Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Actinic keratosis dermoscopy — extra information
Lesions (cancerous) Lesions (benign) Diagnosis and testing
Actinic keratosis dermoscopy
Author: Naomi Ashman, Dermoscopist, Torbay Skin, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. June 2019.
Introduction Clinical features Dermoscopic features Differential diagnoses Histological explanation
What is an actinic keratosis?
Actinic keratosis is a scaly lesion found on sun-damaged skin. It is considered precancerous because a cutaneous squamous cell carcinoma may arise from actinic keratosis. Actinic keratosis is also known as AK and solar keratosis.
What are the clinical features of actinic keratosis?
Actinic keratosis is an irregular, skin coloured, red or pigmented papule or plaque and is most often found on a bald scalp, ear, face or back of the hand. Multiple lesions are often present. Other features may include:
- A white or yellow, scaly, warty or horny surface
- Tenderness.
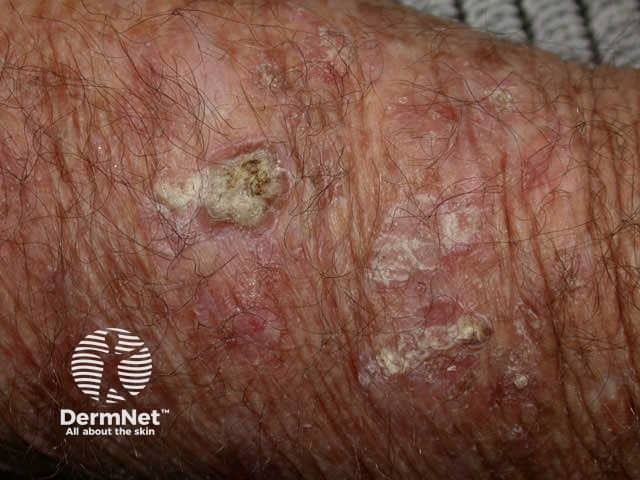
Actinic keratosis
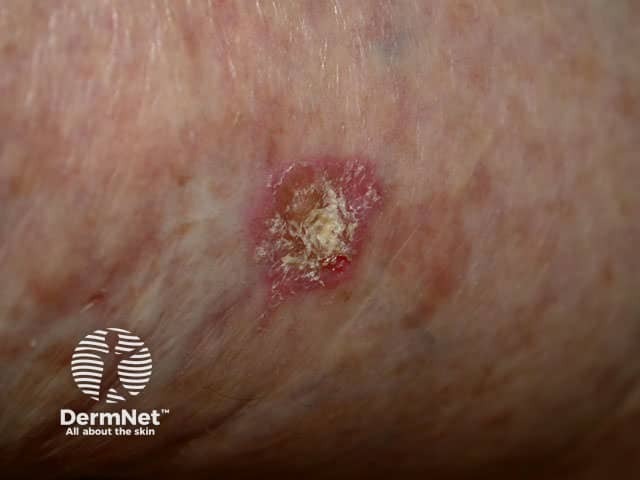
Actinic keratosis
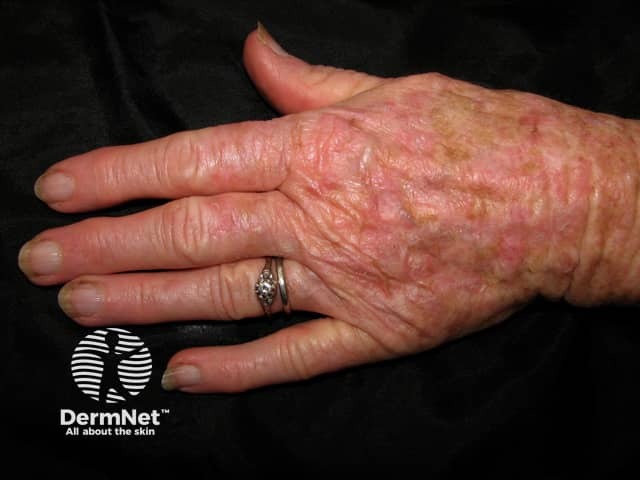
Actinic keratosis affecting a hand
What are the dermoscopic features of actinic keratosis?
