Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Pityriasis alba is a common skin disorder in children (90%) and young adults. It is particularly prevalent in atopics. It is characterised by one or more flaky pink patches and hypopigmentation. The patches are often found on the cheeks and upper arms and are more noticeable in darker skinned children. It is generally asymptomatic.
The cause of pityriasis alba is unknown but is thought to be a type of dermatitis. The dry component may appear more obvious in winter months. The hypopigmentation is more obvious in summer because of relative tanning of unaffected skin.
After some weeks or months the dry surface resolves leaving a smooth pale patch, which slowly disppears over a year or so.
Pityriasis alba Pityriasis alba on the arms Pityriasis alba on the cheeks 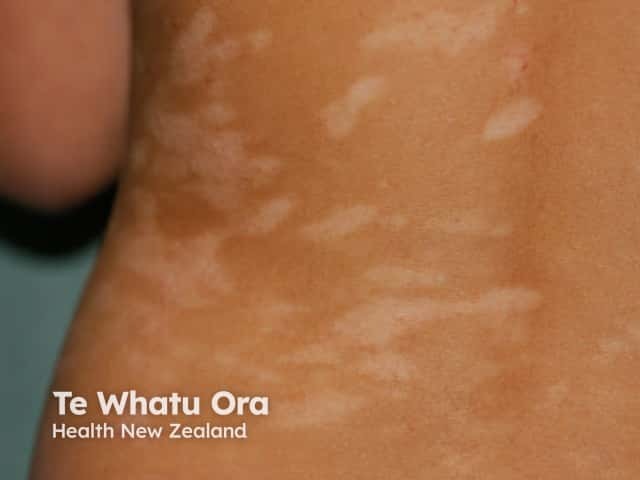
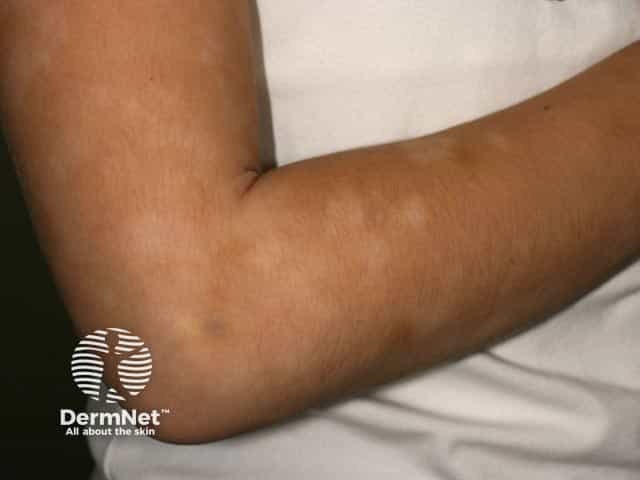
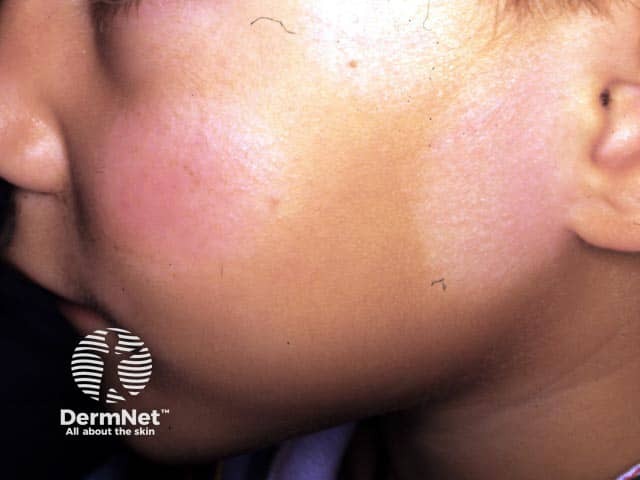
The differential diagnosis of pale dry patches on the face or limb of a child includes:
Mycology is negative in pityriasis alba, but may be necessary to rule out a dermatophyte infection or pityriasis versicolor.
Skin biopsy is rarely necessary and may be reported as nonspecific dermatitis.
No specific treatment is necessary in most children as the patches are asymptomatic and resolve by themselves.
A trial of mild topical steroid cream is sometimes warranted for a couple of weeks. It can be expected to reduce the redness, scaling and itch (if present). Long term, a moisturiser may prove as effective.
Sunscreens may be useful to reduce tanning of surrounding skin.
Assess the prevalence of pityriasis alba in a paediatric population.
Information for patients
See the DermNet bookstore