Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Basic photobiology
Created 2007.
Learning objectives
- Name bands within the electromagnetic spectrum
- Describe variations in ultraviolet radiation (UVR) at the earth's surface
- Describe effects of light on the skin
- Describe the response of the skin to UVR
- Define skin phototypes
- Describe photoprotective measures
Electromagnetic spectrum
The electromagnetic spectrum 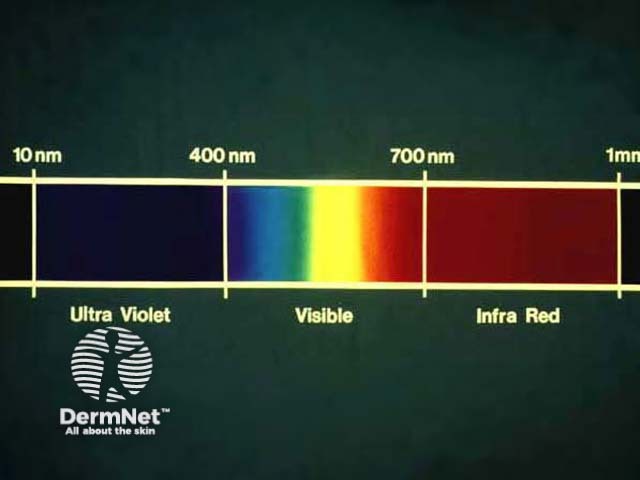
The electromagnetic spectrum emitted from the sun includes:
| Name | Wavelength (nm) | Comments |
|---|---|---|
| X-rays | 0-200 | |
| UVC | 200-290 | Not present at Earth's surface as removed by ozone layer. Germicidal band used in labs for sterilization. Very damaging to superficial skin. |
| UVB | 290-320 | Sunburning rays. Main cause of sun damage and skin cancer. |
| UVA | 320-400 | Long-wave black light tanning rays. Can penetrate into dermis. Contributes to erythema, skin aging and skin cancer. |
| Visible light | 400-760 | Does not significantly damage skin.
|
| Infra-red | 760-1000 | Heat |
| Microwave/ Radiowaves |
>1000 |
Ultraviolet radiation on earth
Most UVR is absorbed by the ozone layer or reflected back into space; in New Zealand, ozone (O3) is maximum in spring and minimum in early autumn. According to the National Institute of Water and Atmospheric Research (NIWA) ozone declined by 8% over New Zealand between 1980 and 1990. This has resulted in a summer-time increase in UV of approximately 9% per decade and is thought related to chlorine in the stratosphere.
Ultraviolet (UV) levels at ground level are greater when the sun is higher in the sky, as it passes through thinner atmosphere than when the sun is at a greater angle:
- At shorter latitudes (Auckland has more 5-10% UV than Invercargill)
- In summer (December, January and February)
- Monthly mean daily erythemal UV dose measured in Lauder in June 01 was 0.29 Kj/m2 compared to 4.51 Kj/m2in January 2002, according to Environment Reporting Programme.
- At midday (summer solar noon is at 1.30 pm in New Zealand).
About 30% of the daily amount of UVB is received between 12.30–2.30 pm and 78% is received 10.30 am –4.30 pm.
There is also greater total UV:
- When the conditions are clear, compared with cloud or smog
- With a reflective surface: snow reflects up to 80% incident UVB, and sand up to 25%.
- At altitude: there is 6% more UV at 1000 m than at sea level.
Variation is greater for UVB than for UVA.
Only 10% of the sunburning UVR is transmitted through standard window glass.
