Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Mark Duffill, Dermatologist, Hamilton, New Zealand, 2008. Updated by A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, January 2016.
Introduction
Introduction - eosinophils
Causes
Clinical features
Diagnosis
Treatment
Outcome
Eosinophilic granulomatosis with polyangiitis is a rare disease that affects the lungs, the skin and sometimes other organs. The name comes from the presence of eosinophils, granulomas and inflamed blood vessels. It is also known as Churg-Strauss syndrome, Churg-Strauss granulomatosis and allergic granulomatosis.
The main features of eosinophilic granulomatosis with polyangiitis are:
Eosinophils are a type of white blood cell. They are often increased in number in allergic disorders.
The cause of eosinophilic granulomatosis with polyangiitis is uncertain, but it is currently thought to be an autoimmune process.
It has been associated with drug sensitivities to penicillin, penicillamine, iodides, leukotriene modifiers and mesalazine in some patients.
Eosinophilic granulomatosis with polyangiitis has been divided into three distinct phases, which may or may not be sequential. Symptoms depend upon the phase and organs involved.
Prodromal phase |
|
Second phase |
|
Vasculitic phase |
|
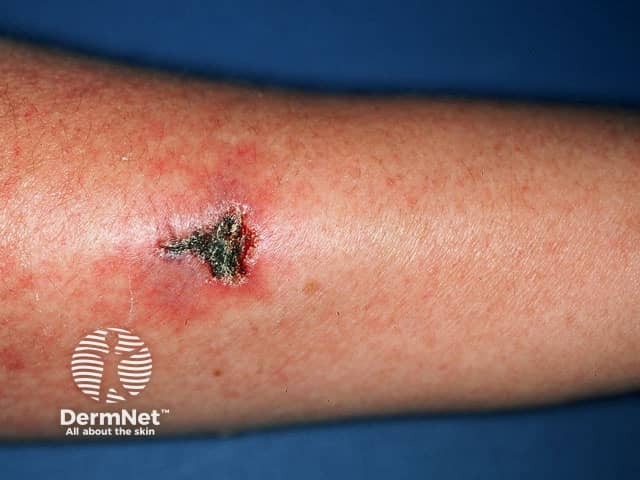
Eosinophilic granulomatosis with polyangiitis
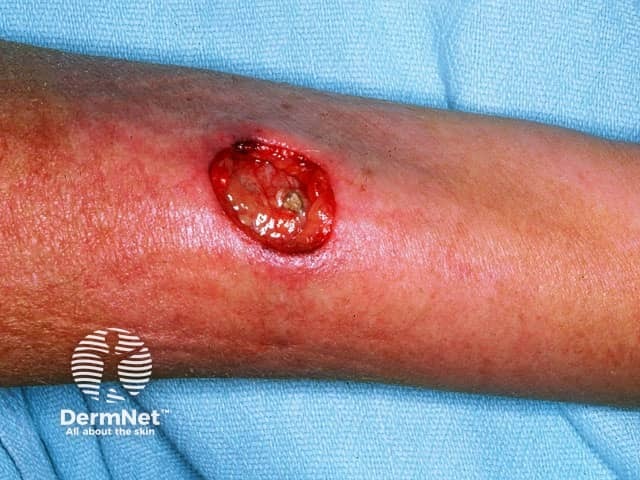
Eosinophilic granulomatosis with polyangiitis
There is no specific blood test for eosinophilic granulomatosis with polyangiitis. Investigations usually include:
Imaging studies may include X-rays of the lungs and sinuses, and electrocardiogram (ECG).
Skin biopsy and kidney biopsy may demonstrate the diagnostic combination of tissue eosinophilia, vasculitis and granulomas. See eosinophilic granulomatosis with polyangiitis.
Systemic corticosteroids are the first-line therapy for eosinophilic granulomatosis with polyangiitis. Mild disease may initially be treated with oral corticosteroids, but most authors suggest beginning therapy for extensive disease with intravenous (IV) corticosteroids. They are usually prescribed long-term.
The patient's response to corticosteroids is often dramatic. Within 1-2 weeks eosinophilia, the ESR and muscle enzyme levels may normalize. Corticosteroids can then be tapered, and remission is normally sustained. Low-dose prednisone may be continued for residual asthma or other symptoms.
If vasculitic symptoms are uncontrolled or if large doses of steroids are required, cyclophosphamide may be used. This appears to improve outcome in severe disease and may reduce the chance of relapse.
Other medications reported to be useful in eosinophilic granulomatosis with polyangiitis include:
Antibiotic prophylaxis with sulfamethoxazole-trimethoprim may be advised because intense immunosuppression increases the risk of infection.
Treatment of eosinophilic granulomatosis with polyangiitis with systemic steroids has improved the survival of patients from 50% at three years to 75% at eight years.
At least half of deaths in eosinophilic granulomatosis with polyangiitis are due to heart involvement.