Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Fiona Larsen, Dermatology Registrar, Green Lane Hospital, Auckland, New Zealand, 2005. Updated by Dr Janice Yeon, Dermatology Research Fellow, The Skin Hospital, Sydney NSW, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. October 2020.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Eosinophilic cellulitis is an uncommon recurrent inflammatory skin disease, also known as Wells syndrome.
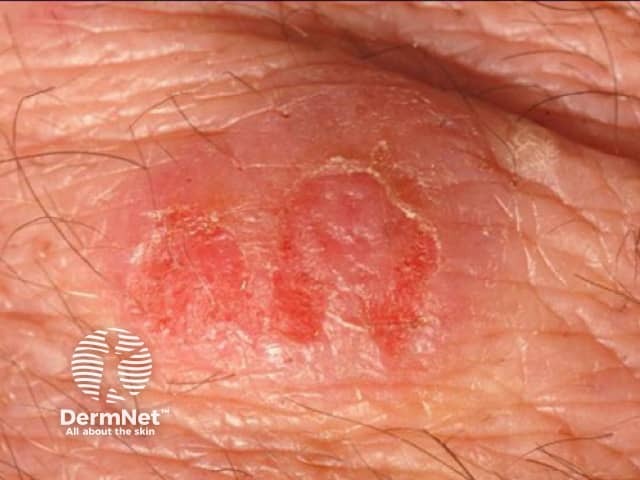
Eosinophilic cellulitis
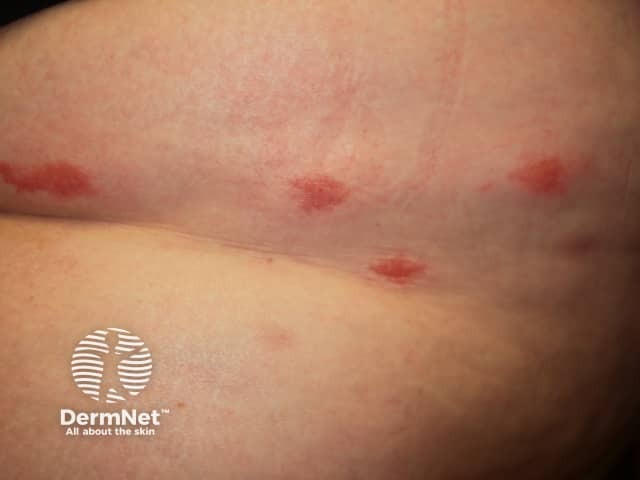
Eosinophilic cellulitis
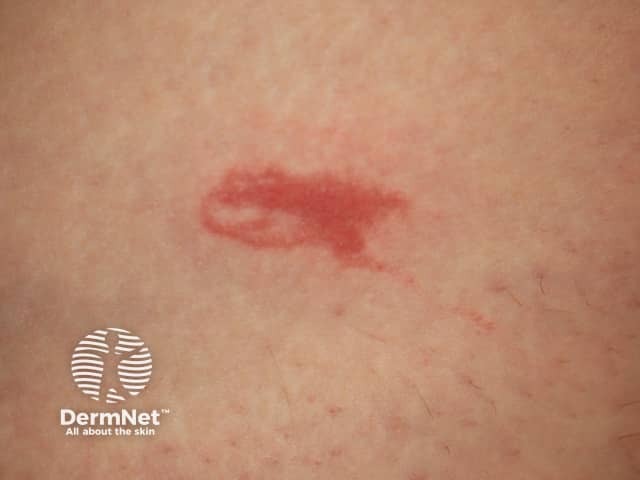
Eosinophilic cellulitis
Eosinophilic cellulitis can affect all age groups including children and infants.
The cause of eosinophilic cellulitis is unknown. It is believed to be a local hypersensitivity reaction.
Most cases appear to be idiopathic. Implicated triggers or associations include:
Eosinophilic cellulitis usually presents as itchy or burning erythematous nodules or plaques resembling cellulitis or erysipelas on a limb. However, the clinical appearance is variable: lesions can be single or multiple, the face and trunk may be affected, and clinical morphology can include:
The classic plaque-type variant of eosinophilic cellulitis is the most common presentation in children, whereas the annular granuloma-like variant is more frequently seen in adults.
Individual lesions can resolve spontaneously but typically recur.
Associated systemic symptoms may include fever and arthralgias.
Eosinophilic cellulitis may be rarely complicated by superinfection.
Severe swelling of a limb can cause compartment syndrome.
Eosinophilic cellulitis is often misdiagnosed initially as cellulitis or erysipelas, and is only considered when antibiotic treatment is unhelpful.
Proposed diagnostic criteria for eosinophilic cellulitis require at least two major and one minor criteria.
Major criteria for an eosinophilic cellulitis diagnosis include:
Minor criteria for an eosinophilic cellulitis diagnosis include:
Peripheral eosinophilia affects approximately 50% of cases but is not required for diagnosis.
Skin biopsy is usually required and the histological findings depend on the stage of disease.
Flame figures are not pathognomonic of Wells syndrome and can be seen with other eosinophilic infiltrates, such as:
The differential diagnosis for eosinophilic cellulitis may include:
Eosinophilic cellulitis rapidly responds to an oral corticosteroid, such as prednis(ol)one, but often relapses when the steroid dose is reduced.
Other treatments used may include:
Treatment of an associated trigger, such as cessation of an implicated drug, can lead to complete resolution.
Eosinophilic cellulitis has a benign course with a tendency for lesions to spontaneously resolve. However, recurrence is common.