Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Reactions Diagnosis and testing
Author: Dr Harriet Cheng, Dermatology Registrar, Waikato Hospital, Hamilton, New Zealand, 2013.
Introduction Histology Special studies Differential diagnoses
Colloid milium is a rare condition characterised by dome-shaped translucent papules and dermal colloid deposition. Four variants are recognised: adult, juvenile, pigmented and nodular colloid milium.
In the papillary dermis, homogenous eosinophilic masses of a colloid are found (figures 1,2,3). Colloid masses are clefted or fissured, and these fissures may be lined with fibroblasts (figure 4 arrow).
In adult-type colloid milium, there is often a grenz zone with subepidermal sparing of the papillary dermis (figure 5 arrow) and solar elastosis. There is sparing of adnexal structures (figure 6).
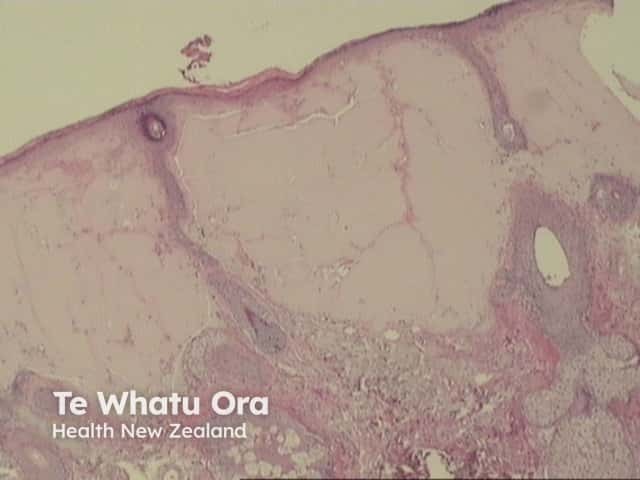
Figure 1
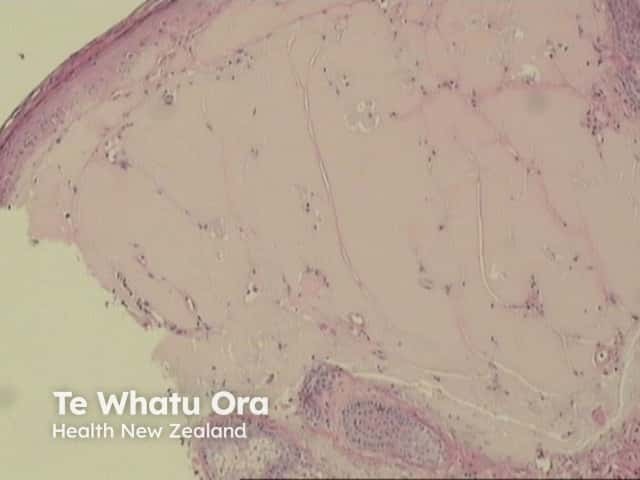
Figure 2
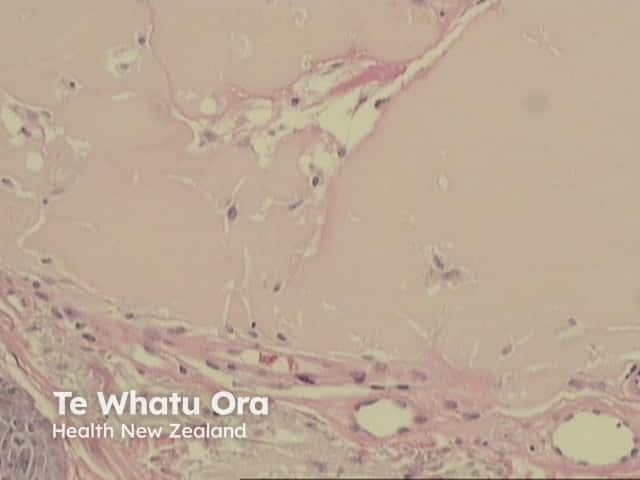
Figure 3
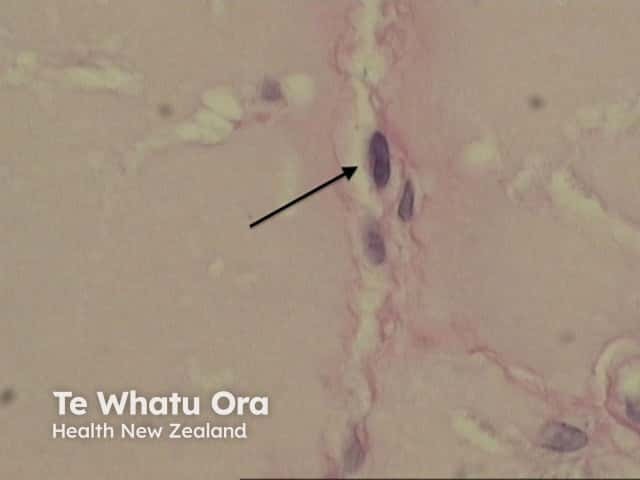
Figure 4
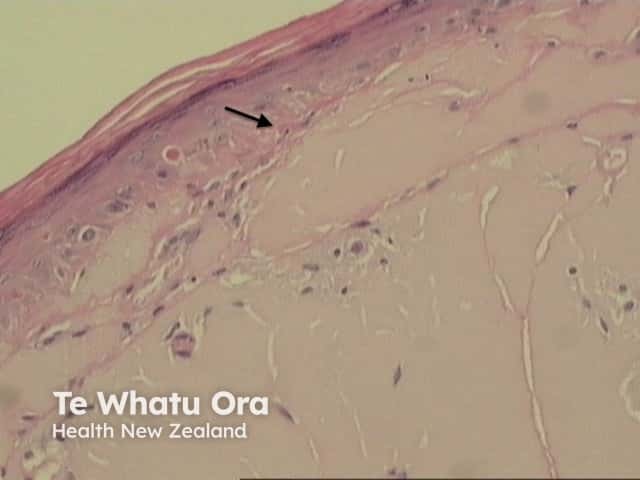
Figure 5
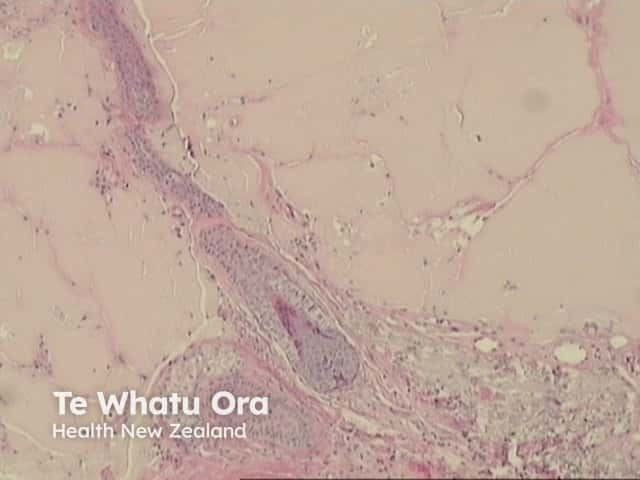
Figure 6
Staining is positive for PAS. Congo red and crystal violet may also be positive.
