Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Emily Ryder, Dermatology Registrar, Addenbrooke's Hospital, Cambridge, United Kingdom; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand; Copy Editor, Clare Morrison, May 2014.
Introduction
Irritant eyelid contact dermatitis
Allergic eyelid contact dermatitis
Treatment
Eyelid contact dermatitis is an inflammatory reaction involving the eyelid skin that is caused by contact with a trigger substance. It may be due to allergy (allergic contact dermatitis) or irritation (irritant contact dermatitis). Eyelid dermatitis is also called eyelid eczema.
Upper, lower or both eyelids on one or both sides can be affected by contact dermatitis. The patient may report itching, stinging or burning, and the lids are red and scaly. They may swell. With persistence of the dermatitis, the eyelids become thickened with increased skin markings (lichenification). The eyelid margins may become involved (blepharitis). The appearance is similar, whatever the cause.
The thin skin of the eyelids is particularly sensitive to irritants and allergens and is thus prone to develop contact dermatitis. Contact with the same trigger may not lead to a rash on other areas of skin.

Mild chronic eyelid dermatitis
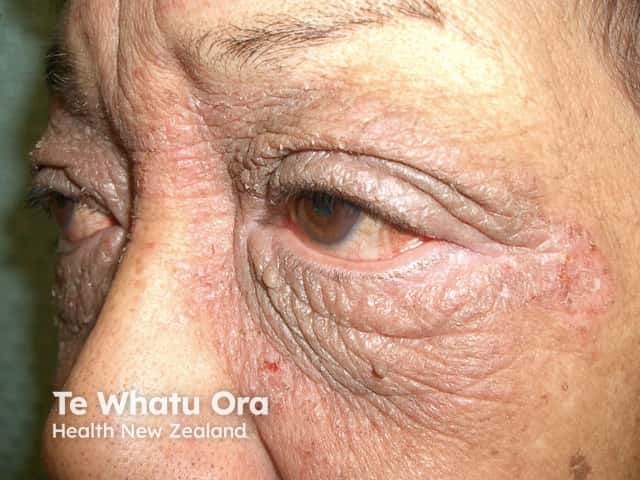
Severe chronic eyelid dermatitis
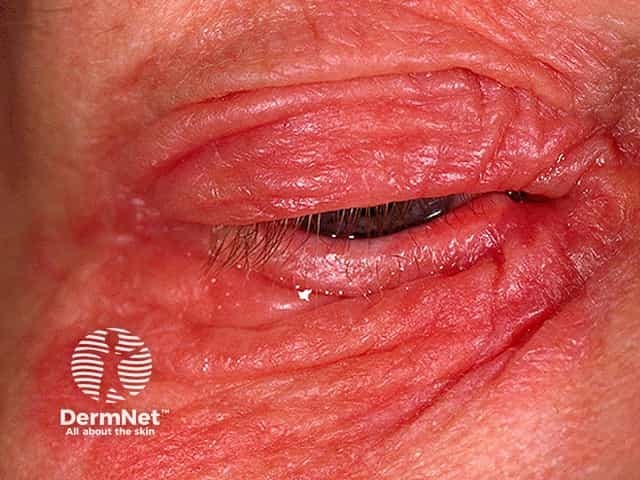
Severe acute eyelid dermatitis
See more images of eyelid contact dermatitis.
Irritant contact dermatitis is an innate inflammatory reaction due to injury to the skin. Unlike allergic contact dermatitis, it does not involve specific antibodies (immunoglobulins) or specific immune cells (memory T cells).
Irritant contact dermatitis may be triggered by contact with irritating substances and/or physical triggers.
Irritating substances that may cause irritant contact dermatitis of the eyelids include:
These substances may touch the eyelids directly or be transferred from the fingers (which may be unaffected by dermatitis).
Physical triggers that may cause irritant contact dermatitis include:
Irritant eyelid contact dermatitis can occur in anyone. However, it is more common in people with sensitive skin. People with a background of atopic eczema, asthma and hayfever ('atopy') are more likely to suffer from irritant contact dermatitis than people without this history.
Any pre-existing inflammation of the skin can cause the skin's waterproof 'barrier' to be compromised and may make it more vulnerable to irritant contact dermatitis. Barrier function may also be defective for genetic reasons.
Diagnosis of eyelid irritant contact dermatitis is made by identifying its characteristic features:
It may be difficult to identify the precise cause.
Allergic contact dermatitis is caused by an immune reaction to the trigger; this is known as the allergen. This is often a substance that the patient has been exposed to many times previously without problem. The rash usually occurs one to several days after the contact with the allergen. This can make it difficult to identify the cause of the dermatitis. Allergic contact dermatitis involves a delayed-type hypersensitivity reaction (also called type IV hypersensitivity) and involves immune memory cells.
Eyelid contact dermatitis follows direct contact with an allergen.
Allergy to cosmetics may be due to contact with allergens in:
Other potential allergens are found in:
Eyelid contact dermatitis may also occur following indirect contact with an allergen, due to transfer of small amounts of substance from the hands (through rubbing or touching the eyelids). Such allergens may include:
Eyelid contact dermatitis is sometimes triggered by airborne allergens, such as dust mite and plant pollens. Compositae allergy is an example of an airborne allergen causing eyelid dermatitis.
Allergic eyelid contact dermatitis can occur in anyone. It is no more likely in those with known sensitive skin or atopic eczema than it is in people that have previously had no skin problem.
Contact allergy usually develops after repeated previous contact with the allergen, so it is not necessarily a new substance that has triggered the allergy.
Diagnosis of eyelid allergic contact dermatitis is made by identifying its characteristic features:
Knowing the details of all substances that the skin may have been exposed to in skin care, hobbies and work are an important part of the detective work required to find the cause of a eyelid dermatitis. Patch tests should be arranged to establish or confirm the triggering allergen.
It is important to avoid contact with irritants and known or potential allergens, to ensure that the skin is healthy and able to form a waterproof barrier.
Short courses of mild topical corticosteroids (ie hydrocortisone 1% cream or ointment) or calcineurin inhibitors (ie pimecrolimus 1% cream) may be required to treat active inflammation. Severe contact dermatitis of the eyelids is usually treated with a short course of oral corticosteroids.
Eyelid dermatitis can be followed by postinflammatory pigmentation, one of the causes of dark circles under the eyes.