Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: August, 2025
Author: Orhan Yilmaz, University of Saskatchewan College of Medicine, Canada (2024)
Peer reviewed by: Dr James A. Ida, Dermatologist, Veterans Administration, United States (2025)
Previous contributor: Vanessa Ngan, Staff Writer (2005)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department.
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Cryptococcosis is a serious, invasive fungal infection caused primarily by two species of encapsulated yeasts: Cryptococcus neoformans and Cryptococcus gattii.
Cryptococcosis poses a significant global health concern due to its high rates of morbidity and mortality, particularly where effective antifungal treatments are not available.
Cryptococcus neoformans is considered an opportunistic pathogen and mainly affects immunocompromised individuals.
Causes of immunodeficiency commonly associated with cryptococcosis include:
In contrast, Cryptococcus gattii is known to cause cryptococcosis in individuals who appear to be immunocompetent.
C. neoformans and C. gattii are both distributed worldwide and thrive in warm, humid regions. High rates of infection are seen in regions such as sub-Saharan Africa, Southeast Asia, and parts of the Americas.
Cryptococcal infection of the central nervous system (CNS) is the leading cause of death among patients with advanced HIV/AIDS in sub-Saharan Africa.
C. neoformans
C. gattii
Other species, such as Cryptococcosus laurentii and Cryptococcosus albidus, have been rarely reported to cause cryptococcosis.
Cryptococcosis is typically acquired by inhaling spores or poorly encapsulated yeast cells from the environment.
Initial cryptococcal infection typically occurs in the lungs and may disseminate haematogenously to other organs, including the skin, with a strong tropism for the central nervous system (CNS). Immunocompromised individuals are at high risk of dissemination.
Primary cutaneous cryptococcosis (PCC):
Secondary cutaneous cryptococcosis (SCC):
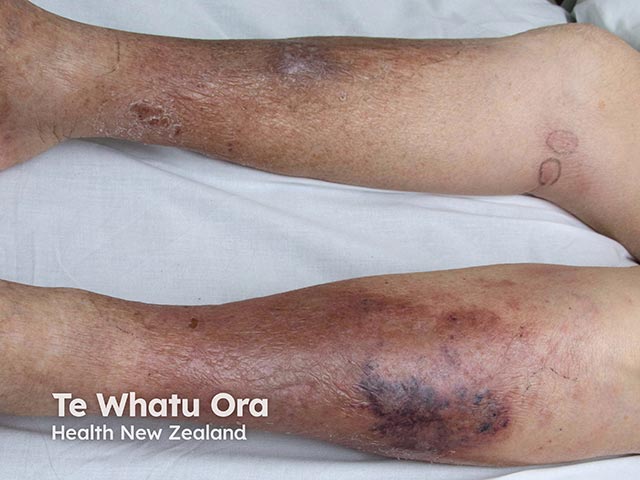
A haemorrhagic cellulitis-like eruption due to cryptococcosis (CFI-patient1)
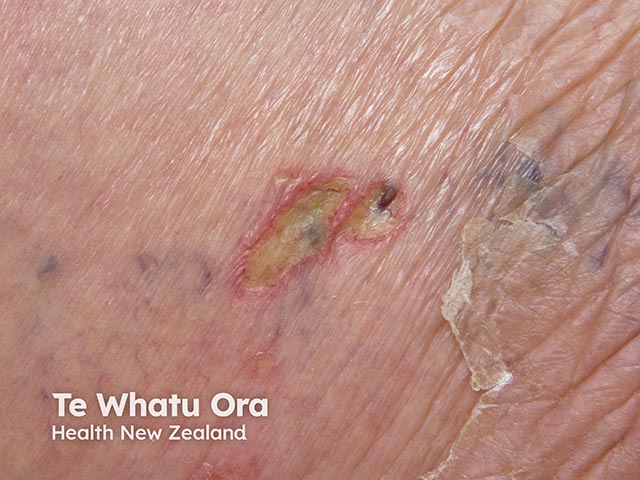
An ulcerated area due to cryptococcosis (CFI-patient1)
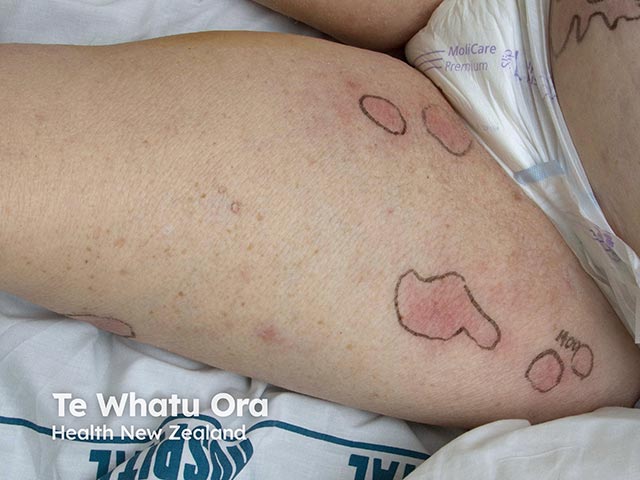
Spreading erythema due to disseminated cryptococcosis (CFI-patient1)
Papules, pustules, and purpuric lesions may be less evident on individuals with darker skin tones.
Nucleic acid sequence-based amplification (NASBA) and polymerase chain reaction (PCR) are emerging as reliable diagnostic methods.
Chest imaging (eg, X-ray, CT scan) may exhibit characteristic radiographic findings of pulmonary disease (eg, nodules or masses).
Differentials for cutaneous cryptococcosis include:
Cryptococcosis is treated with systemic antifungal therapy, and the regimen depends on the site of infection and immunological status of the patient. Treatment should be guided by current local or national infectious disease protocols.
CNS disease:
Pulmonary or disseminated disease (outside of the CNS):
There is no vaccine for cryptococcosis. Immunocompromised individuals should be advised to avoid environments in which Cryptococcus is commonly found eg, areas contaminated with bird droppings.
Early diagnosis and timely intervention are crucial for improving outcomes for those affected.
Patients with HIV:
Patients without HIV:
Despite aggressive antifungal treatment, CNS cryptococcosis often results in protracted neurological sequelae and requires extended monitoring to manage potential recrudescence (incomplete clearance of infection) or complications.