Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Avee Naidoo, Resident Physician, University of Toronto Faculty of Medicine, Toronto, Canada. DermNet New Zealand Editor in Chief: A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. July 2020.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Sneddon syndrome is a rare, slowly progressive, neurocutaneous vasculopathy. It is characterised by the combination of livedo racemosa and recurrent cerebrovascular events, such as transient ischaemic attacks and strokes.
Sneddon syndrome is also called Ehrmann-Sneddon syndrome, livedo racemose and cerebrovascular accident syndrome, and livedo reticularis and cerebrovascular accident syndrome.
The incidence of Sneddon syndrome is approximately four per million per year in the general population. Sneddon syndrome is typically first diagnosed in women aged 20–42 years. There does not appear to be any racial variation, although reported numbers are small.
Sneddon syndrome is often associated with autoimmune diseases, such as antiphospholipid syndrome and systemic lupus erythematosus.
As antiphospholipid antibody markers are present in 50–80% of patients with Sneddon syndrome, it is included in the clinical spectrum of primary antiphospholipid syndrome.
Vascular thrombosis and recanalisation of small and medium-sized blood vessels in the skin and brain are due to coagulopathy or thrombophilia, which is associated with decreased levels of activated protein C and protein S and elevated levels of factor VII.
Sneddon syndrome can be inherited as an autosomal dominant disease with variable penetrance in rare familial cases. Loss-of-function mutations have been identified in the cat eye syndrome region 1 candidate 1 (CECR1) on chromosome 22, encoding adenosine deaminase 2 (ADA2).
Sneddon syndrome has dermatological and neurological manifestations.
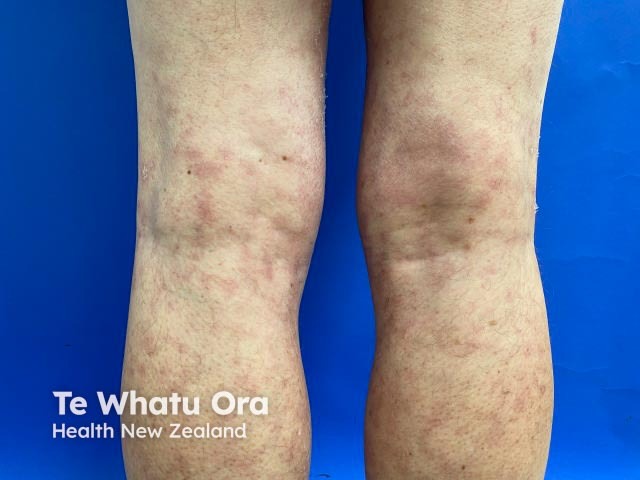
Livedo racemosa
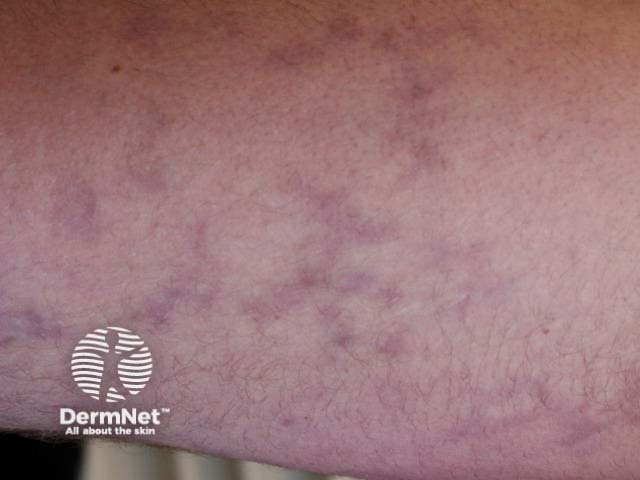
Livedo racemosa
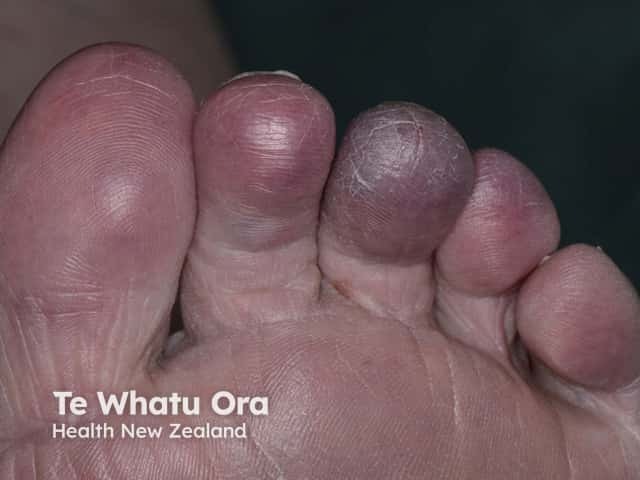
Acrocyanosis
Sneddon syndrome is characterised by livedo racemosa, which precedes the onset of recurrent strokes by over 10 years [1,2]. The significance of the livedo racemosa, which often begins in childhood, is only recognised in the 20s and 30s after the cerebrovascular events begin.
Other dermatological manifestations associated with Sneddon syndrome include:
Neurological manifestations associated with Sneddon syndrome generally present in three stages.
Cerebrovascular complications of Sneddon syndrome include:
Cardiovascular complications of Sneddon syndrome include:
Ophthalmological complications of Sneddon syndrome include:
Renal complications are rare:
Criteria for diagnosis of Sneddon syndrome include the presentation of livedo racemosa with characteristic histopathological findings on skin biopsy and focal neurological deficits. History of transient ischaemic attacks or stroke or evidence of these on imaging can support the diagnosis.
Patients with a suspected diagnosis of Sneddon syndrome should have blood tests screening for autoimmune disease and coagulopathies, cerebral MRI, cardiovascular assessment, and skin biopsy.
Lesions identified by MRI tend to be small, multifocal, and often located in the periventricular deep white matter or pons. In up to 75% of patients with Sneddon syndrome, cerebral angiography is abnormal.
On deep skin biopsy, histopathology demonstrates a non-inflammatory thrombotic vasculopathy involving subcutaneous small and medium-sized dermal arteries. Sensitivity increases with the number of deep skin biopsies: 27% sensitivity with one, 53% with two, and 80% with three biopsies.
Extensive investigation is necessary for patients presenting with livedo racemosa or stroke to rule out other diseases in the differential.
Sneddon syndrome is classified as antiphospholipid negative or positive, based on the presence of any of 3 antiphospholipid antibodies: anticardiolipin, lupus anticoagulant, and anti-beta 2-glycoprotein I [2].
It can also be classified as primary (idiopathic) or secondary to an identified thrombophilia or autoimmune disease, such as lupus erythematosus [1]. Sneddon syndrome is also occasionally classified as a vasculitis.
The differential diagnosis for Sneddon syndrome may include:
Congenital livedo reticularis
Another haematological condition
Cardiac disease resulting in multiple emboli
Neoplasia
Infection
Effects of a drug
Divry van Bogaert Syndrome.
Treatment is based on anecdotal reports and includes:
Lifestyle modifications recommended for Sneddon syndrome include:
Sneddon syndrome is a chronic, progressive disease often resulting in cognitive decline and early-onset dementia due to the cumulative effect of multiple cerebral infarcts.