Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Latest update by Dr Arun Gangakhedkar, Paediatrician, Waitakere Hospital, Auckland, New Zealand. DermNet Editor in Chief: Adjunct Assoc. Prof. Amanda Oakley. December 2019.
Introduction Zinc in the body Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
Acrodermatitis enteropathica is a rare disorder associated with zinc deficiency. It presents with the classic triad of:
Primary acrodermatitis enteropathica is due to an inherited zinc transporter defect, resulting in reduced intestinal absorption of zinc.
Acquired acrodermatitis enteropathica may be a result of reduced intake, increased demand, malabsorption, or may rarely be associated with certain metabolic disorders. [See Acrodermatitis enteropathica-like conditions]
Pseudo-acrodermatitis enteropathica has been described in biotinidase deficiency, organic acid, amino acid, urea cycle and essential fatty acid disorders.
Acrodermatitis enteropathica is also called acrodermatitis enteropathy, primary zinc malabsorption syndrome, Danbolt-Closs syndrome, and Brandt syndrome.
Zinc is an essential micronutrient with better bioavailability from human milk than cow’s milk or other infant formulae.
Zinc is a part of over 200 metalloenzymes involved in cellular metabolism.
Primary acrodermatitis enteropathica is an autosomal recessive genetic disorder and manifests when two defective genes are inherited (one from each parent). Carriers have one normal gene and one defective gene and will not usually have any symptoms of the disease.
The SLC39A4 gene located on chromosome 8q24.3 codes for the zinc transporter protein, ZIP4. A mutation in SLC39A4 disturbs the uptake, transport and overall homeostasis of zinc. Zinc deficiency in primary acrodermatitis enteropathica is secondary to a partial block in zinc absorption across the small intestinal mucosa.
A large number of enzymes require zinc as a cofactor leading to heterogenic clinical manifestations.
Acquired acrodermatitis enteropathica may be associated with the following:
Primary acrodermatitis enteropathica may manifest in formula-fed infants within a few days to weeks after birth, and soon after weaning in breast-fed infants. Both males and females are equally affected.
Symptoms of acquired acrodermatitis enteropathica may occur at any age, depending on the underlying cause, but mostly affect older children, adolescents and adults.
Preterm infants may present early with acrodermatitis enteropathica due to increased demand and negative zinc balance at birth. Acrodermatitis enteropathica in preterm infants can be due to zinc-deficient breast milk or a mutation of the transporter protein.
Primary and acquired acrodermatitis enteropathica have similar cutaneous and non-cutaneous findings.
A form of dermatitis is typically the first manifestation of zinc deficiency. Characteristically, it is found in an acral and peri-orificial distribution.
Diffuse hair loss affects the scalp, eyebrows and, eyelashes. The nails are soft with ridging, dystrophy and paronychia.
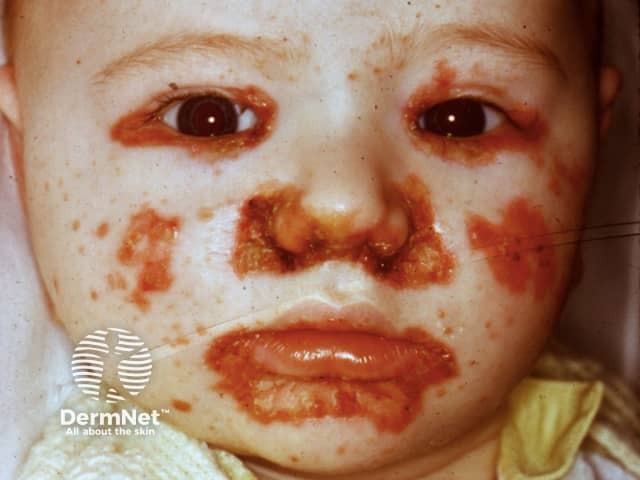
Acrodermatitis enteropathica
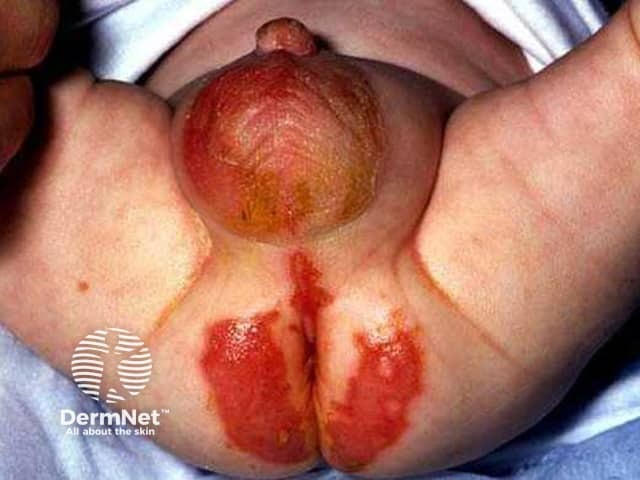
Acrodermatitis enteropathica
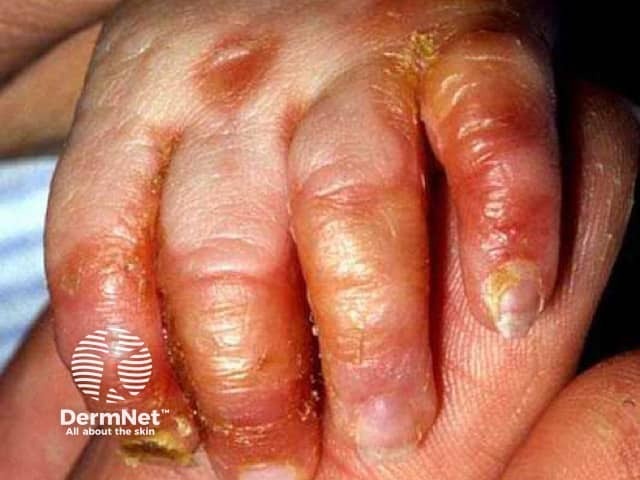
Acrodermatitis enteropathica
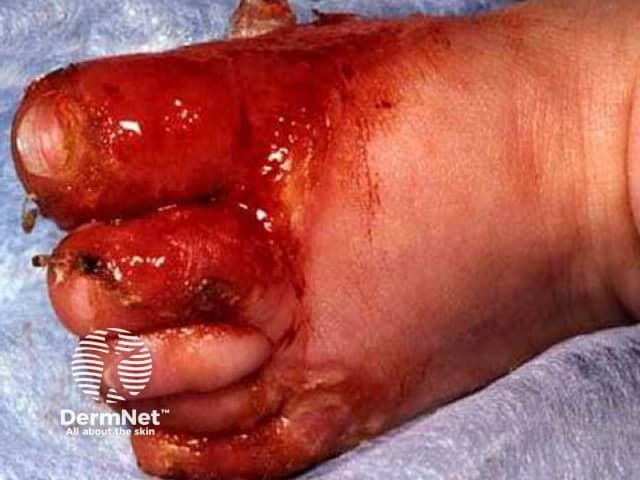
Acrodermatitis enteropathica
Other features of acrodermatitis enteropathica include:
The following investigations may be helpful if zinc deficiency and acrodermatitis enteropathica are suspected.
A biopsy from an early skin lesion is not specific as the histology may be similar to eczema or psoriasis. Spongiosis with epidermal pallor may be seen initially. Confluent parakeratosis, keratinocyte necrolysis, a thin Malpighian layer and an absence of granular layer may be seen later.
Other conditions that should be considered may include:
Treatment of primary acrodermatitis enteropathica begins with high-dose supplementation using oral elemental zinc at 3 mg/kg/day (there is 50 mg of elemental zinc in 220 mg of zinc sulfate). High dose oral supplementation overcomes the transporter defect.
Treatment of acquired or dietary zinc deficiency begins with 0.5-1 mg/kg/day of elemental zinc while the malnutrition is being treated. Zinc can be given during pregnancy.
Secondary bacterial skin infection and candida require appropriate therapy.
Typically, diarrhoea, irritability, and mood symptoms improve within a day of commencing zinc treatment. Skin healing is noted within a week and normal hair growth is seen within a month of zinc replacement.
The prognosis of acrodermatitis enteropathica is generally good with prompt diagnosis and zinc replacement but can be potentially fatal without treatment.
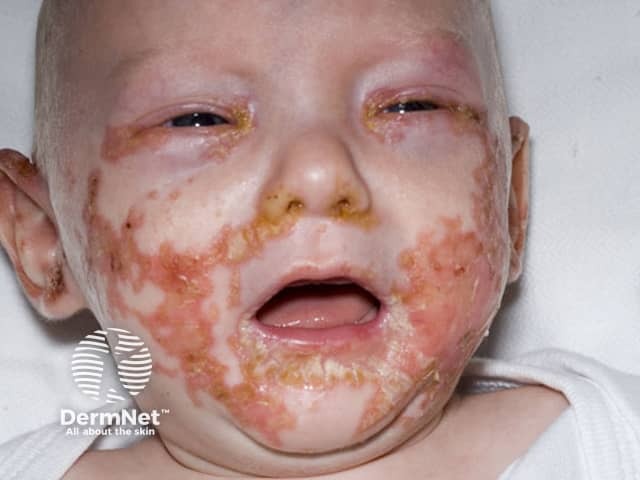
Acrodermatitis enteropathica
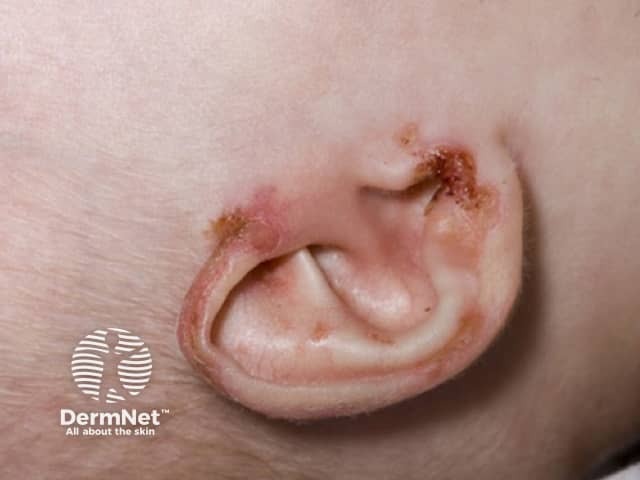
Acrodermatitis enteropathica
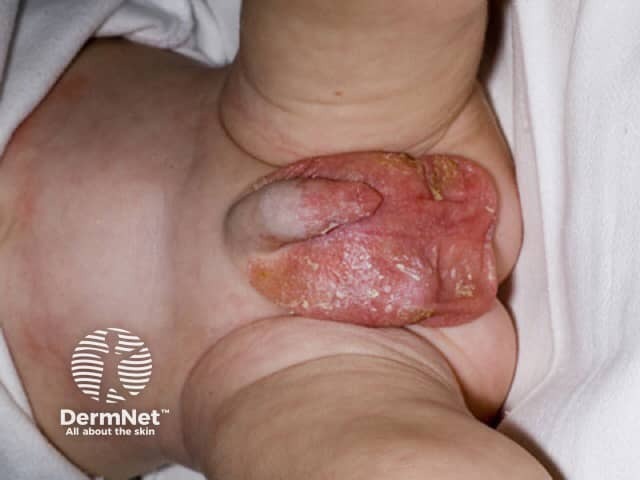
Acrodermatitis enteropathica
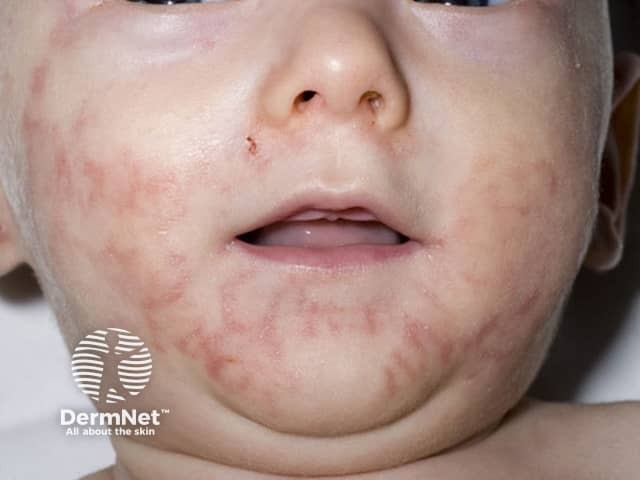
Acrodermatitis enteropathica
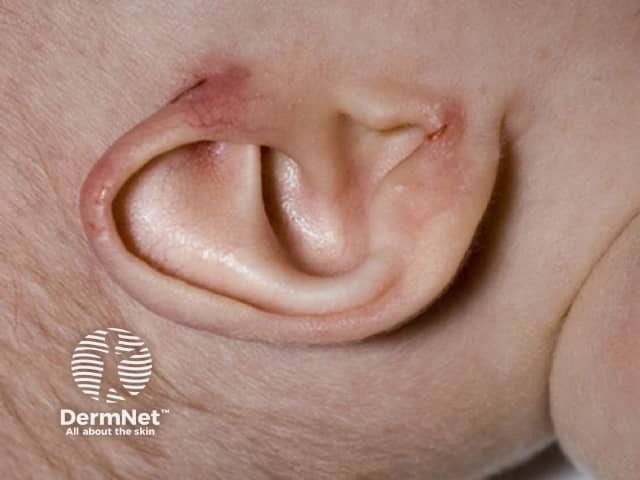
Acrodermatitis enteropathica
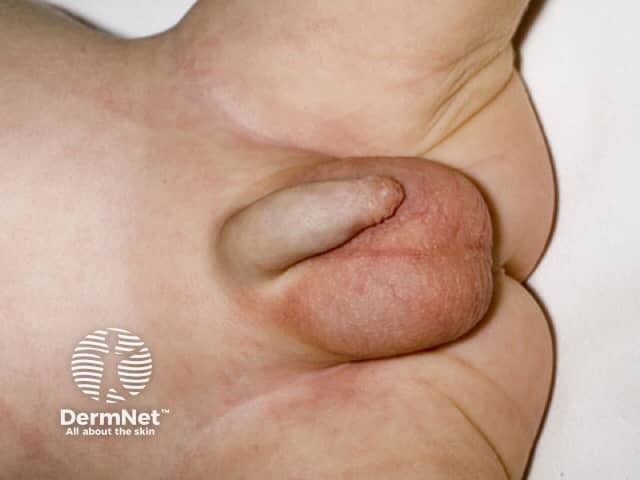
Acrodermatitis enteropathica