Measurements of UVR at Waikato Hospital in 1989
UV on a clear day Seasonal UV 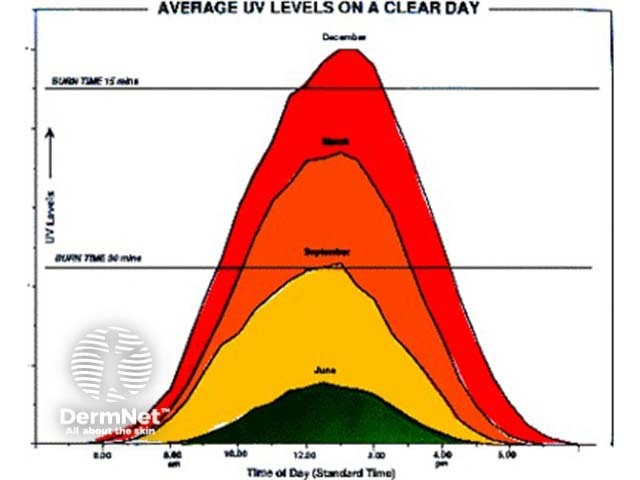
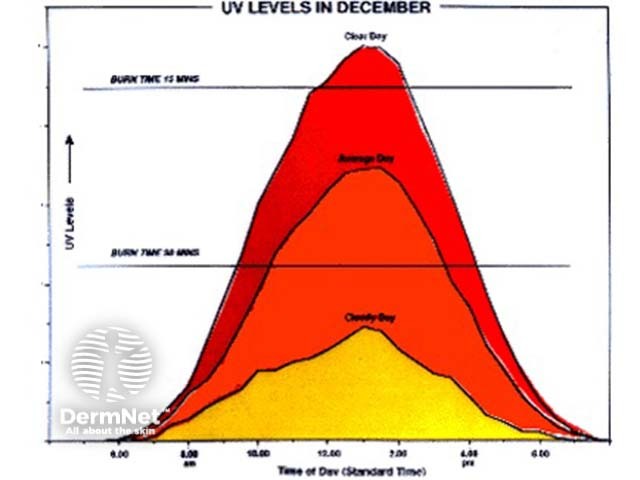
A: The difference in UVR on a clear day compared with a cloudy day, by time of day.
B: The difference in UVR in different seasons, by time of day.
Optics of the skin
UVR incident on the skin may be:
- Reflected
- Refracted
- Absorbed
- Scattered
- Transmitted
- Produce fluorescence
The total quantity of UVR transmitted through skin depends on:
- Wavelength of UVR
- Depth of measurement
- Direct and scattered UVR
UVR and the skin 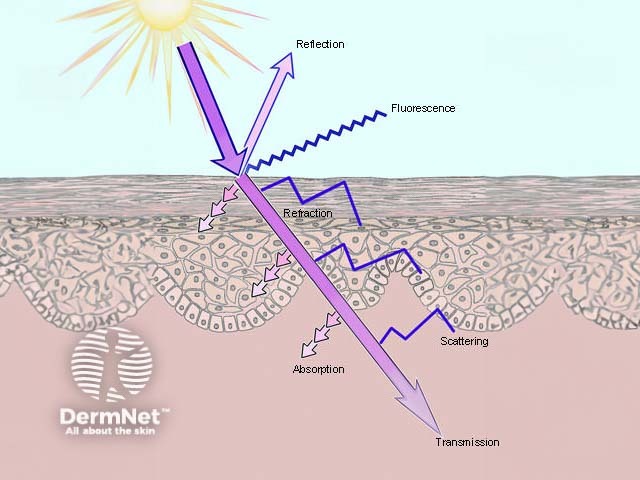
The biological effects of light on normal skin
UVR causes biological effects when it is absorbed. Target biomolecules are:
- Nucleic acids, resulting in dimers, adducts, hydrates and cross-links.
- Proteins
- Porphyrins
- Carotenoids
- Steroids
- Quinones
There are several repair mechanisms to UVR damage.
Acute response of skin to exposure to UVR
The acute response of the skin to exposure to UVR has rapid onset (minutes to days) and short duration (hours to weeks).
- Erythema (sunburn)
- Immediate pigmentation
- Delayed pigmentation (suntan)
- Vitamin D production
- Skin thickening
Erythema mainly results from UVB i.e. wavelengths <320nm. It arises from dilation of the superficial blood vessels. Solar-induced erythema is delayed by a few hours after exposure.
