmoplantar pustulosis and/or generalised pustular psoriasis.
Acrodermatitis continua 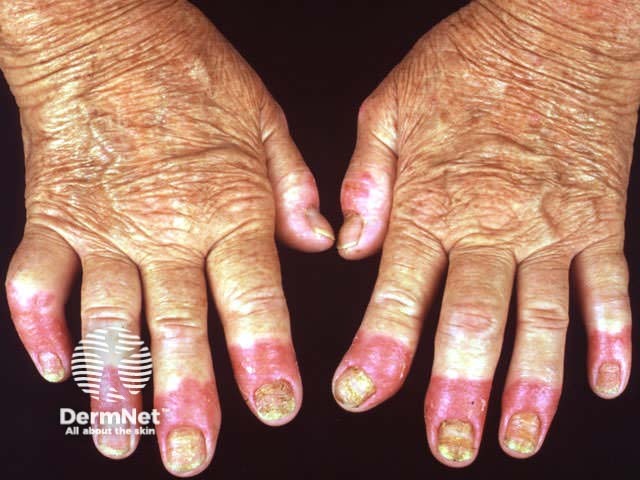
Palmoplantar psoriasis may be confused with:
Localised pustular psoriasis may be confused with:
Investigations indicated in palmoplantar psoriasis may include:
Mild palmoplantar plaque psoriasis is usually managed with topical agents.
Keratoderma is unresponsive to topical steroids and calipotriol. Use emollients that incorporate keratolytic agents such as 5% salicylic acid or up to 40% urea (e.g. heel balm).
Nail psoriasis is very refractory to treatment. Very patient subjects may see results from calcipotriol or fluororuacil solution applied to nail folds and hyponychium twice daily for at least 12 months. Injected triamcinolone acetonide is rarely used because of pain and the potential to cause atrophy. Systemic therapy may be helpful but is rarely warranted for nail disease in the absence of troublesome psoriasis elsewhere.
Palmoplantar pustulosis is usually initially managed with intermittent ultrapotent topical steroids (continuous treatment aggravates the condition), crude coal tar ointment, and/or emollients.
If palmoplantar psoriasis is severe and interferes with function (painful to walk or work), refer to a dermatologist. Do not prescribe oral corticosteroids as these often make the condition worse and more difficult to control by other means. Possible treatments include:
Provide advice about footwear for a patient with plantar psoriasis.
Information for patients
See the DermNet bookstore