Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Dr Natalie Renaud, Registrar, Sexual Health Services, Waikato District Health Board, Hamilton, New Zealand. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. April 2018.
Introduction
Prevalence
Demographics
Clinical features
Diagnosis
Treatment
Prevention
Chancroid is a sexually transmitted infection (STI) caused by the small fastidious gram-negative bacterium Haemophilus ducreyi (H. ducreyi). It is characterised by painful genital ulcers and painful swollen lymph glands in the inguinal area. Chancroid is different from the non-sexually transmitted skin ulcer disease also caused by H. ducreyi reported in children and young adults in the South Pacific islands.
The incidence of chancroid is unknown because of limitations in the availability of confirmatory diagnostic tests. It is rarely encountered in New Zealand and in most other developed countries where cases are most often related to foreign travel. There have been small outbreaks in the USA and in France. Overall, chancroid is becoming less common, even in endemic areas (Africa, South Asia, Latin America, Caribbean).
Anyone who has sexual contact with an individual infected with H.ducreyi is at risk of developing chancroid. The organism is highly infectious but it does not typically infect intact skin. It is thought that it enters the host through microscopic breaks into the skin during sex. It is more commonly diagnosed in heterosexual men than in women, particularly uncircumcised men.
The time from infection during sexual contact to the onset of signs and symptoms is typically 4–10 days (range 1–35 days). An infected person initially develops one or more red erythematous papules, which quickly evolve to pustules and become larger until they break down into an ulcer. A typical ulcer is deep, has shaggy undermined borders and is very painful. The base of the ulcer has a purulent exudate and bleeds easily.
Chancroid affects the sites most prone to friction during sex. In men, these include the foreskin, the glans and the corona. If left untreated, 50% of cases develop infected lymph glands, which become large, hard painful lumps called buboes on either one or both sides of the groin. Buboes arise about 1–2 weeks after the initial ulcers. Men usually seek medical care for these painful genital lesions. Buboes can burst and discharge pus.
In women, ulcers may be located on the labia, vaginal entrance, cervix, perineum and perianal area. Women generally have nonspecific symptoms such as painful urination or pain on defaecation, vaginal discharge, dyspareunia, and rectal bleeding. Some women are asymptomatic carriers and are unaware of the infection.
Untreated chancroid ulcers may persist for 1–3 months and can result in scarring. They can increase the risk of human immunodeficiency virus (HIV) infection by providing a CD4-rich environment at the point of entry. An atypical presentation can occur in HIV-positive individuals.