Nonpigmented actinic keratosis on the face
Nonpigmented actinic keratosis on the face is characterised by a 'strawberry pattern' on dermoscopy. The border of the lesion is often well demarcated but may merge into surrounding skin as many patients have extensive sun damage. Other features may include:
- A pink, structureless background
- A pink to red pseudonetwork created by straight or wavy vessels surrounding the hair follicles
- Prominent small skin coloured, white or yellowish spots corresponding to follicular openings of variable size.
- Skin coloured or white circles around a yellowish clod (this is a keratotic plug)
- Four dot clods (rosettes) under polarised light
- Surface scale.
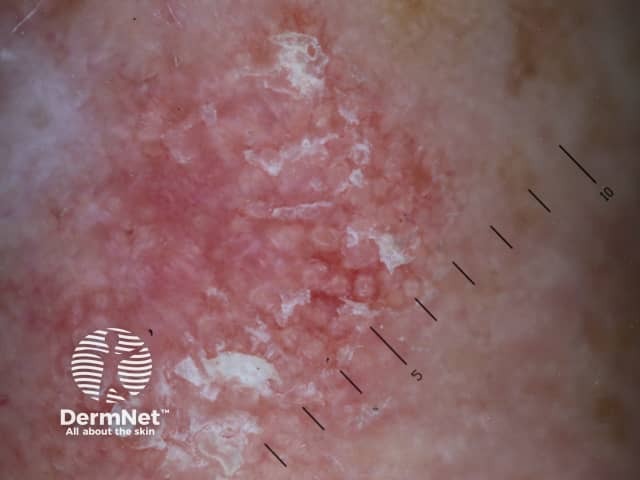
Actinic keratosis affecting the face
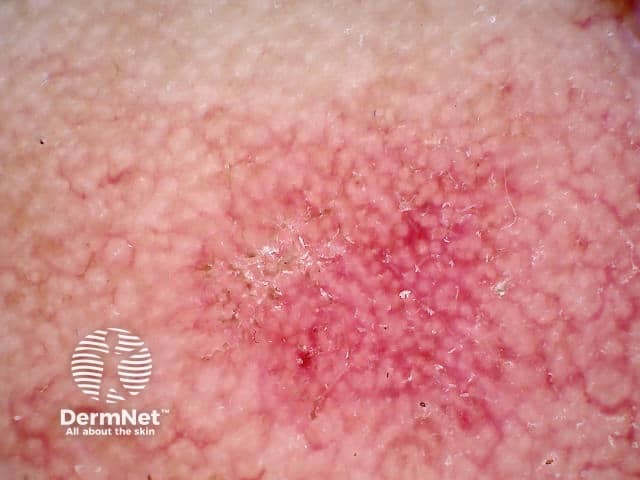
Strawberry pattern dermoscopy of facial actinic keratosis
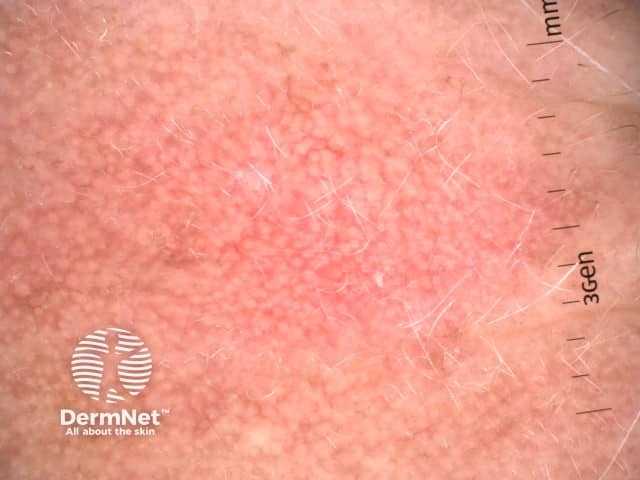
Strawberry pattern dermoscopy of facial actinic keratosis
Nonpigmented actinic keratosis on nonfacial skin
Actinic keratosis on nonfacial skin usually exhibits a nonspecific pattern. Features may include:
- Irregular shape
- Surface scale (white or yellow)
- Sometimes, oyster shell-like concentric yellow structures
- Erythema, sometimes with dotted vessels (tiny crops of red dots)
- Rosettes (polarised light only)
- Short shiny streaks.