The mechanism that results in erythema is unknown. Possibilities include:
- Direct action on vessel wall
- Production of an epidermal chemical (?prostaglandins) that diffuses into the dermal vessels
Skin phototypes 1 to 6 are used to classify the effect of sun exposure on an individual's skin.
| Type 1 | Very fair. Burns easily, doesn't tan |
| Type 2 | Fair. Burns easily, tans lightly |
| Type 3 | Olive. Burns somewhat, tans readily |
| Type 4 | Light brown. Burns rarely, tans well |
| Type 5 | Dark brown. Doesn't burn, tans deeply |
| Type 6 | Black |
In skin types 4-6, immediate tanning may arise within minutes of exposure to long wave ultraviolet radiation (UVA) or visible light and is due to oxidation of pre-formed melanin in basal keratinocytes.
Delayed tanning is noticeable two days after exposure and most intense a week afterwards. It is due to melanogenesis and distribution of melanin to keratinocytes throughout the epidermis. UVA and even visible radiation may cause melanogenesis, but UVB is the most effective in initiating it.
Further exposure to UVR causes less damage:
- Melanin absorbs the UVR preventing it from reaching lower layers of the skin
- Epidermal keratinocytes proliferate so the skin becomes thicker (acanthosis)
UVB converts precursors in the skin into vitamin-D. The liver then the kidneys change vitamin-D into calcitriol (1,25 dihydroxycholecalciferol), which is required for calcium homeostasis.
Immune response
UVR results in profound alterations of both local and systemic immune responses.
- The immune changes are mainly mediated by cytokines released from epidermal cells, but also by neuropeptides released from sensory nerves in the skin.
- Targets include urocanic acid, cellular DNA, cell membranes.
- Neuropeptides may also play a role in the repair of cutaneous UV injury and in immunosuppression.
- The function of antigen-presenting cells (Langherhan's cells) is reduced.
- UV may cause apoptosis (cell self-destruction).
- UVR prevents primary contact sensitisation to surface antigens.
- It inhibits histamine release from mast cells.
- Suppressor T cells may induce tolerance contributing to the eventual development of skin cancers.
Chronic response to exposure to UVR
Sun damage (photoaging) includes:
- Dry coarse leathery appearance
- Loss of skin elasticity
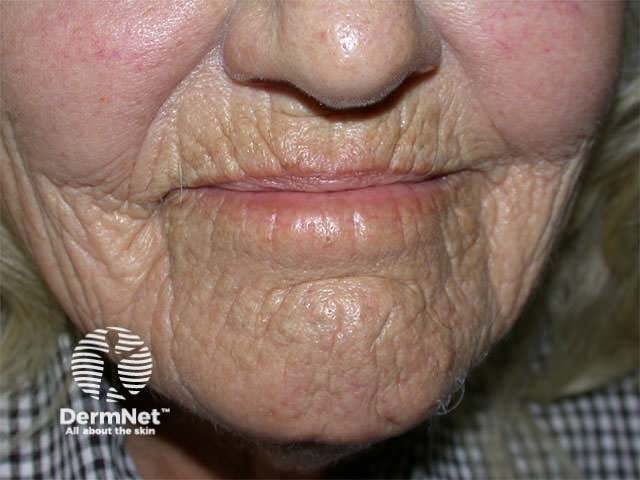
- Fine wrinkles
- Dilated capillaries and easy bruising
- Thin, transparent, fragile tissue
- Actinic keratoses
- Skin cancer (melanoma, basal cell carcinoma, squamous cell carcinoma)
Long-term effects of exposure to UVR
Thin skin Furrows Brusing Actinic keratoses Basal cell carcinoma Squamous cell carcinoma Melanoma 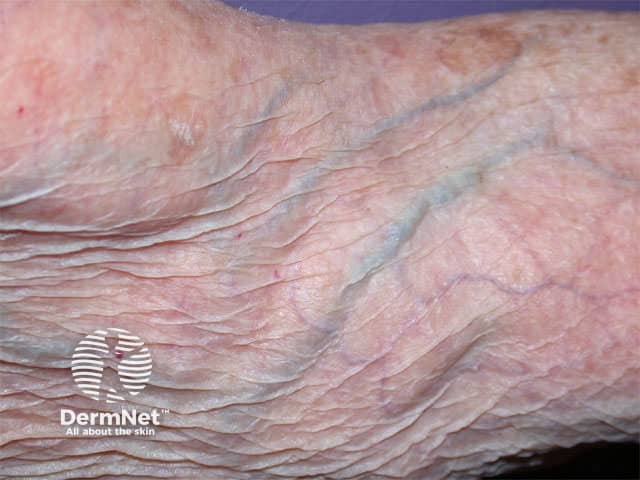
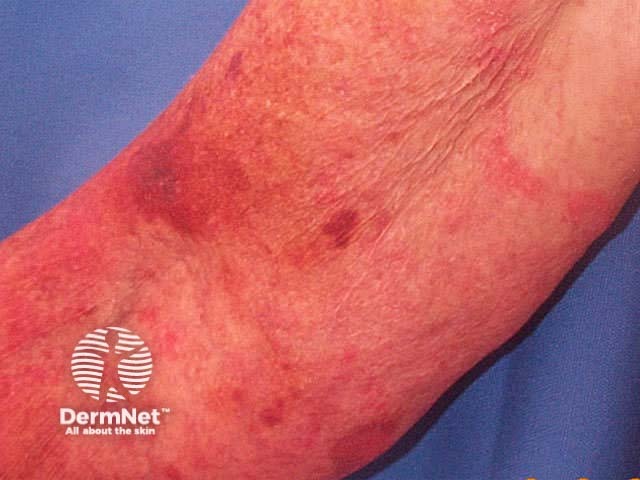
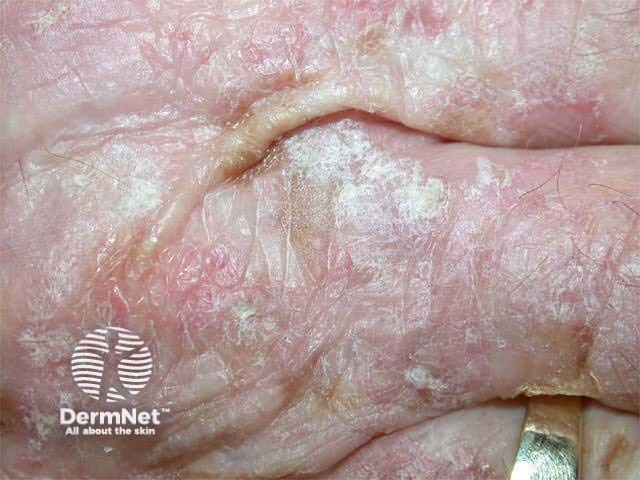
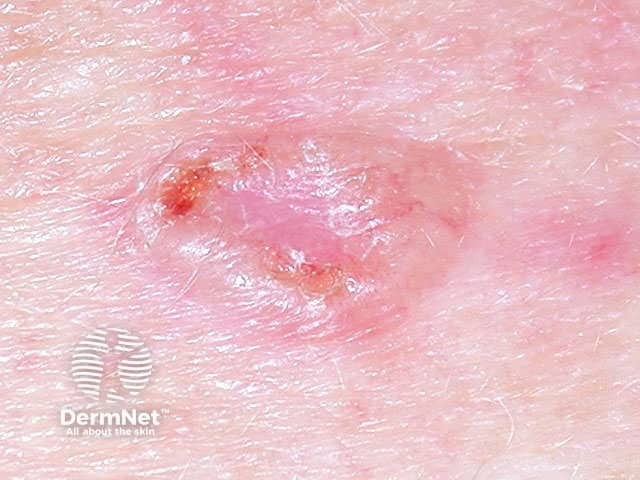
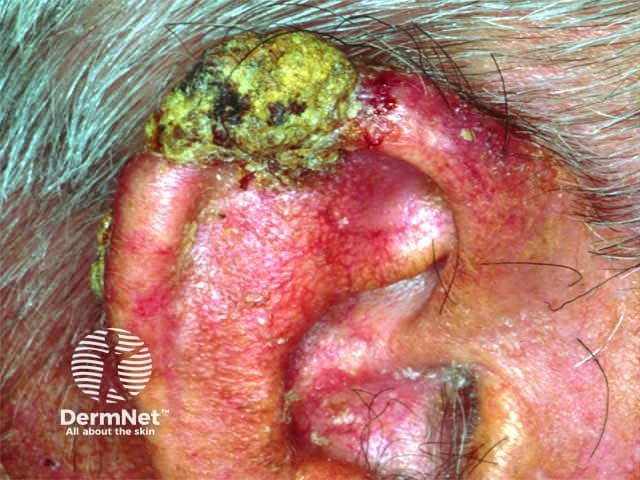
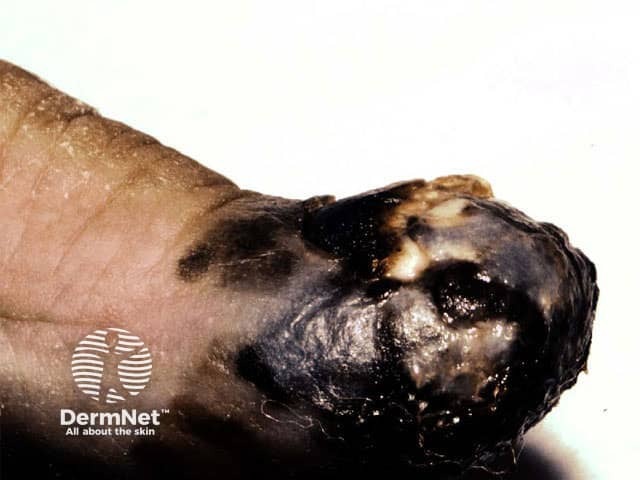
Skin cancers are induced by:
- UVB definitely
- UVA probably
A 5% increase in erythemally effective global UVR may result in a 15% increase in skin cancer in a susceptible population after about 60 years.
Photoprotection
The best protection from sun damage is to stay indoors. If outside, then protection from directly incident light can be obtained by seeking shade: trees, verandas, and umbrellas.
As much skin as possible should be covered with densely woven darkly coloured clothing.
