Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Ian Coulson, East Lancashire NHS Trust, UK. Copy edited by Gus Mitchell. January 2022
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Ichthyosis prematurity syndrome is a rare autosomal recessive genetic skin disorder in which affected infants are born prematurely with abnormal skin covered in a thick clay-like vernix.
Their mothers usually develop polyhydramnios, which can precipitate premature labour, and after birth, the affected infant often develops severe, temporary respiratory failure. If the infant survives, the skin may remain red and slightly scaly for the rest of its life.
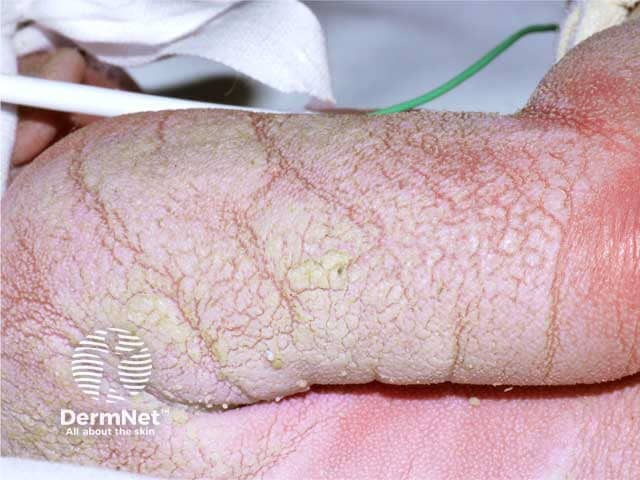
Ichthyosis prematurity syndrome skin at 48 hrs of life
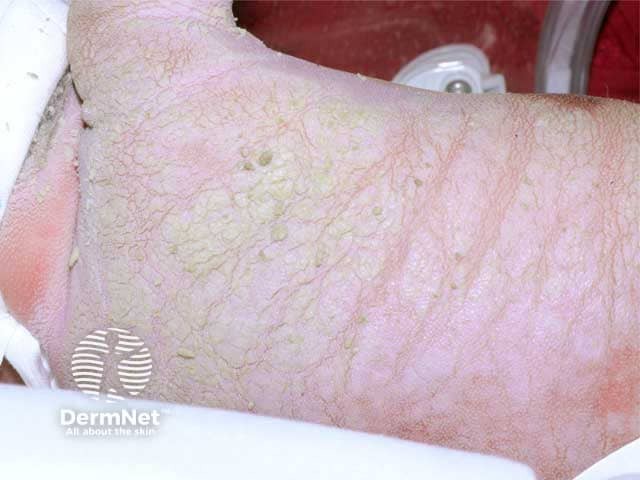
Ichthyosis prematurity syndrome - thick hyperkeratotic skin over the back at 48 hrs of life
Ichthyosis prematurity syndrome is a rare condition with less than 100 affected individuals reported worldwide.
Being recessively inherited, both parents must carry a copy of the defective gene in order for this recessive disorder to manifest. Clusters of cases have been reported from Ireland and Scandinavia.
Ichthyosis prematurity syndrome is caused by mutations of the SLC27A4 gene that codes for the fatty acid transport protein 4 (FATP4), which is responsible for skin barrier function during the embryonic and neonatal period.
This mutation results in abnormal desquamation of keratinocytes into the amniotic fluid, causing polyhydramnios. Aspiration of the excessive amniotic keratinocyte debris into the lungs results in temporary respiratory failure in the days after delivery.
Skin changes lessen rapidly, and during later childhood and adulthood, there may be mild ichthyosis and follicular hyperkeratosis.
The clinical appearance at birth is characteristic even though it is rare. Specific diagnostic tests include:
The clinical appearance is unique but other inherited skin conditions may need consideration, such as:
Subsequent pregnancies require expert obstetric care and ultrasound observation of the amniotic fluid. Affected babies should be delivered with ventilatory support available.
An affected individual may continue to have dry skin and follicular ichthyosis into adult life. There is a higher incidence of atopic conditions (asthma, eczema, and hay fever).