Primary cutaneous amyloidosis: Differentiation may be difficult and made only by special stains. In contrast to amyloidosis, colloid milium is negative for laminin and type IV collagen. Cytokeratin is positive in lichen amyloidosis and can be helpful in differentiation from colloid milium, which stains negatively; however, nodular amyloid and skin involvement by systemic amyloid are also negative for cytokeratin. Juvenile-type colloid milium may stain positively for cytokeratin and is considered a variant of lichen amyloidosis by some authors. Electron microscopy of amyloidosis reveals straight non-branched filaments whereas colloid milium filaments are shorter, branched and wavy.
Erythropoietic protoporphyria: hyaline deposits are seen around and within superficial blood vessel walls. Involvement of the dermoepidermal junction may be seen (spared in colloid milium).
Lipoid proteinosis: dermal deposits are accentuated around blood vessels. Atrophy of eccrine sweat glands and involvement of pilosebaceous units are additional features. Unlike colloid milium, there is positive staining for laminin, type IV collagen and cytokeratin.
Ligneous conjunctivitis: Juvenile colloid milium has been reported to be associated with this chronic pseudomembranous conjunctivitis. Plasminogen deficiency may be a common causality. Histology of ligneous conjunctivitis reveals thinned or eroded conjunctival epithelium, subepithelial amorphous eosinophilic masses and foci of granulation tissue.