Dermoscopy of actinic keratosis on nonfacial skin
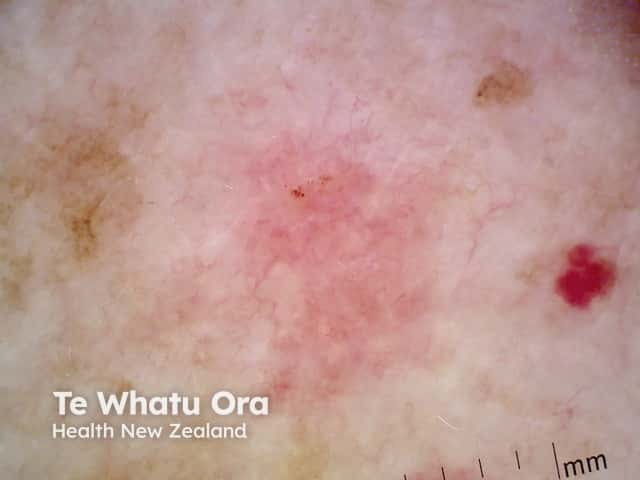
Actinic keratosis on nonfacial skin
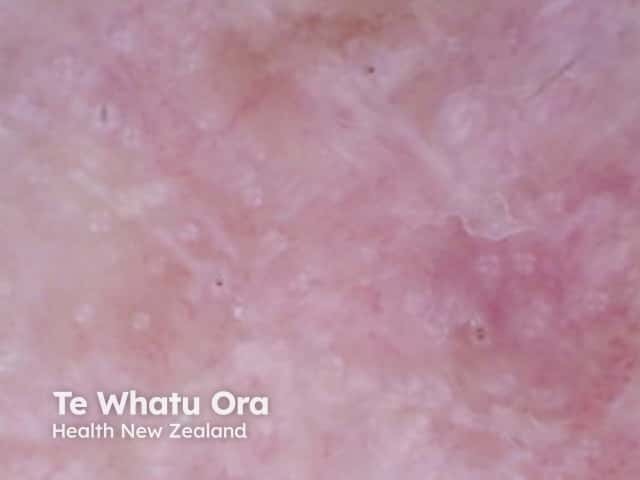
Rosettes in actinic keratosis
Dermoscopic features of pigmented actinic keratosis
Pigmented actinic keratosis has a similar appearance to nonpigmented actinic keratosis with the addition of pigmented structures.
The most common dermoscopic findings are:
- Hyperpigmented follicular openings
- Brown structureless areas
- Annular-granular structures.
Other features include:
- Brown background skin
- Angulated superficial brown lines
- Perifollicular inner grey halo
- Sometimes, grey rhomboidal structures: grey confluent dots arranged in lines or grey-to-brown linear structures located between follicular structures.
