Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu PhD. MD Candidate, Keck School of Medicine, Los Angeles, USA; Chief Editor: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, July 2016.
Introduction
Demographics
Causes
Clinical symptoms
Complications
Diagnosis
Treatment
Outlook
Chediak-Higashi syndrome is a childhood disorder that interferes with immune system function. It is also known as Begnez-Cesar syndrome, leukocyte anomaly albinism or defect in natural killer lymphocytes.
It was first described in 1943 by Dr Beguez-Cesar.
Chediak-Higashi syndrome is rare.
Chediak-Higashi syndrome is an autosomal recessive condition caused by a mutation on the LYST gene. It is often due to parental consanguinity. The LYST gene affects the creation and maintenance of storage granules and causes problems with the transport of a protein across cells.
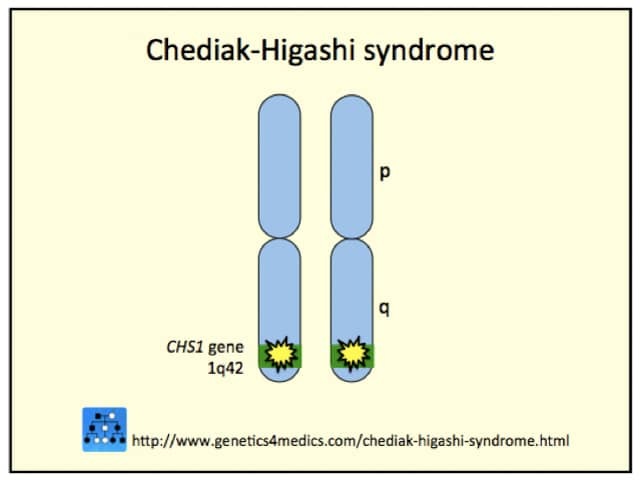
Chediak Higashi syndrome genetics*
*Image courtesy Genetics 4 Medics
Signs and symptoms begin to affect children with Chediak-Higashi syndrome shortly after birth or by age five at the latest.
Onset of Chediak-Higashi syndrome in adult life is associated with milder symptoms. These may include:
The majority of patients (around 80%) will undergo an accelerated phase of Chediak-Higashi syndrome. This phase is marked by the nonmalignant reproduction of white blood cells in multiple body organs. This accelerated phase can be precipitated by the presence of a viral infection, and it is often fatal if it occurs in childhood. This phase is called haemophagocytic lymphohistiocytosis (HLH).
Diagnosis of Chediak-Higashi syndrome is made by:
Treatment for Chediak-Higashi syndrome may include:
Without treatment, the outlook for Chediak-Higashi syndrome is poor. Around 50–85% of children with this disorder will enter the accelerated HLH phase. This process with fatal without treatment and most patients will die by the age of 10 years.