Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Emily Ryder, Dermatology Registrar, Waikato Hospital, Hamilton, New Zealand; Chief Editor: A/Prof Amanda Oakley, August 2014.
Introduction Clinical features Demographics Causes Diagnosis Treatment
Perineal pyramidal protrusion is a lump or protrusion of perineal tissue near the anus of some young children, usually girls.
Perineal pyramidal protrusion may also be called perianal pyramidal protrusion, perianal protrusion in childhood, infantile perineal protrusion or infantile perianal pyramidal protrusion.
Perineal pyramidal protrusion may be present at birth or may occur during early childhood. It may be noticed when a child is assessed for a symptom such as constipation or vulval itch.
It is characterised by a smooth flesh-coloured or pink-red nodule near the anus. It is located in the midline and anterior to the anus in an area called the perineal median raphe.
Perineal pyramidal protrusion is typically smooth and pink and measures from 5.5 mm2 to 28.5 mm2 in size. The tissue has been described as triangular, pyramidal, oval, tongue-shaped or leaf-shaped.
A careful history and examination are required to differentiate perineal pyramidal protrusion from the following conditions:
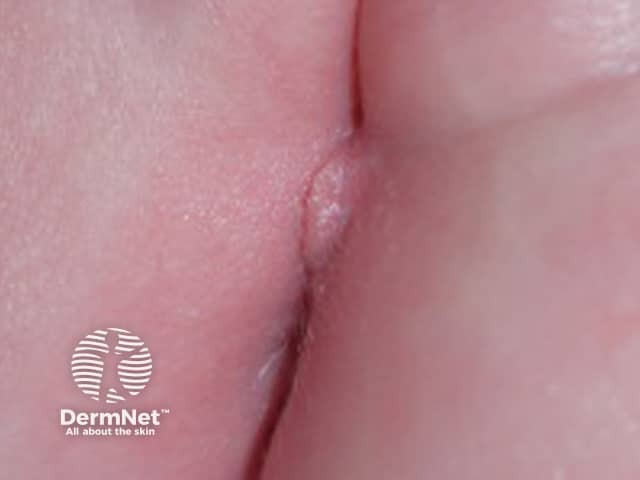
Perineal pyramidal protrusion

Perineal pyramidal protrusion
Perineal pyramidal protrusion occurs in children from birth to the age of 13 years. The average age at diagnosis is 14 months. More than 90% of patients with perineal pyramidal protrusion are female.
Perineal pyramidal protrusion is often associated with constipation although it is not clear whether constipation is a cause or a consequence of the protrusion. It has also been reported in infants with lichen sclerosus.
The cause of perineal pyramidal protrusion is not clear.
The diagnosis of perineal pyramidal protrusion is made by recognition of the clinical features.
Surgery or skin biopsy is not usually required but may be undertaken to exclude lichen sclerosus. Histopathologic examination of perineal pyramidal protrusion may show normal skin or acanthosis (thickening of the epidermis), dilated capillaries, fibrous tissue and eosinophils (inflammatory cells).
Perineal pyramidal protrusion tends to resolve on its own. If the infant is reported to have constipation, dietary changes, ensuring adequate fluid intake and laxatives may be helpful.