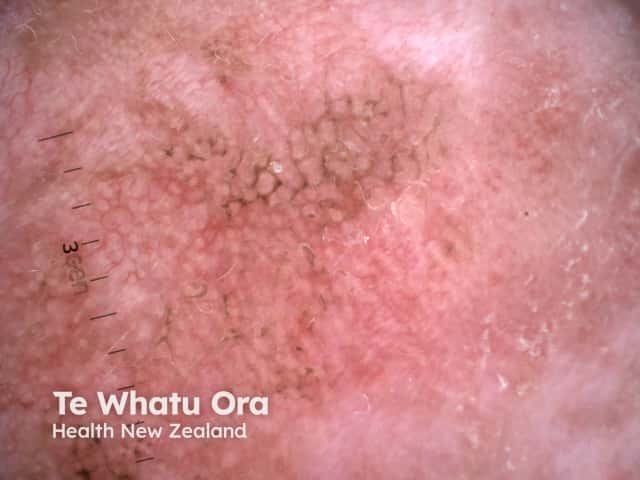
Dermoscopy of actinic keratosis
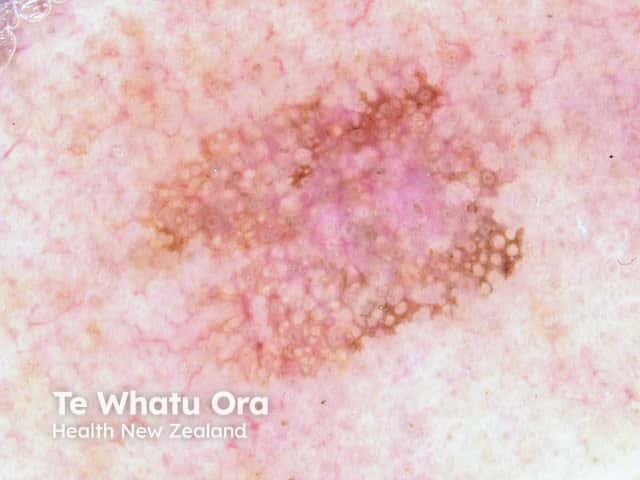
Dermoscopy of pigmented actinic keratosis
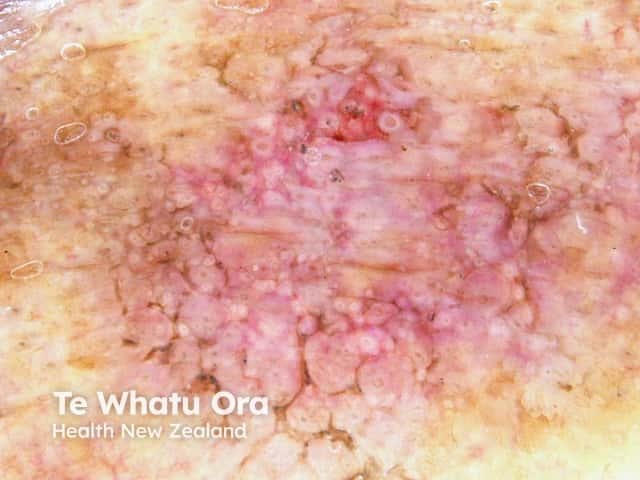
Dermoscopy of pigmented actinic keratosis
What is the dermoscopic differential diagnosis of actinic keratosis?
Actinic keratosis is diagnosed by a combination of clinical and dermoscopic features and sometimes can be difficult to distinguish from other lesions. It may coexist with solar lentigo, cutaneous squamous cell carcinoma, and lentigo maligna.
Cutaneous squamous cell carcinoma
Cutaneous squamous cell carcinoma can arise from actinic keratosis. Differentiation is determined by dermoscopic findings of peripheral white around a central scaly core (the original actinic keratosis).
Squamous cell carcinoma in situ
Dotted/coiled vessels tend to be scattered more randomly in actinic keratosis than in intraepidermal carcinoma where they are arranged in lines or clusters. Vascular structures in squamous cell carcinoma in situ show greater variation in size and structure.
Lentigo maligna
The following four features are significantly associated with lentigo maligna: hyperpigmented follicular openings, obliterated follicular openings, annular-granular structures, and pigmented rhomboids.
Pigmented rhomboids and obliterated follicular openings are significantly more frequent in lentigo maligna than pigmented actinic keratosis.
