Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2005. Updated by Dr Sara de Menezes, Basic Physician Trainee, Alfred Health, Melbourne, Australia; Chief Editor: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, November 2016.
Introduction - lymphoma
Introduction - cutaneous B-cell lymphoma
Demographics
Skin signs
Diagnosis
Treatment
Outcome
Lymphomas are tumours of the lymph nodes and lymphatic system.
Primary cutaneous lymphoma can be broadly divided into two categories:
Primary cutaneous B-cell lymphomas (PCBCL) comprise approximately 20% of cutaneous lymphomas and are described on this page.
Cutaneous B-cell lymphomas are a malignant proliferation of lymphocytes of the B-cell type. Mutation occurring at different points in B cell development leads to different forms of lymphoma.
In 2005, the World Health Organization (WHO) and the European Organization for Research and Treatment of Cancer Classification (EORTC) reached a consensus classification for cutaneous lymphomas. It was revised by the WHO in 2008. The three main types of PCBCL are:
Rare cases of PCDLBCL that do not belong to the PCDLBCL-LT or PCFCL groups are categorised as PCDLBCL-other. Other entities such as anaplastic or plasmablastic lymphoma, primary cutaneous T-cell/histiocyte-rich B-cell lymphomas and primary cutaneous intravascular large B-cell lymphomas are very rare.
Due to differences in treatment and prognosis, it is important to discern between PCBCL and systemic forms of B-cell lymphomas that manifest with secondary skin involvement.
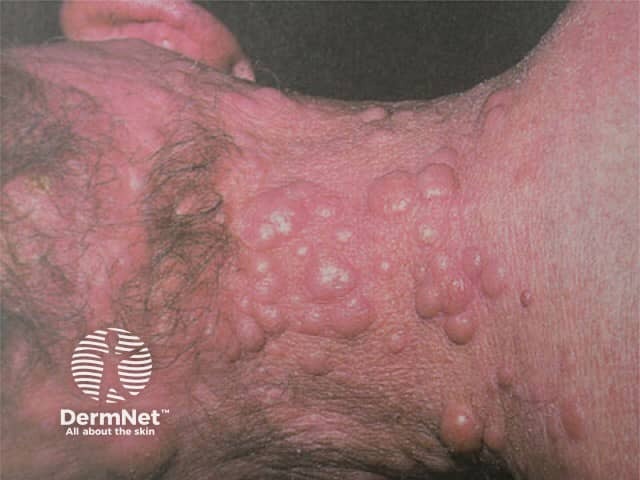
FC lymphoma

Cutaneous B-cell lymphoma

Cutaneous B-cell lymphoma
See primary cutaneous marginal zone B-cell lymphoma (PCMZL).
PCMZL is a low-grade malignant B-cell lymphoma of the MALT (mucosa-associated lymphoid tissue) type.
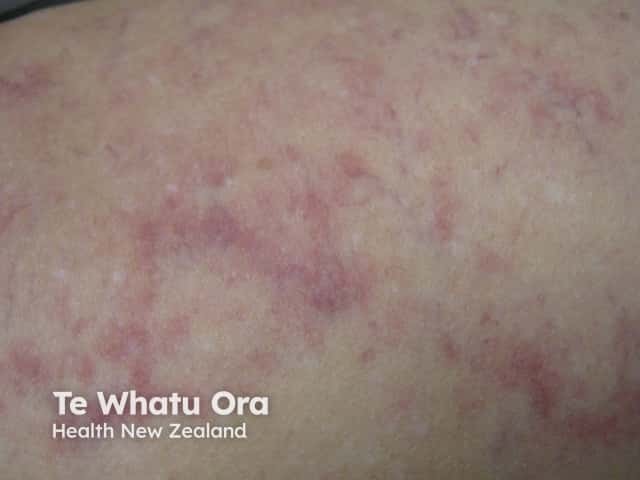
Intravascular B-cell lymphoma

Intravascular B-cell lymphoma
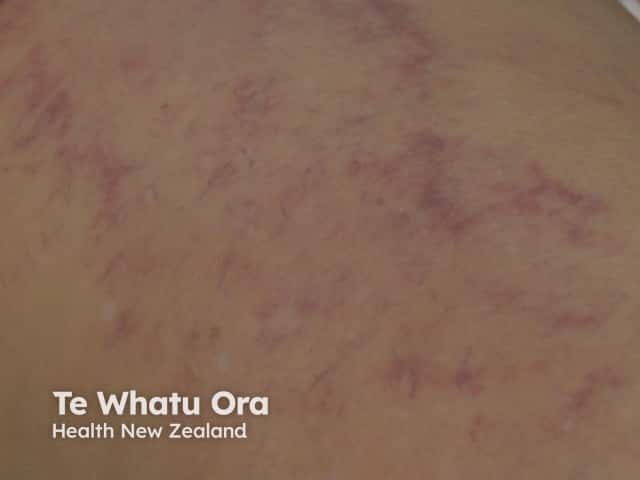
Intravascular B-cell lymphoma
The work-up of PCBCL should include a complete history, physical and skin examination. Initial blood tests should include:
If the full blood count shows lymphocytosis, peripheral blood flow cytometry may be needed.
An adequate skin biopsy is also important for evaluation and staging. Either 4–6 mm punch, incisional, or excisional biopsies should be obtained and should include the reticular dermis and subcutaneous fat. Superficial biopsy specimens may not differentiate PCBCL from reactive or inflammatory processes.
Assessment for extra-cutaneous involvement should be done, particularly in patients with palpable lymphadenopathy.
Any lymph node identified on imaging > 1.5 cm in length or showing high PET activity should undergo a biopsy; an excisional biopsy is preferred where possible.
Histologically, PCBCL shows a diffuse monotonous population of centroblasts and immunoblasts. Histochemistry tests are essential to classify the exact type of lymphoma.
PCFCL needs to be differentiated from a secondary cutaneous lymphoma, which is where a nodal follicular lymphoma has spread to involve the skin. Cellular morphology may vary with the age and size of the lesion.
Histologically, PCFCL shows:
Immunostaining shows:
A FISH analysis is unhelpful.
The histology of PCMZL consists of:
Immunostaining shows
PCFCL and PCDLBCL-LT have diffuse large B-cell infiltrates. PCDLBCL-LT shows:
Histopathological differential diagnoses should include:
Immunostaining shows:
The FISH analysis shows translocations of myc, Bcl-6 and immunoglobulin H genes.
The rarity of PCBCL and lack of comparative prospective, randomised studies limits the choice of therapy as most treatments are based on data from small retrospective studies. The European Organisation for Research and Treatment of Cancer Cutaneous Lymphoma Group (EORTC-CLG) and the International Society for Cutaneous Lymphoma (ISCL) have uniform recommendations on treating the three main types of PCBCL. Treatment is also influenced by whether the lesion is single or limited to a single site.
Without any treatment, PCFCL lesions may be stable, gradually enlarge, or rarely, regress. The histological growth pattern does not influence survival or treatment choice.
The recommended therapies for PCMZL are similar to PCFCL.
Localised or solitary leg-type B-cell lymphoma is usually are treated with local radiotherapy alone or in conjunction with R-CHOP.
Generalised PCDLBCL-LT can be treated with R-CHOP and/or local radiotherapy. Response rates are high but relapse rates are > 58% Around 30% develop extracutaneous disease.
Trials are assessing the efficacy of biological agents like ofatumumab, lumilixumab, dacetuzumab and intralesional TG1042 in the treatment of PCDLBCL-LT.
Very rarely, PCMZL can transform into DLBCL.