Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Jacqueline K. Nguyen, St Vincent’s Hospital, Melbourne, Australia (2023)
Previous contributors: Dr Delwyn Dyall-Smith, Dermatologist (2011)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Familial cold autoinflammatory syndrome (FCAS) is a rare autosomal dominant autoinflammatory disease that presents with episodic rash, fever, arthralgias, and fatigue upon generalised exposure to the cold.
FCAS is also known as familial cold urticaria or familial polymorphous cold eruption. It belongs to the spectrum of cryopyrin-associated periodic syndromes (CAPS) or NLRP3-associated autoinflammatory diseases (NLRP3-AIDS), along with Muckle-Wells syndrome (MWS) and neonatal onset multisystem inflammatory disease (NOMID) / chronic infantile neurological cutaneous and articular syndrome (CINCA).
FCAS is the mild phenotype compared to MWS (moderate phenotype) and NOMID/CINCA (severe phenotype).
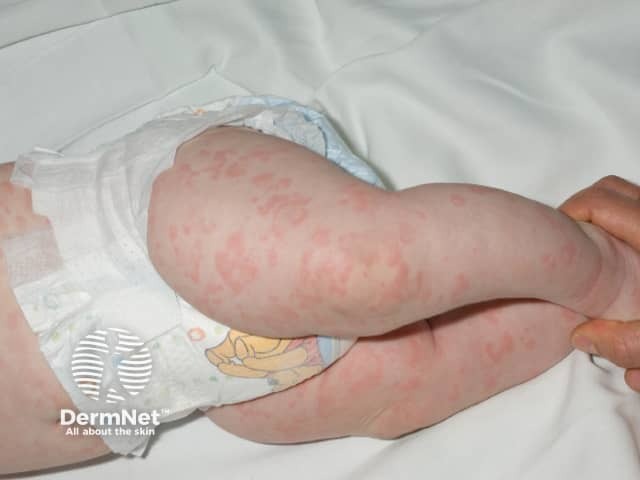
Transient annular macular erythema 2 hrs after cold exposure
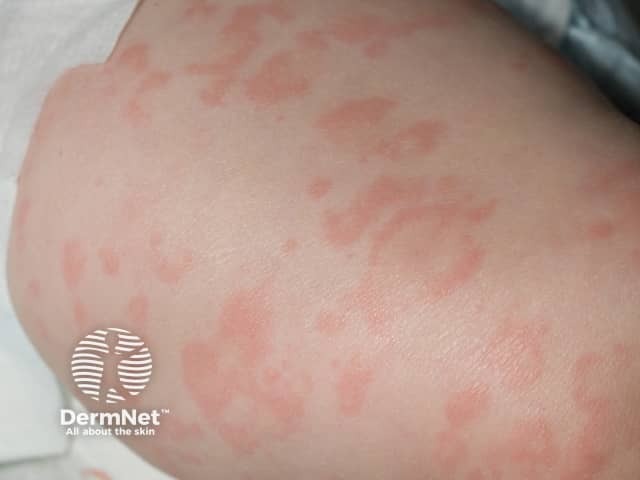
Close up of transient annular macular erythema 2 hrs after cold exposure
FCAS is inherited in an autosomal dominant pattern. Children of an affected parent have a 50% chance of inheriting the disease.
Onset of symptoms has been reported from birth. The mean age of presentation is 47 days old, and 95% of affected individuals present by 6 months of age. In rare cases, symptom onset may occur during young adulthood. FCAS is a lifelong condition.
FCAS is extremely rare with an estimated prevalence of 1:1,000,000. It is primarily reported in families of North American and European descent and is seen equally in females and males.
FCAS results from a gain of function mutation in the NLRP3 gene which encodes cryopyrin on chromosome 1q44. This leads to the activation of the cryopyrin inflammasome, causing uncontrolled inflammation through the inappropriate release of cytokines including interleukin 1-beta (IL-1β). This results in the inflammatory symptoms of FCAS.
Generalised cold exposure is a trigger for the symptoms of FCAS. The mechanism of temperature dependence is still being studied, but monocytes in patients with FCAS showed enhanced release of cytokine IL-1 on exposure to subnormal temperatures.
FCAS is characterised by acute, episodic attacks of fever with rash following generalised exposure to cold. The average delay from cold exposure to onset of symptoms is 2.5 hours. Episodes usually last less than 24 hours (on average ~12 hours) and settle spontaneously.
Clinical features of an acute episode may include:
Diagnosis of FCAS is primarily clinical, based on a history of episodic febrile attacks and rash following generalised cold exposure.
Due to the autosomal dominant inheritance pattern, diagnosis can be accelerated by monitoring children with a known family history of FCAS.
Genetic testing can be performed by NGS (next-generation sequencing) or Sanger sequencing to detect mutations in the NLRP3 gene.
Laboratory findings may include:
Skin biopsy shows dermal oedema with neutrophil infiltration in the dermis, particularly perivascular and peri-eccrine.
Interleukin 1 (IL-1) blocking therapy is now the recommended standard of care for FCAS. These biological treatments block the effect of IL-1β on the IL-1 receptor, inhibiting downstream signalling which reduces systemic inflammation and improves symptom control. Dosing requirements may vary depending on severity of disease.
Currently available IL-1 blockers (given by subcutaneous injection) include:
FCAS is a lifelong condition with good long-term prognosis. Patients can be monitored for the rare development of amyloidosis and renal failure by monitoring for proteinuria and microalbuminuria. While the episodic attacks of FCAS can affect quality of life, treatment with IL-1 blockers has greatly improved outcomes for patients with cryopyrin-associated periodic syndromes (CAPS).