Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Reactions Diagnosis and testing
Author: Aamenah Al-Ani, Medical Student, University of Auckland, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. February 2018.
The classical tests for immediate type I hypersensitivity (allergy) are specific immunoglobulin E (IgE) antibody levels, such as the radioallergosorbent test (RAST), and skin prick tests. Although often performed in patients with asthma and hay fever, these tests are not applicable to atopic dermatitis, which is not caused by a type I reaction. However, the same allergens may also cause type IV or delayed hypersensitivity reactions.
An atopy patch test is an epicutaneous patch test with the type I allergens known to elicit IgE-mediated hypersensitivity reactions. Eczematous skin lesions, if any, are evaluated after 24–72 hours. Atopy patch tests can be used as a diagnostic tool in patients with atopic dermatitis triggered by aeroallergens or by food allergy [1,2].
Positive atopy patch tests are associated with allergen-specific T lymphocyte responses.
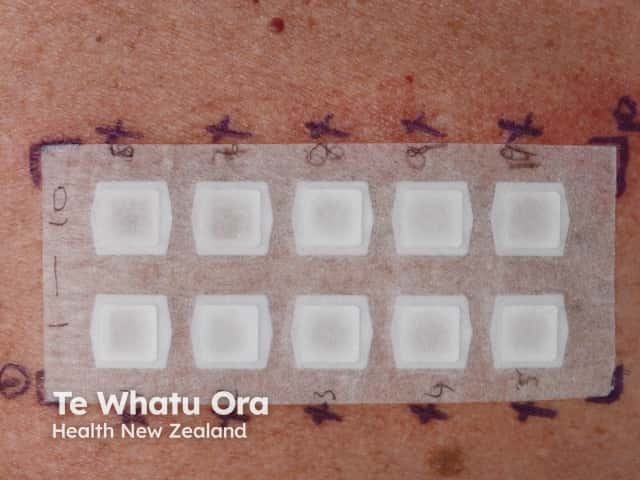
Patch tests applied to skin of upper back
The indications for atopy patch tests in a patient with atopic dermatitis include:
The atopy patch test technique is similar to usual patch tests used for the diagnosis of contact allergic dermatitis (which is a type IV hypersensitivity reaction).
Allergens are applied directly onto clinically uninvolved and untreated skin of the back. They remain in place for 48 hours. Tape stripping should be avoided [1].
The most common allergens tested in atopy patch tests are:
The European Task Force on Atopic Dermatitis (ETFAD) study in six European countries showed that the allergen that most often elicited a positive atopy patch test reaction was house dust mite extract, followed by pollen allergens [1].
Various vehicles are used to carry the allergen, including petroleum jelly, hydrogel and no vehicle. Allergens in petroleum jelly (petrolatum) generally elicit more positive atopy patch test reactions than allergens in a hydrophilic vehicle [1].
Evaluation of the patch test sites is conducted after 48 and 72 hours. The ETFAD grading system may be used to grade atopy patch tests; this grading system being:
There is no 'gold standard' for atopy patch tests. Positive results may correlate with a history of allergen-specific flares of dermatitis.
When compared with classic tests of IgE-mediated hypersensitivity, the atopy patch test has a higher specificity but a lower sensitivity. The classic tests may have some value as screening tests for IgE hypersensitivity, but the atopy patch test may add specificity.
The atopy patch test does not replace the classic methods of diagnosis of IgE-mediated allergy [1].
Predictors of positive atopy patch test reactions include: