Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Sheida Naderi-Azad, medical student, University of Toronto Faculty of Medicine, Toronto, ON, Canada. DermNet Editor in Chief: Adjunct Assoc. Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. December 2019.
Introduction - innate immune response Introduction - inflammasome Introduction - inflammatory skin disease Inflammasomes in allergic contact dermatitis Inflammasomes in psoriasis Introduction - autoinflammatory disease Inflammasomes in autoinflammatory skin disease
The innate immune response refers to the parts of the immune system that are immediately functional. It includes:
An inflammasome is a part of the innate immune system. It is an intracellular complex that binds microbes and creates a signal cascade to attack them.
Inflammasomes include [2]:
An inflammasome consists of [3]:
Inflammasomes regulate the immunological response to exogenous stimuli (eg, bacteria) and endogenous stimuli (eg, neoplasia) via cytokine secretion, particularly interleukin (IL)-1β and IL-18, and induce neutrophil recruitment [4].
Inflammasomes also play an important role in acute and chronic inflammatory diseases [4].
Inflammatory skin diseases are characterised by the activation of the innate and adaptive immune system via the production of pro-inflammatory cytokines [4]. They are classified as autoimmune diseases and autoinflammatory syndromes or diseases.
Autoimmune inflammatory skin diseases such as vitiligo and lupus erythematosus involve aberrant responses to autoantigens, controlled by B cells and T cells, with the presence of autoantibodies.
Autoinflammatory skin diseases such as periodic fever syndromes and neutrophilic dermatoses involve activation of innate immune system cells (macrophages, neutrophils, mast cells and natural killer [NK] cells), resulting in tissue damage in the absence of autoantigens and autoantibodies.
Some skin diseases such as psoriasis have autoimmune and autoinflammatory components [4].
We use the examples of allergic contact dermatitis and psoriasis to illustrate the role that inflammasomes have in chronic inflammatory skin diseases.
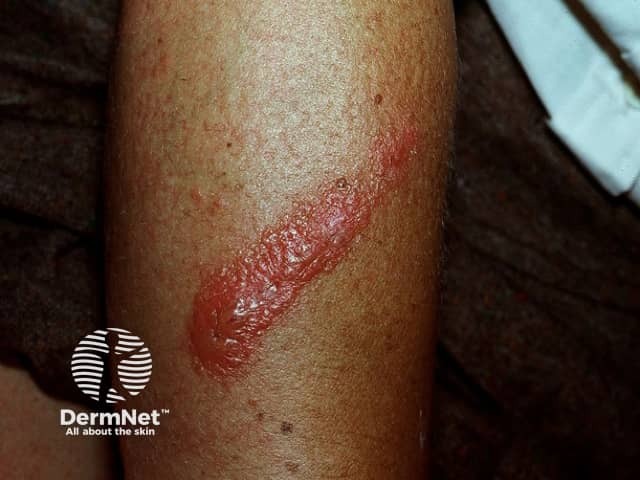
Contact allergic dermatitis
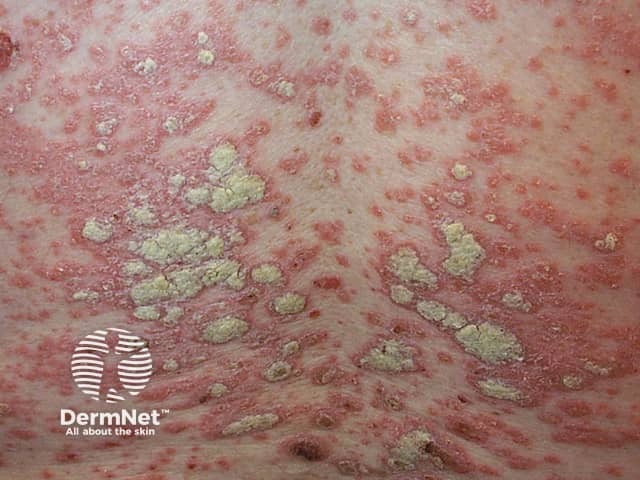
Chronic plaque psoriasis
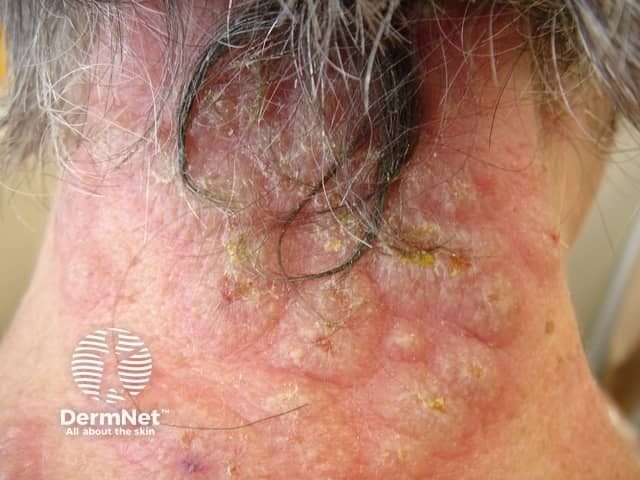
Acute neutrophilic dermatosis
Allergic contact dermatitis is an erythematous, pruritic rash caused by a delayed hypersensitivity reaction to a small molecule [5].
In experimental contact dermatitis due to 2,4-dinitrofluorobenzene (DNFB), priming of the adaptive immune system has been shown to depend on the activation of the innate immune system [5].
The evidence behind inflammasome-mediated production of IL-1 family cytokines in contact dermatitis is as follows:
Psoriasis is a common skin condition characterised by circumscribed erythematous plaques covered with a silvery scale.
The pathophysiology of psoriasis is complex; it involves neutrophils and the innate immune response [7].
Antagonists of members of the IL-1 family are under investigation for the treatment of psoriasis [2].
Autoinflammatory syndromes and diseases are characterised by multiple inflammatory episodes caused by an exaggerated innate immune response. The pathogenesis does not involve specific autoantibodies and T-cells.
An autoinflammatory disease is diagnosed after excluding infective, neoplastic and allergic conditions.
Autoinflammatory syndromes include hereditary periodic fever syndromes, other monogenic autoinflammatory syndromes, noninherited or polygenic disorders (such as generalised pustular psoriasis) and neutrophilic dermatoses.
Inflammasomes upregulate the signalling of various cytokines (including IL-1) in autoinflammatory skin diseases, which in turn amplify neutrophil-mediated inflammation through multiple mechanisms. IL-1β has antiapoptotic effects on neutrophils, prolonging their survival.