Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Tom Moodie, Dermatology Registrar, Waikato Hospital, Hamilton, New Zealand, 2013. DermNet Revision September 2021
Introduction
Clinical features
Diagnosis
Bacterial causes
Fungal panniculitis
Viral panniculitis
Panniculitis of the skin is inflammation of the subcutaneous fat. It has many causes. An infective cause is more likely in those with immunodeficiency (a weakened immune system).
Immunodeficiency may be due to disease, such as infection with human immunodeficiency virus (HIV), or drug-induced immunosuppression (eg, prescribed after organ transplantation). Immunodeficiency may lead to infection with unusual organisms in unusual sites, including the subcutaneous fat.
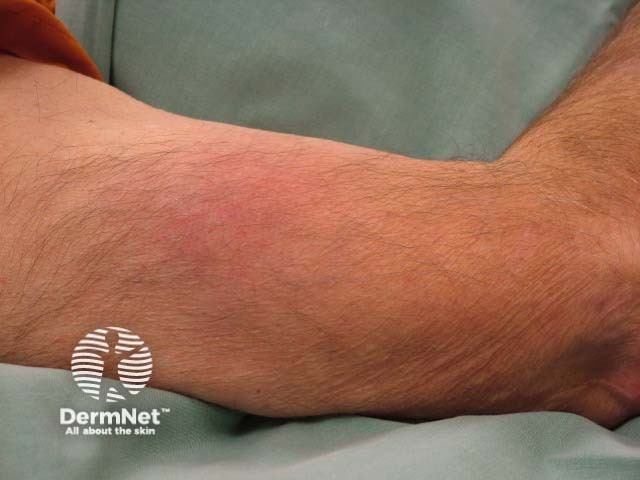
Staphylococcus
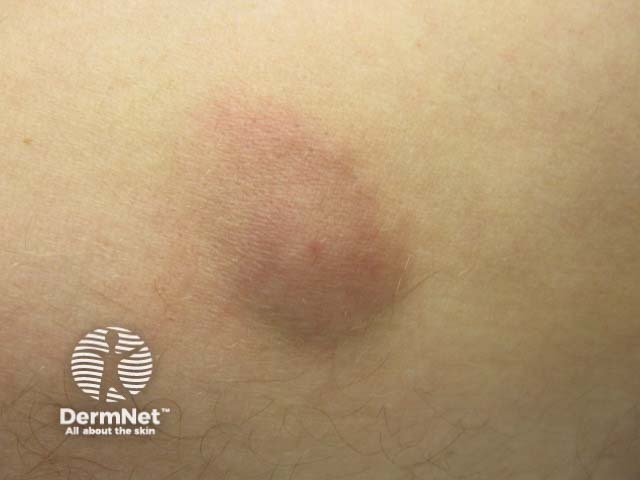
Atypical mycobacterium
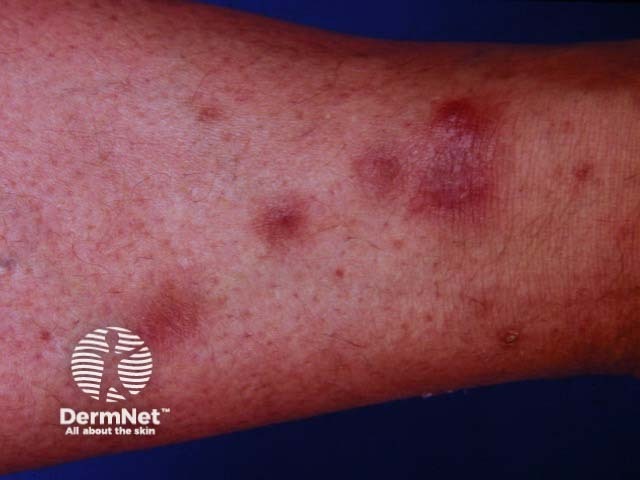
Cause unknown
Infective panniculitis, in general, has no specific features. The clinical presentation depends on:
Whilst history is important, the diagnosis usually requires microbiological and histological confirmation. On biopsy, most infectious panniculitis causes a lobular pattern of inflammation. A lobular pattern is nonspecific although there are sometimes clues that an organism is responsible. Cultures and special stains are required to distinguish these.
Common bacteria that cause panniculitis include:
Bacterial panniculitis can appear in immunocompetent as well as immunosuppressed individuals. It can develop as a result of direct inoculation or from seeding from systemic infection.
The classical histopathological appearance is a lobular or mixed lobular/septal suppurative panniculitis with heavy infiltrate of neutrophils.
The choice of antibiotic treatment depends on the specific bacteria identifed. If the microorganism is unknown, a broad-spectrum antibiotic such as amoxicillin-clavulanic acid is often chosen.
Mycobacteria have a wide range of skin manifestations and panniculitis is uncommon. Most mycobacterial panniculitis is due to atypical mycobacteria including:
Mycobacterial panniculitis is most frequently seen in immunocompromised individuals spreading through the bloodstream to present as widespread skin lesions. Trauma is the usual means of inoculation in individuals with a normal immune system and results in a single lesion.
Histology demonstrates lobular panniculitis, sometimes with granuloma formation. Zeihl-Neelson, auramine-rhodaine or Fite-Faraco stains are specialised mycobacterial stains that help highlight the organism. Cultures are more sensitive and allow for accurate identification of the mycobacterial species but can take many weeks. DNA probes and DNA PCR are quick ways of species identification.
Treatment regimes are specific to the species of mycobacteria. Treatment is usually continued for 6–12 months or at least 6–8 weeks after clinical resolution.
Treatment of cutaneous non-tuberculous mycobacterial infection |
||
|---|---|---|
Micro-organism |
First Line |
Other treatment options |
M. chelonae |
Clarithromycin + ciprofloxacin/doxycycline |
Surgical debridement |
M. fortuitum |
Amikacin + ciprofloxacin/doxycycline |
Surgical debridement |
M. abscessus |
Clarithromycin + amikacin/cefoxitin |
Surgical debridement/excision |
M. marinum |
Ethambutol + rifampicin or doxycycline |
Surgical debridement |
M. avium-intracellulare |
Ethambutol + clarithromycin + rifampicin |
Surgical excision |
Fungal panniculitis can be separated into disseminated disease or classical subcutaneous mycosis.
Biopsy, fungal culture and specific histology stains (silver-impregnated procedure and periodic acid-Schiff) are required to make the diagnosis.
Treatment of fungal panniculitis depends on the identification of the organism.
Features of deep fungal infections |
||
|---|---|---|
Disseminated fungal disease |
Classical subcutaneous mycosis |
|
Causative organisms |
Candida spp, Aspergillus spp, Fusarium spp, Histoplasma capsulatum |
[Sporotrichosis] |
Patient characteristics |
Immunosuppressed individuals |
A healthy individual directly inoculated by soil, plant, or wood |
Clinical manifestations |
Multiple inflammatory subcutaneous lesions |
Single slowly growing subcutaneous nodule |
Histology |
Lobular panniculitis without vasculitis |
Lobular panniculitis without vasculitis |
Management |
Therapy may include itraconazole or amphotericin B (for months) |
Surgical excision |
The medical literature about viral panniculitis is limited to a few case reports. Cytomegalovirus (CMV) has been reported to cause panniculitis in an immunocompromised patient.