Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Sarajane Ting, General Practitioner, Tasmania, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. February 2020.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
Lymphocytic thrombophilic arteritis is a primary lymphocytic vasculitis. It presents with livedo racemosa or macular hyperpigmentation. It has distinct histological findings affecting small to medium-sized arteries in the deep dermis and superficial subcutis [1].
It is also known as macular lymphocytic arteritis.
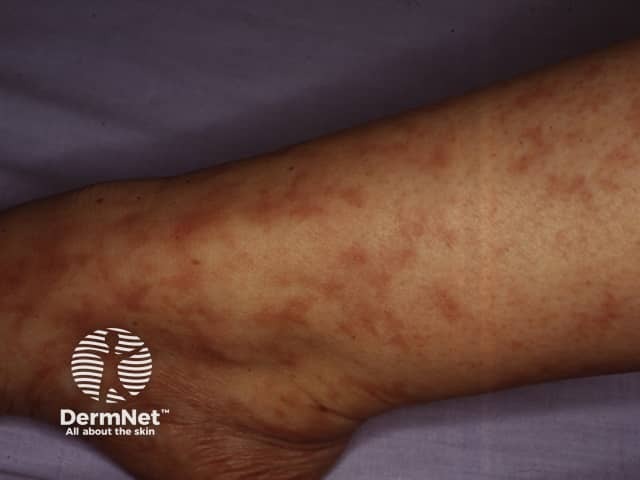
Lymphocytic thrombophilic arteritis shows a female predominance, with a median age of 39 years (range 6-73) [2].
The exact cause of lymphocytic thrombophilic arteritis is unknown. It has been proposed that the underlying lymphocytic endovasculitis drives a localised thrombophilia, represented by the intraluminal fibrin ring seen on histology, without any evidence of destruction of the vessel wall [1].
The clinical features of lymphocytic thrombophilic arteritis include:
The diagnosis of lymphocytic thrombophilic arteritis is based on a combination of typical clinical features supported by distinct histological findings [1].
Signs or symptoms of systemic vasculitis are also absent (see Cutaneous vasculitis) [2].
Lymphocytic thrombophilic arteritis can be confused with several other vascular occlusive conditions showing livedo reticularis.
Lymphocytic thrombophilic arteritis tends to show an indolent course with persistent asymptomatic livedo racemosa or macular hyperpigmentation [1]. As most lesions are asymptomatic, treatment is not always required [2].
Treatment options that have shown a beneficial response include:
Oral and topical steroids have not been shown to be helpful [2].
Given the rarity of lymphocytic thrombophilic arteritis and inconsistent treatment responses, there is no current consensus on treatment recommendations.
Lymphocytic thrombophilic arteritis tends to follow a chronic indolent course with no progression to systemic vasculitis [1,2]. Ongoing follow-up is advisable as there have been rare reports of later systemic vasculitis [11]. The long-term prognosis remains unclear.