Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated January 2016. Revised September 2020.
Introduction Demographics Causes Clinical features Diagnosis Treatment Prevention Outlook
Pityriasis alba is a low-grade type of eczema/dermatitis mainly seen in children.
The name describes its appearance: pityriasis refers to the characteristic fine scale, and alba to its pale colour (hypopigmentation).
Pityriasis alba is common worldwide with a prevalence in children of around 5%.
The cause of pityriasis alba is unknown.
Researchers have not reached any conclusions about the relationship of pityriasis alba to the following:
Classic pityriasis alba usually presents with 1 to 20 patches or thin plaques.
Typically, a patch of pityriasis alba evolves through several stages.
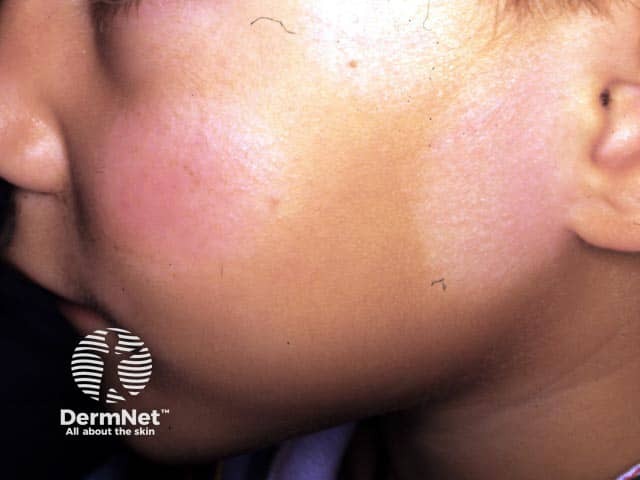
Pityriasis alba on the cheeks
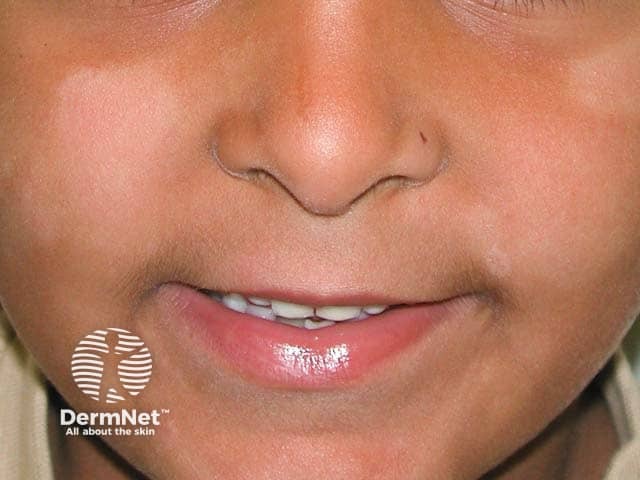
Pityriasis alba on the cheeks
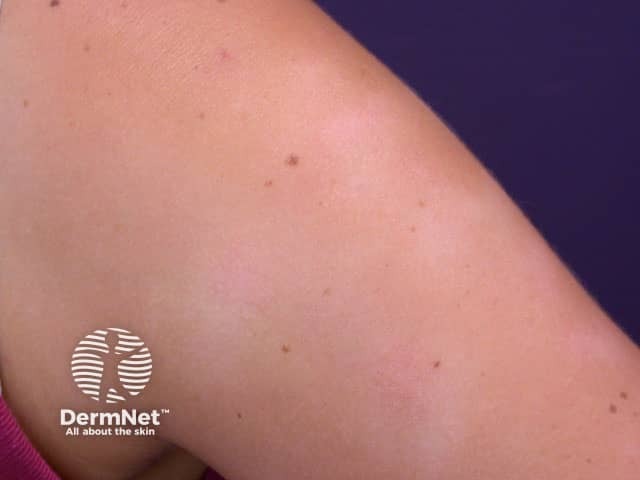
Pityriasis alba
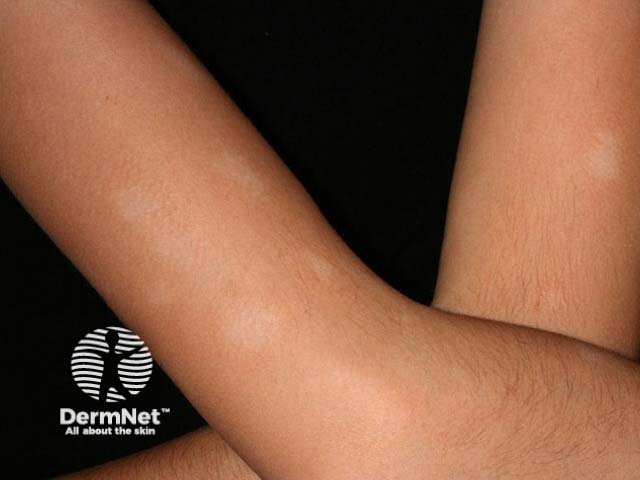
Pityriasis alba
See more images of pityriasis alba ...
Pityriasis alba is usually a clinical diagnosis but may be confused with several other disorders that cause hypopigmentation.
To exclude these, investigations may include:
No treatment is necessary for asymptomatic pityriasis alba.
The development or prominence of pityriasis alba can be reduced with sunscreen use to minimise sun tanning.
Pityriasis alba clears after an average of one year, with a range of a few months up to two or three years. The colour gradually returns completely to normal.