Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Necrolytic acral erythema is a clinically distinct entity affecting the skin of the toes and tops of feet, seen predominantly in patients with hepatitis C.
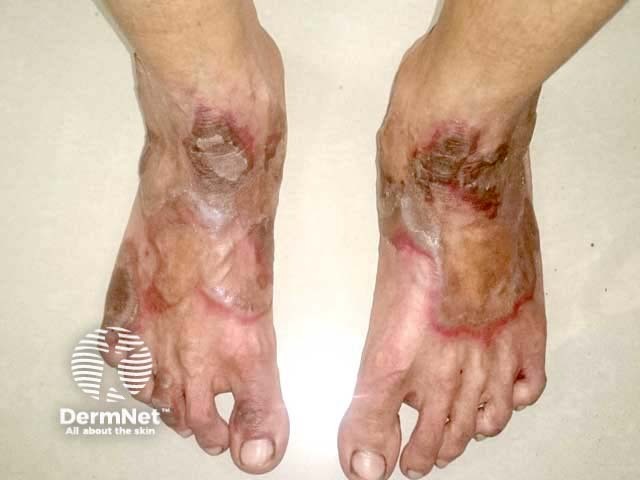
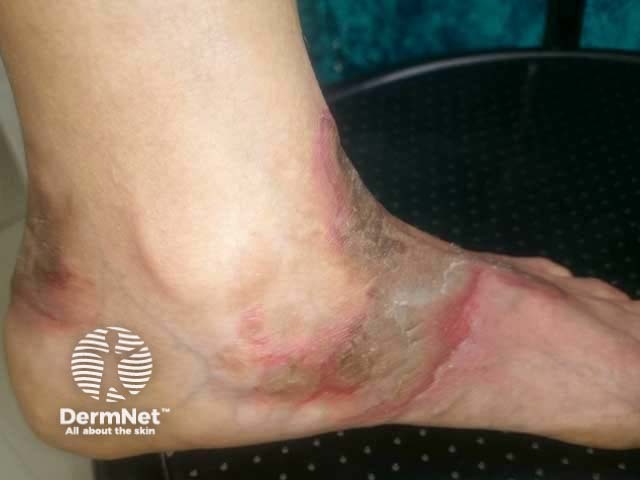
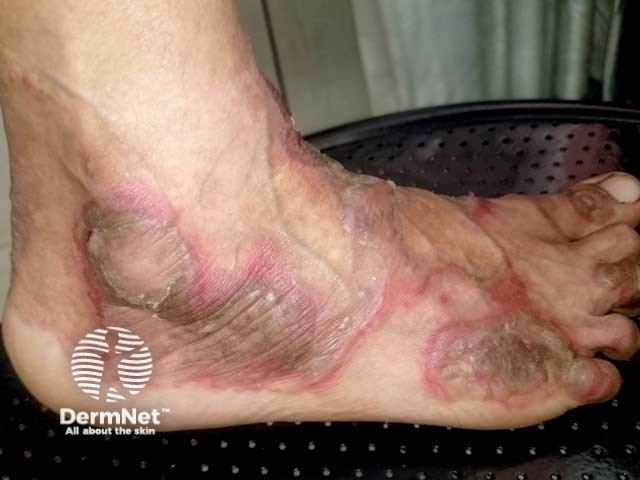
Necrolytic acral erythema was first described in hepatitis C-positive patients. A study in the US suggested it develops in 1–2% of patients with chronic hepatitis C, and most studies report this to be the commonest association for this skin sign [see Viral hepatitis].
A small number of affected patients are seronegative for hepatitis C. The next most common association reported has been zinc deficiency occurring with various other disorders including coeliac disease and Crohn disease.
All reported cases have been in skin of colour including Asians and Africans, with an equal sex incidence, and a mean onset of 40–45 years of age (range 11–78 years).
The aetiopathogenesis of necrolytic acral erythema appears to be multifactorial and may involve genetic factors, nutritional deficiency (specifically zinc), and liver dysfunction resulting in low blood levels of albumin, glucagon, and amino acids.
Although Japan has a very high rate of chronic hepatitis C infection, no cases have been reported from Japan. This may reflect the predominant hepatitis C genotypes in that population or predisposing genetic factors.
Zinc is an essential cofactor for replication of the hepatitis C viral genome.
