Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Lauren Smith, medical student, Christchurch, New Zealand. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor(s): Gus Mitchell/Maria McGivern. July 2017.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Phrynoderma is a form of follicular hyperkeratosis associated with nutritional deficiency.
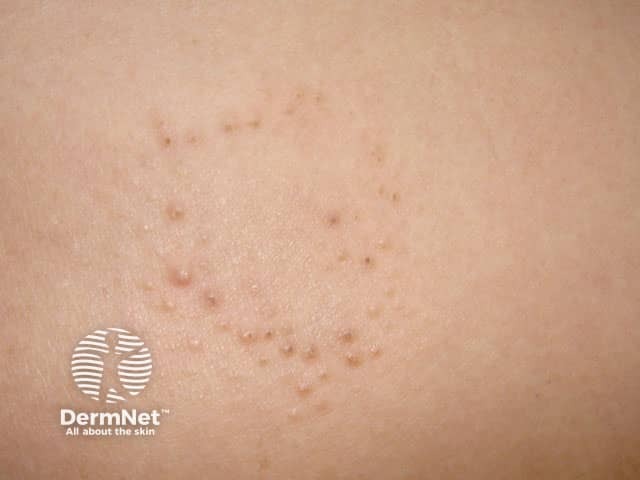
Lichen spinulosa
Phrynoderma is most often reported in children living in poverty in Africa and Asia.
A dietary history may reveal:
Phrynoderma is rare in developed countries, when it is most often associated with:
Phrynoderma is associated with other chronic illnesses, such as pancreatic insufficiency, inflammatory bowel disease, and gallbladder disease [1–3].
Phrynoderma is associated with nutritional deficiency, particularly [1,4]:
Phrynoderma is a form of asymptomatic or mildly symptomatic follicular hyperkeratosis, where follicular papules of various sizes with central keratotic plugs that block the follicle openings develop on the skin [1]. New patches may be hypopigmented [3,4].
Patches initially arise on the back of the elbows and the front of the knees, and can spread to involve the extremities, upper forearms and thighs.
Occasionally patches will also appear on the abdomen, back and buttocks. The face is rarely affected, and hands and feet are spared [1].
Other symptoms of vitamin A deficiency can be present, such as:
Features of severe vitamin A deficiency can include [2]:
Phrynoderma may result in persistent hyperpigmentation or scarring.
In the right context, phrynoderma may be suspected by its characteristic clinical features. If a skin biopsy is performed, histological features may include:
The level of vitamin A in the blood of patients with phrynoderma may be either low (< 30 μg/100 mL) or normal. These vitamin A levels may not reflect a clinically apparent deficiency, as stores may last up to a year in adults [1]. Severe malnutrition is also associated with reduced albumin levels.
The diagnosis of phrynoderma is supported if the signs resolve with better nutrition [4].
Several other conditions are characterised by follicular hyperkeratosis. These conditions include:
Patients with phrynoderma can be assessed by a nutritionist, dietician, ophthalmologist, dermatologist, gastroenterologist and/or a general physician.
Nutritional management may include:
Topical keratolytic agents can be applied to the scaly plaques for symptomatic relief. These agents can include:
Skin lesions can take 1–4 months to resolve with restoration of nutrition. Topical keratolytic medicines can provide temporary relief [3,4].
Vitamin A deficiency can cause ocular disturbance, but this generally resolves within days of starting therapy, unless scarring has occurred. If left untreated, there can be permanent scarring of the conjunctiva and cornea [3,4].