- Wear a hat with a wide brim all round
- Fully covering top with long sleeves and high neck
- Long trousers or skirt
- Gloves, socks and shoes
Clothing as sun protection
Children with hats 
Apply sunscreen to all uncovered skin liberally. Reapply after half an hour to ensure an even coating soaks into the skin, and then follow the instructions on the container. These generally advise reapplication 2-hourly and after bathing.
Sun protective factors (SPF) are calculated from in-vivo testing, and are the ratio of the time for the skin to burn when exposed to solar simulating UVR with the sunscreen compared without the sunscreen. Thus white skin that normally burns in 10 minutes will burn in 150 minutes (2 1/2 hours) with SPF 15 sunscreen however often it is reapplied. In general, sunscreens are much less effective than predicted by their SPF number as they are applied significantly less thickly than is tested and are rubbed, sweated or washed off.
Desirable properties of the sunscreen include:
- Sun protection factor (SPF) 50+
- Broad spectrum protection against UVB and UVA
- Water resistance for 2 hours or more if swimming, bathing or sweating
- Non-comedogenic (i.e. it is not prone to aggravate acne)
- Cosmetically acceptable.
Activity
What are the required criteria for a sunscreen to comply with the Australian and New Zealand Standard?
References:
- Phototherapy resources
- Australian Photobiology Testing Facility
- Photobiology Online (POL) (The European and American Societies for Photobiology)
- New Zealand Standards 2604:1998(AS/NZS) Sunscreen products - Evaluation and classification (NZ$62.44)
On DermNet:
Information for patients
Other websites:
Books about skin diseases:
See the DermNet bookstore
