Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Leah Jones, Medical Registrar, Christchurch, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. May 2020.
Introduction - Acrodermatitis enteropathica Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Acrodermatitis enteropathica is a rare genetic disorder of zinc metabolism characterised by the triad of dermatitis, diarrhoea, and alopecia [1]. It is an autosomal recessive condition caused by a mutation in the SLC39A4 gene, which codes for a zinc transporter protein [1,2].
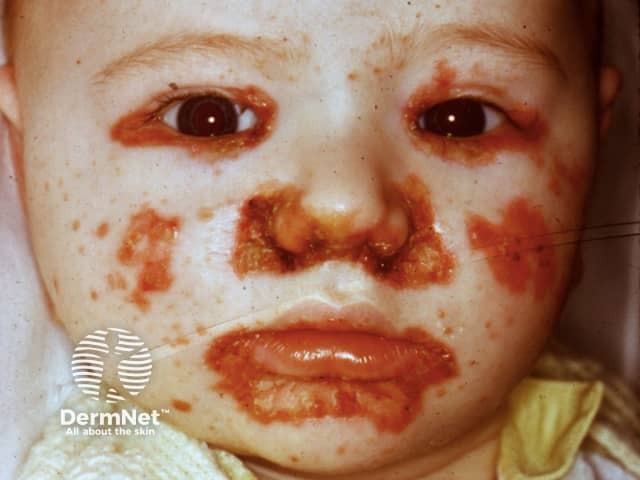
Acrodermatitis enteropathica
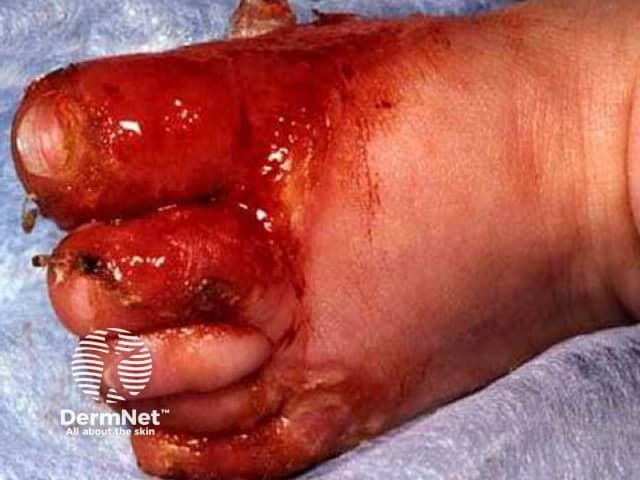
Acrodermatitis enteropathica
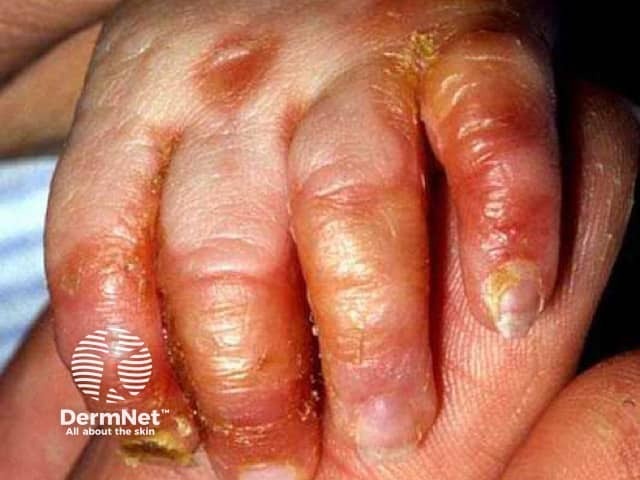
Acrodermatitis enteropathica
An acrodermatitis enteropathica-like condition presents with similar features to acrodermatitis enteropathica, but is caused by acquired zinc deficiency or a disorder of amino acid or fatty acid metabolism [1].
Acrodermatitis enteropathica-like conditions include:
An acrodermatitis enteropathica-like condition can be categorised as secondary to acquired zinc deficiency or to a metabolic disorder unrelated to zinc deficiency [1].
Causes of acquired zinc deficiency include [1-4]:
An acrodermatitis enteropathica-like condition related to a metabolic disorder can be secondary to:
Acrodermatitis enteropathica-like conditions secondary to metabolic disorders are caused by abnormalities disrupting the metabolism of amino acids or fatty acids [1]. This can be direct, through disruption of the urea cycle, or by affecting co-factors, notably biotin [1–3].
Metabolic disorders responsible for acrodermatitis enteropathica-like conditions include [1–3]:
Necrolytic migratory erythema can present with a rash similar to acrodermatitis enteropathica in adults and is associated with glucagonoma [1].
When an acrodermatitis enteropathica-like condition is related to acquired zinc deficiency, the lack of zinc leads to abnormal keratinisation, cell proliferation, and defective immune response [1].
In metabolic disorders, amino acid or fatty acid deficiency leads to reduced keratinocyte growth and differentiation [1].
Like its namesake, an acrodermatitis enteropathica-like condition typically presents with the triad of dermatitis, diarrhoea, and alopecia [2].
The cutaneous features of an acrodermatitis enteropathica-like condition include [1–3]:
Other features of an acrodermatitis enteropathica-like condition depend on the underlying cause, but often include [1,3,5]:
An acrodermatitis enteropathica-like condition can be complicated by secondary bacterial infection or candidiasis [1].
Decompensation of a congenital metabolic disorder during periods of illness or stress may result in acidosis, which is potentially fatal [5]. Long-term neurodevelopmental problems are not uncommon in congenital metabolic disorders [1,5,6].
Acquired zinc deficiency is associated with low serum zinc levels and alkaline phosphatase [2]. Zinc levels and alkaline phosphatase tend to be normal in acrodermatitis enteropathica-like conditions related to metabolic disorders [1].
A full blood count may reveal cytopenias in both acquired zinc deficiency and metabolic disorders [2,5].
The initial blood tests for an organic acidaemia may include [5]:
Levels of specific amino acids or enzyme activity and the presence of organic acids in the urine may support a specific diagnosis [1,5].
Newborn screening detects many of the congenital metabolic causes of acrodermatitis enteropathica-like conditions and is available in many parts of the world including New Zealand, Australia, the United Kingdom, the United States, and Canada [5].
A skin biopsy of an acrodermatitis enteropathica-like condition has non-specific histopathology; epidermal pallor and confluent parakeratosis may be observed [7].
The differential diagnosis of an acrodermatitis enteropathica-like condition includes:
An acrodermatitis enteropathica-like condition secondary to acquired zinc deficiency will resolve after oral zinc supplementation, usually at an initial dose of 0.5–1 mg/kg/day of elemental zinc [2]. Whether there is an ongoing need for zinc replacement will depend on the cause [2,8].
An acrodermatitis enteropathica-like condition secondary to a metabolic disorder generally responds to dietary manipulation and medication in the form of specific organic supplements to correct metabolic deficiencies [5]. Expert assistance should be sought from a nutritionist.
The outcome for an acrodermatitis enteropathica-like condition depends on the underlying condition.
An acrodermatitis enteropathica-like condition secondary to acquired zinc deficiency has a favourable prognosis if identified early [8,9]. The dermatological, gastrointestinal, and psychological manifestations tend to resolve within days to weeks following zinc replacement [9].
An acrodermatitis enteropathica-like condition secondary to a metabolic disorder can have a high mortality rate in the newborn period if undiagnosed. This is mitigated to some extent by detection in the newborn period with the help of screening programmes [5]. A significant number of children diagnosed early with congenital metabolic disorders will still have ongoing problems with metabolic crises and neurocognitive development [5,6].