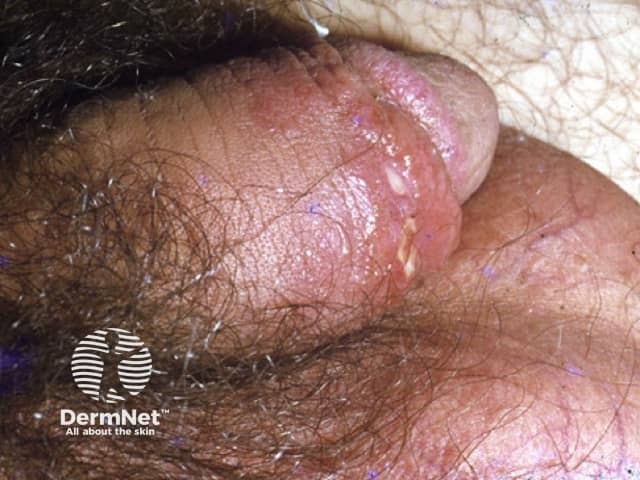
Chancroid
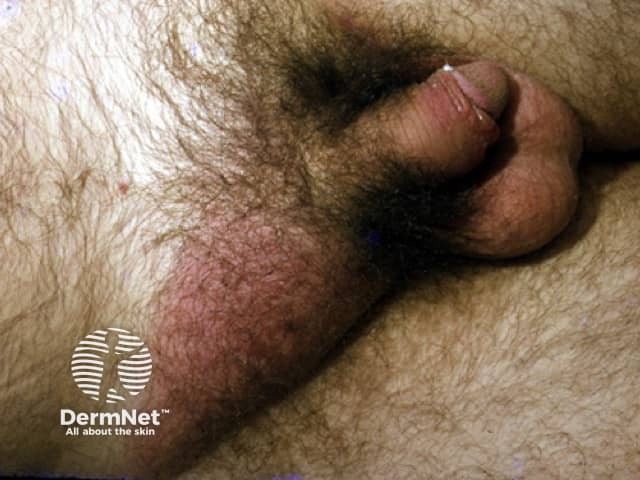
Chancroid
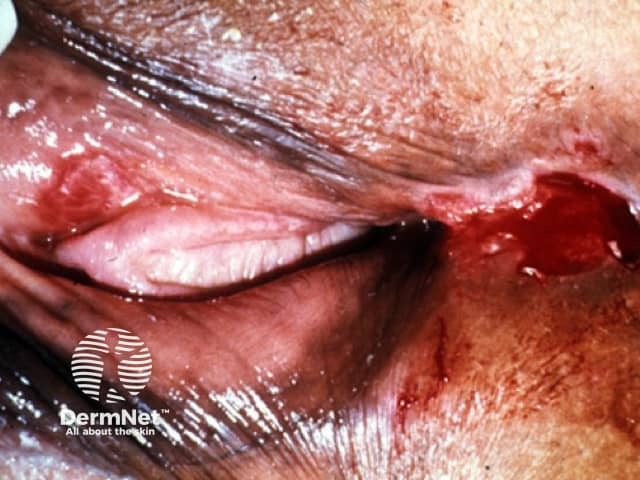
Chancroid
The diagnosis of chancroid is based on the CDC 'probable diagnosis' criteria. The following four criteria are necessary:
Nucleic acid amplification tests (NAAT) are not commercially available even in developed countries. In a research setting, combined NAATs for syphilis (Treponema pallidum), chancroid (H. ducreyi) and herpes simplex virus have been evaluated with high sensitivity (> 95%) and specificity (99%).
A definite diagnosis of chancroid traditionally requires the culture of H. ducreyi from material from the ulcer base on special culture media and under very specific laboratory conditions. The reported sensitivity of culture is 60–80%.
A Gram stain of material from the ulcer base or from buboes can show typical clumping of the causative organism (described as a 'school of fish') but the sensitivity of the test is poor.
No antigen or antibody detection test is in routine clinical use.
Chancroid is treated with antibiotics. The antibiotics of choice are azithromycin, ciprofloxacin, ceftriaxone or erythromycin.
There has been reported resistance to trimethoprim-sulfamethoxazole and to tetracycline. Ciprofloxacin is not recommended in pregnancy and lactation. A single-dose regimen is preferable to increase adherence to treatment (except in immunocompromised individuals). An assessment for the risk of QT prolongation is required if erythromycin is prescribed.
Given that most diagnoses of chancroid are based on clinical criteria and patients may have dual infections, empiric therapy also includes treatment for herpes simplex and syphilis.
Follow-up should continue until the signs and symptoms have completely resolved. Antibiotics result in improvement within 3–4 days and re-epithelisation should be evident by day 7. Time to complete healing depends on the area of skin affected, the presence of buboes, and on the immune status of the infected individual. If healing is delayed beyond 7 days:
An individual with chancroid should not resume any sexual activity until all lesions are completely healed. Sexual contacts need to be notified immediately and treated even if they don't have any signs or symptoms especially if the contact has occurred within the 10 days before the start of chancroid ulceration.
It is important that patients with chancroid undergo a full sexual health screen for other sexually transmitted infections; the sexual health screen should be repeated a few weeks later.
The risk of acquiring chancroid is reduced by safe sex practices including limiting the number of sexual partners, avoiding sexual contact with a high-risk individual, and using condoms.
If you think you are infected, stop all sexual contacts and see your usual doctor or a specialist clinician at a Sexual Health clinic.