Lentigo maligna tends to be smooth to the touch, whilst actinic keratosis tends to be rough in texture. The border of lentigo maligna has variable abruptness (fading in some areas, sharp in others) whereas pigmented actinic keratosis tends to have a defined border. Lentigo maligna may have asymmetrical pigmented follicular openings and a darker dot located within ostial openings (a concentric circle or the isobar sign); a finding rarely seen in pigmented actinic keratosis.
Psoriasis
Psoriasis presents with red scaly plaques. Occasionally a solitary plaque of psoriasis may be confused with actinic keratosis. It has a regular structure. The uniform scale tends to be whiter and more silvery in psoriasis compared to the irregular yellowish scale of actinic keratosis. Dotted blood vessels are distributed uniformly throughout the lesion in psoriasis.
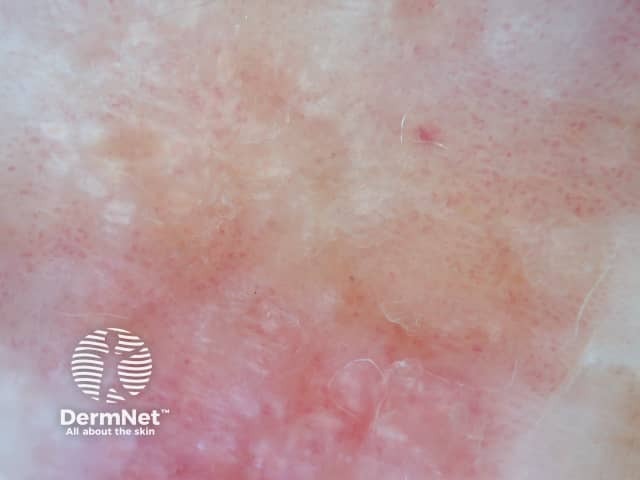
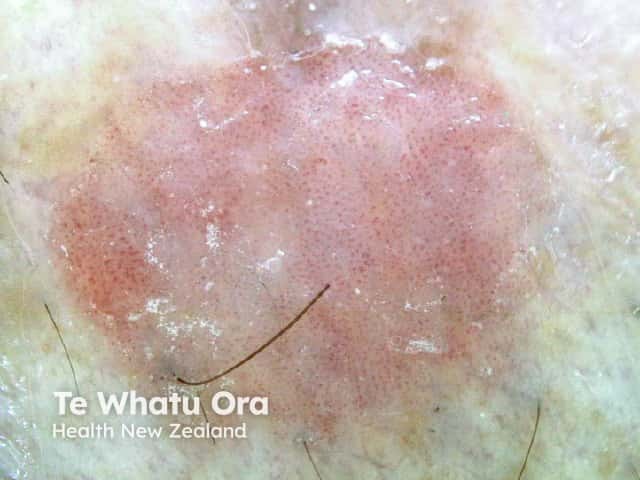
Dermoscopic view of squamous cell carcinoma
Dermoscopic view of squamous cell carcinoma in situ
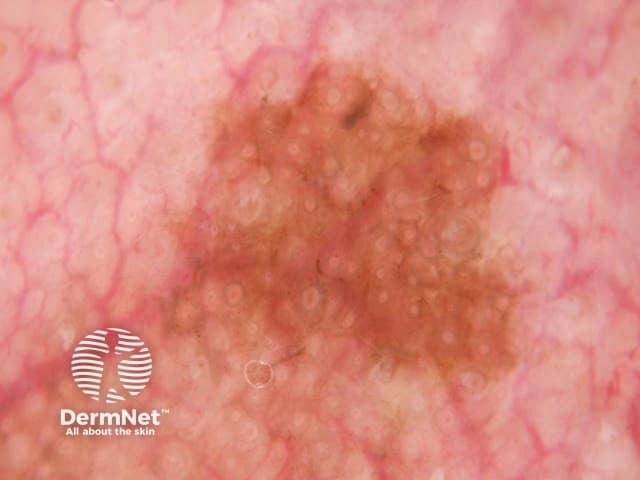
Dermoscopic view of lentigo maligna showing pigmented circles and the isobar sign
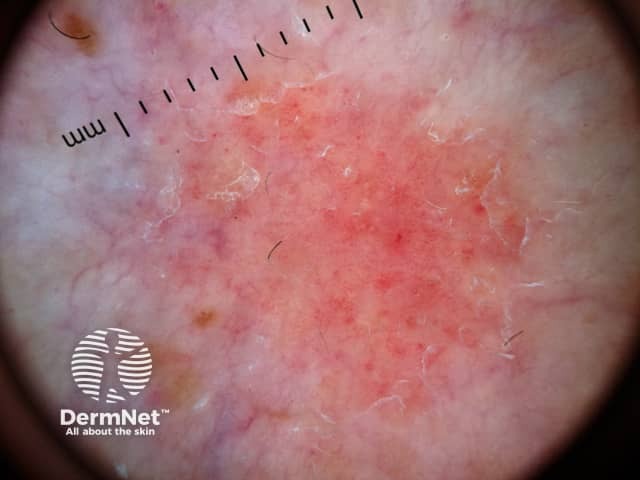
Dermoscopic view of psoriasis
What is the histological explanation for the dermoscopic findings in actinic keratosis?
The correlation between histological and dermoscopic features of actinic keratosis is poor.
Rosettes
The exact histological explanation of rosettes is unclear but they are thought to be due to an interaction between polarised light and narrowed keratin-filled, or fibrotic adnexal openings. Haspeslagh et al found that small rosettes (0.1–0.2 mm) corresponded to concentric horny material in follicular and eccrine ducts at the infundibular level and larger rosettes (0.3–0.5 mm) to perifollicular concentric fibrosis.
Surface scale
Alternating orthokeratosis and parakeratosis.
