Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Sabrina Sapsford. Dermatology Research Fellow, New Zealand (2023)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Prevention Outcome
Consort allergic contact dermatitis (CACD) is a skin reaction that occurs on allergen exposure from another person. The ‘consort’ is the person carrying the allergen that causes the contact dermatitis via close contact.
Consort allergic contact dermatitis is also known as contact dermatitis by proxy or connubial contact dermatitis. Because the allergen originates from another person, careful history-taking to deduce the cause of contact hypersensitivity is required.
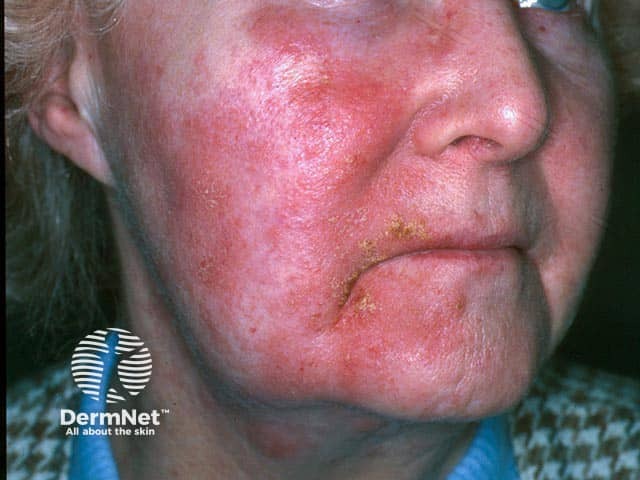
Facial contact dermatitis due to allergy to partner’s aftershave
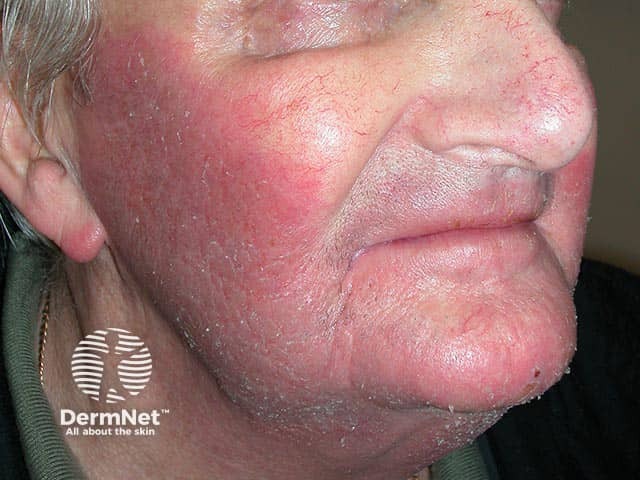
Facial contact dermatitis caused by fragrance in wife’s hair spray
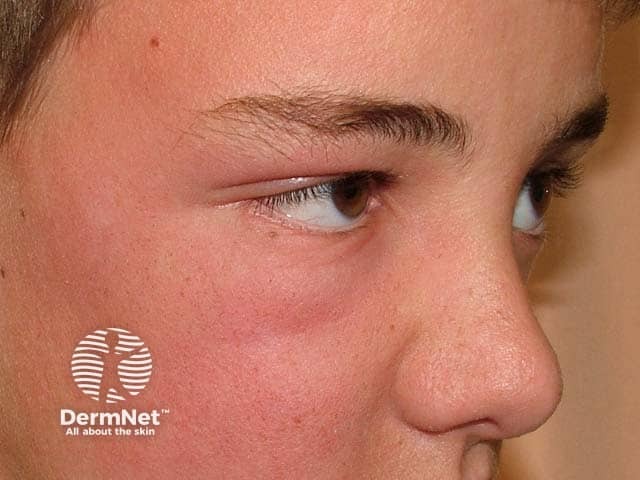
Facial dermatitis due to neomycin allergy after putting antibiotic drops into pet dog’s ears
Anyone can develop consort allergic contact dermatitis. However, allergic dermatoses are more common in patients with other atopic diseases such as hay fever, atopic dermatitis (eczema), and asthma.
Most patients with consort allergic contact dermatitis are women. The most common consorts are partners/spouses, children, healthcare workers, and carers.
Potential allergens include medications (36%), plants/botanicals (12%), fragrances (9%), and other occupational, cosmetic, or common household products.
In 80% of cases the patient has direct contact with the consort, resulting in a type 4 (cell-mediated) hypersensitivity reaction. Contact can also be indirect, for example, via clothing, sheets, or the environment.
Bedsharing partners may only be affected on the side of the skin exposed to the consort. One-third of partner-associated consort allergic contact dermatitis involves sexual contact and may be associated with condoms, lubricants, or feminine hygiene products. Semen can also rarely cause contact dermatitis.
History taking is important to deduce the cause of consort allergic reactions, including an occupational history of the patient and their close contacts. Associated occupations include manufacturing, pharmaceuticals, farming, hairdressing, and perfumery work.
The most common presentation of consort allergic contact dermatitis is an eczematous rash. Around 14% may develop a vesiculobullous rash. Other less common presentations include oedematous, nummular, follicular, and lymphomatoid dermatitis.
The distribution of the rash depends on the areas of the skin exposed to the allergen.
A high index of suspicion is required to diagnose consort allergic contact dermatitis; for example, a handprint-shaped rash may indicate exposure from the consort’s hand or glove.
Rather than appearing erythematous (red), consort allergic contact dermatitis may appear violaceous (purple) or mute (no added colour) in darker skin types.
Consort allergic dermatitis is diagnosed through careful history-taking. A patient’s close contacts and their occupational history, as well as sexual and other social factors, may be relevant.
Thorough examination of the rash is important. An unexpected pattern or distribution, or genital involvement, may suggest a consort allergic contact dermatitis.
Patch testing to determine or confirm the causative allergen can be helpful. An unexpectedly vigorously positive patch test in a patient with unexplained contact dermatitis may increase the index of suspicion for consort allergic dermatitis.
When an allergen is identified, the best treatment is avoidance of the allergen. This does not mean avoiding the consort. However, it does require identifying the allergen and mitigating the risk of exposure to those sensitised to that allergen.
This may require the consort to keep work uniforms at work, and showering after work if the allergen is occupational. Other strategies may include consorts avoiding causative cosmetics, household products, or contact with patients sensitised to medications soon after using those medications (or even changing medications if possible).
Other general measures:
Allergen avoidance, once identified, is key to prevent recurrence of symptoms.
With allergen avoidance, the reaction should resolve.