Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Riyad N.H. Seervai and Claire Jordan Wiggins, Medical Students, Baylor College of Medicine, Houston, Texas, USA. Medical Editor: Dr Helen Gordon, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. July 2020.
Introduction Causes Demographics Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Epidermolytic ichthyosis is one of the five main types of ichthyosis along with lamellar ichthyosis, ichthyosis vulgaris, congenital ichthyosiform erythroderma, and X-linked ichthyosis.
It typically presents at birth with erythroderma, skin fragility, and blistering [1–3].
Epidermolytic ichthyosis was formerly known as epidermal hyperkeratosis and bullous congenital ichthyosiform erythroderma.
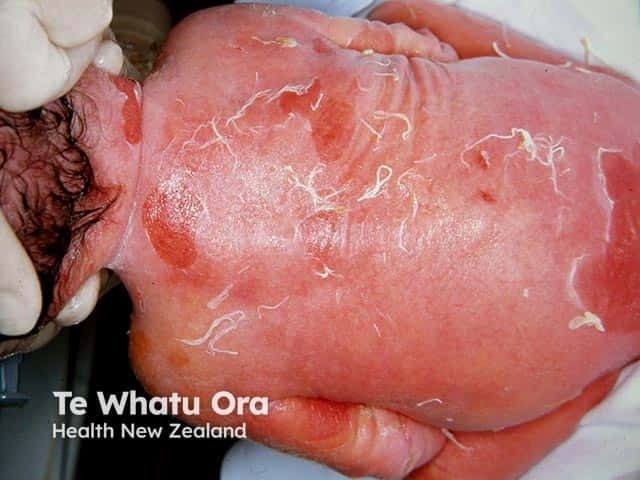
Denuded areas of skin on the back with erythroderma in a neonate with bullous ichthyosiform erythroderma (KI-patient1)
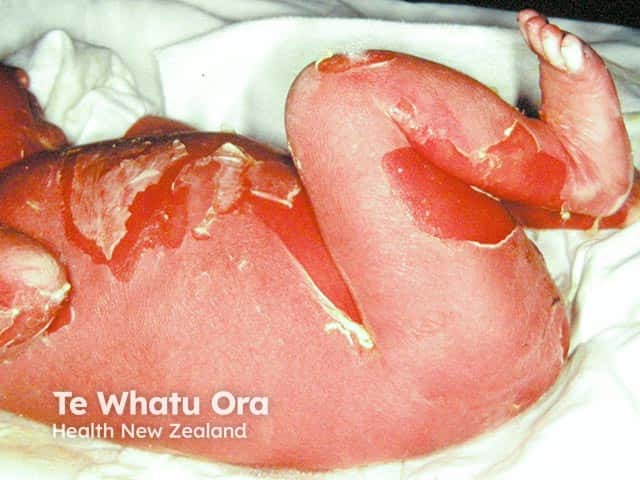
Denuded areas of skin on the legs and abdomen with erythroderma in a neonate with bullous ichthyosiform erythroderma (KI-patient1)
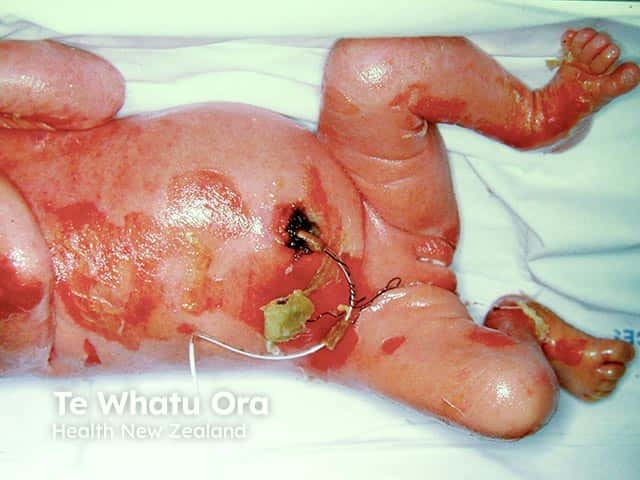
Denuded areas of skin on the abdomen and legs with erythroderma in a neonate with bullous ichthyosiform erythroderma (KI-patient1)
Epidermolytic ichthyosis is caused by missense mutations (where a single nucleotide is changed) in the keratin genes keratin 1 (KRT1) [4,5] and keratin 10 (KRT10) [5–7].
Keratin tonofilaments consist of keratin 1 (K1) and 10 (K10) and are a robust structural component of the flattened squamous keratinocytes in the superficial epidermis [10–12].
Mutations in KRT1 and KRT10 lead to variable disruption and decreased stability of the K1/K10 tonofilaments and hyperkeratosis due to lack of desquamation [13,14].
Epidermolytic ichthyosis is a rare disorder seen to affect 1 in 100,000–300,000 infants in males and females equally [1–3].
Epidermolytic ichthyosis is the only keratin disease associated with genetic mosaicism; the offspring of parents with epidermolytic epidermal naevi can develop generalised epidermolytic ichthyosis if the gonads are involved [17,19].
The clinical features of epidermolytic ichthyosis are [1–3]:
Common symptoms are anhidrosis, pruritus, fissuring, and decreased joint mobility.
Hair, nails, and mucosal surfaces are usually not involved.
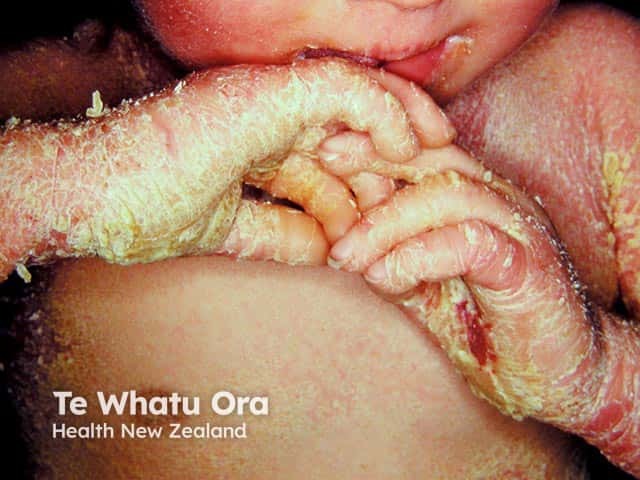
Severe palmar keratoderma and extensive scaling over the chest in a baby with bullous ichthyosifrom erythroderma (KI-patient2)
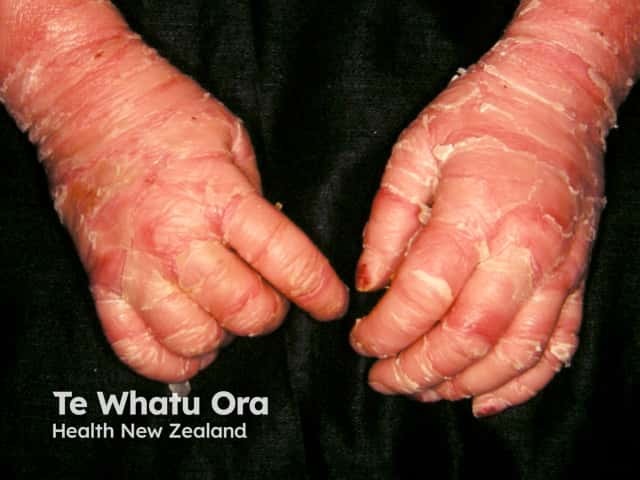
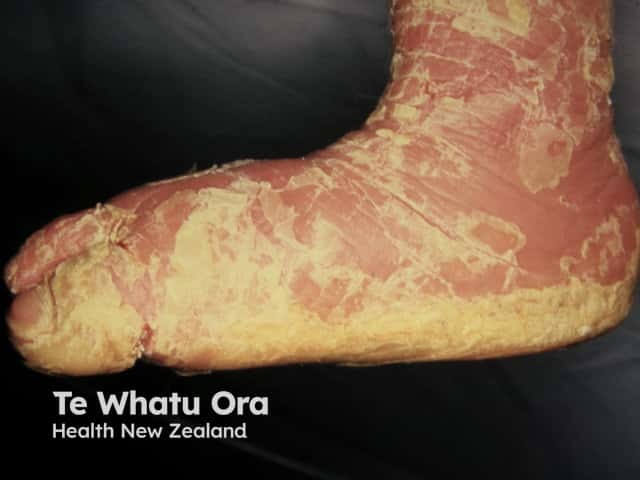
Complications of epidermolytic ichthyosis are due to the impaired skin barrier function [2,3].
Epidermolytic ichthyosis is associated with atypical naevi [18]. There are also reports of palmoplantar contractures [20].
Given the similarities between various ichthyoses, a diagnosis of epidermolytic ichthyosis can be made using clinical, histopathological, and laboratory findings. The diagnosis can be confirmed with genetic testing [1–3].
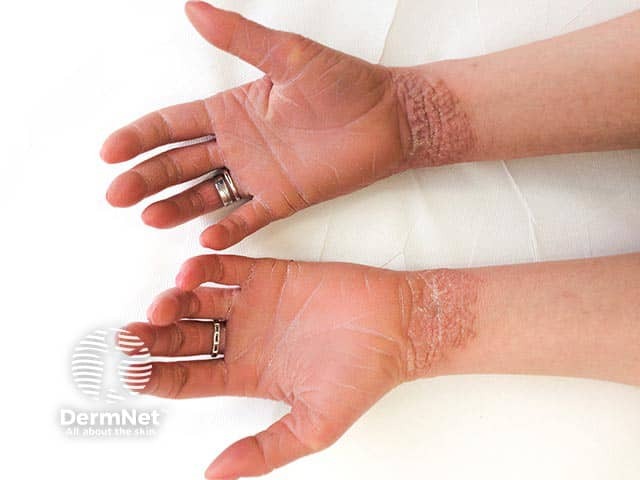
Localised dry hyperkeratotic plaques on the wrists in an adult with bullous ichthyosiform erythroderma (KI-patient3)
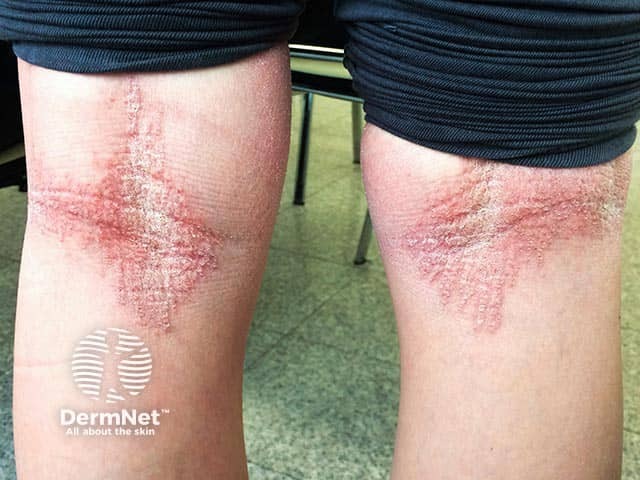
Localised dry hyperkeratotic plaques in the popliteal fossae in an adult with bullous ichthyosiform erythroderma (KI-patient3)
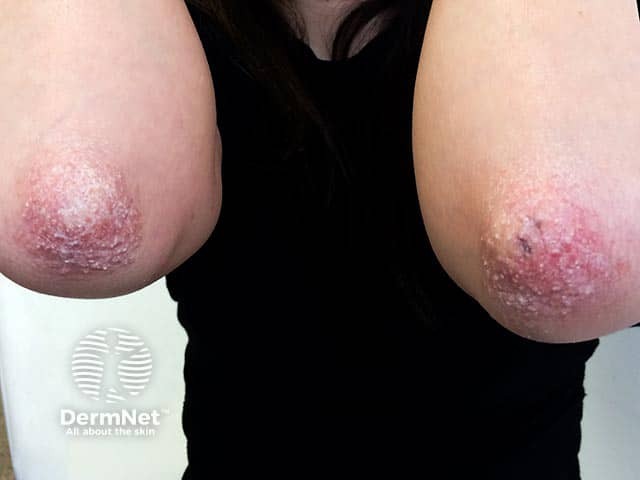
Localised dry hyperkeratotic plaques on the elbows in an adult with bullous ichthyosiform erythroderma (KI-patient3)
The differential diagnosis for epidermolytic ichthyosis includes other congenital ichthyoses, vesiculobullous and erosive disorders, and syndromic genodermatoses [2,3].
Other congenital ichthyoses can be a differential diagnosis to epidermolytic ichthyosis include:
Vesicobullous and erosive disorders that could be a differential diagnosis to epidermolytic ichthyosis include:
Syndromic genodermatoses that can be a differential diagnosis to epidermolytic ichthyosis include:
There is no cure for epidermolytic ichthyosis, and treatments are limited to management of symptoms depending on the age and sex of the patient, severity of the disease, and location of the skin lesions [2,3]. These include:
Retinoids are used to prevent hyperkeratinisation and superinfection in severe cases and have been found to be more effective in patients with KRT10 mutations [21,22]. However, retinoids can paradoxically increase skin fragility and blistering and must be used with caution and careful monitoring [23].
The prognosis of epidermolytic ichthyosis is variable and depends on the severity of the symptoms. There is an immediate risk of dehydration, infection, sepsis, and premature death. Patients who survive experience infection, skin fragility, and blistering episodes throughout their lives, in addition to stress and social isolation accompanying these symptoms [1,2].
Gene therapy has been demonstrated to be effective in improving tonofilament stability in KRT10 mutant primary keratinocytes [24] and remains the best hope for these patients.