Viral load and immunosuppression do not appear to be risk factors.
Necrolytic acral erythema can be the first sign of hepatitis C infection or zinc deficiency, presenting as a symmetrical acral rash.
Necrolytic acral erythema typically affects the tops of the toes and feet. Sometimes the skin lesions occur on the ankles, knees, and legs, and rarely the hands, elbows, genitalia, and buttocks. Palms, soles, and nails are almost always spared.
The skin lesions are usually painful or sometimes itchy or with a burning sensation.
The acute skin lesions are red with a margin of erosions or flaccid blisters.
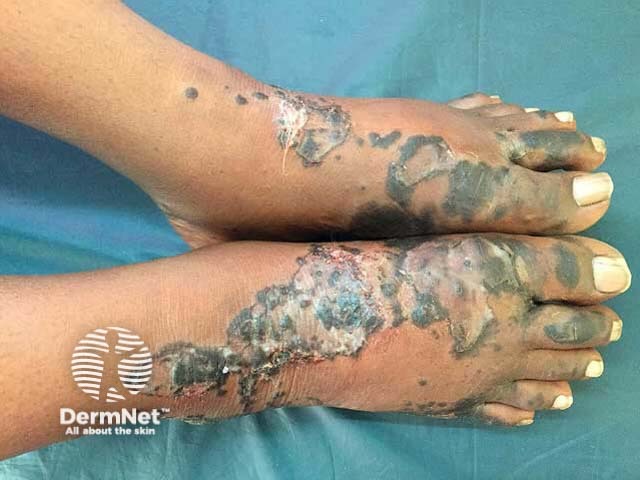
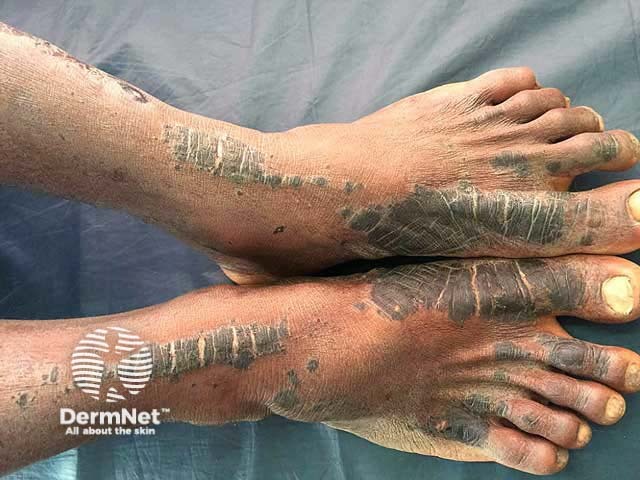
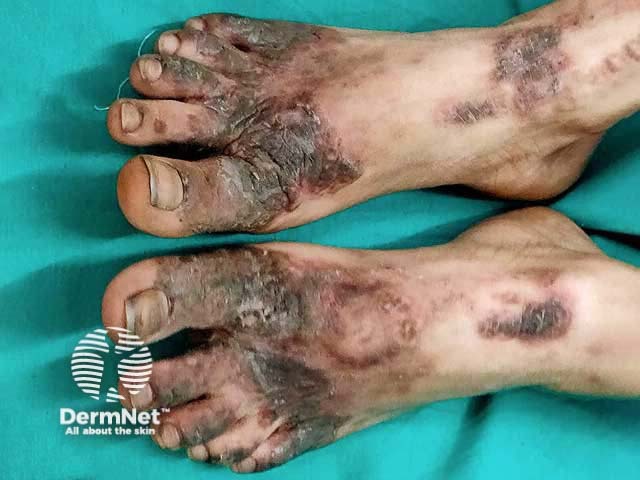
Necrolytic acral erythema should be suspected on the skin signs in an appropriate clinical setting.
Skin biopsy shows the same histological features as necrolytic migratory erythema: hyperkeratosis with parakeratosis, epidermal spongiosis and focal necrosis, mixed superficial dermal inflammatory infiltrate.
Blood tests should include:
Topical treatments, such as topical steroids or calcineurin inhibitors (eg, pimecrolimus, tacrolimus), do not seem to be helpful.
Necrolytic acral erythema follows a relapsing course of spontaneous remissions and recurrences. Skin changes rapidly settle with appropriate treatment, but can recur if treatment is stopped.