Strawberry pattern
Vessels between hair follicles, with white haloed follicular openings.
Circles
Circles that appear in pigmented keratosis are due to the involvement of follicular infundibula.
References
- Dermoscopedia
- Pathology outlines: histology of actinic keratosis. Available from: www.pathologyoutlines.com/topic/skintumornonmelanocyticactinickeratosis.html (accessed 10 August 2020)
- Lee DW, Kim DY, Hong JH, Seo SH, Kye YC, Ahn HH. Correlations between histopathologic and dermoscopic findings in Korean actinic keratosis. Microsc Res Tech 2019; 82: 12–17. DOI: 10.1002/jemt.23043. PubMed
- Lozano-Masdemont B, Polimón-Olabarrieta I, Marinero-Escobedo S, Gutiérrez-Pecharromán A, Rodríguez-Lomba E. Rosettes in actinic keratosis and squamous cell carcinoma: distribution, association to other dermoscopic signs and description of the rosette pattern. J Eur Acad Dermatol Venereol 2018; 32: 48–52. DOI: 10.1111/jdv.14474. PubMed
- Lee JH, Won CY, Kim GM, Kim SY. Dermoscopic features of actinic keratosis and follow up with dermoscopy: a pilot study. J Dermatol 2014; 41: 487–93. PubMed
- Costa-Silva M, Calistru A, Barros AM, Lopes S, Esteves M, Azevedo F. Dermatoscopy of flat pigmented facial lesions — the evolution of lentigo maligna. Dermatol Pract Concept 2018; 8: 198–203. Journal.
- Haspeslagh M, Noë M, De Wispelaere I, et al. Rosettes and other white shiny structures in polarized dermoscopy: histological correlate and optical explanation. J Eur Acad Dermatol Venereol 2016; 30: 311–3. DOI: 10.1111/jdv.13080. PubMed
On Dermnet
- Actinic keratosis
- Actinic keratosis affecting the hand images
- Actinic keratosis affecting the face images
- Actinic keratosis affecting the nose images
- Actinic keratosis affecting the scalp images
- Actinic keratosis affecting the legs and feet images
- CME dermoscopy course: dermoscopy of squamous cell carcinoma
