Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
DermNet, August 2021. Copy edited by Gus Mitchell.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Primary cutaneous follicle centre lymphoma (PCFCL) is a low-grade primary cutaneous B-cell lymphoma, defined as a lymphoma of germinal centre B-cells without extracutaneous involvement at the time of diagnosis.
Primary cutaneous follicle centre lymphoma is the most common type of primary cutaneous B-cell lymphoma (PCBCL), accounting for 50%, and the second most common cutaneous lymphoma in the Western world. It accounts for 10–20% of all cutaneous lymphomas.
PCFCL mainly affects middle-aged white men (50–60 years of age). It is extremely rare in children.
Primary cutaneous follicle centre lymphoma has been associated with infections including Epstein-Barr virus, Helicobacter pylori, and Borrelia burgdorferi. It is a form of non-Hodgkin lymphoma.
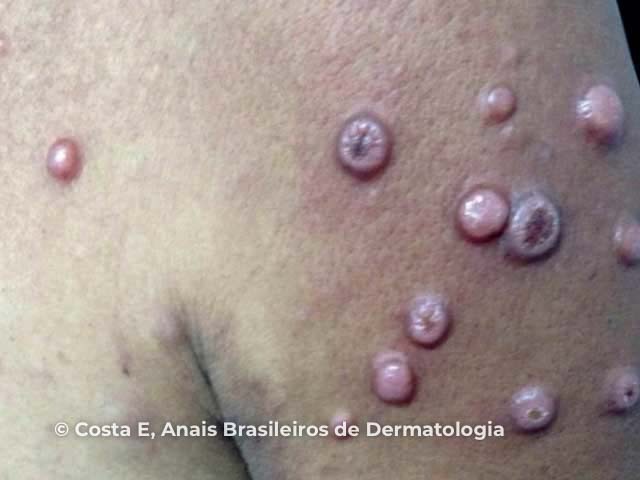
Figure 1
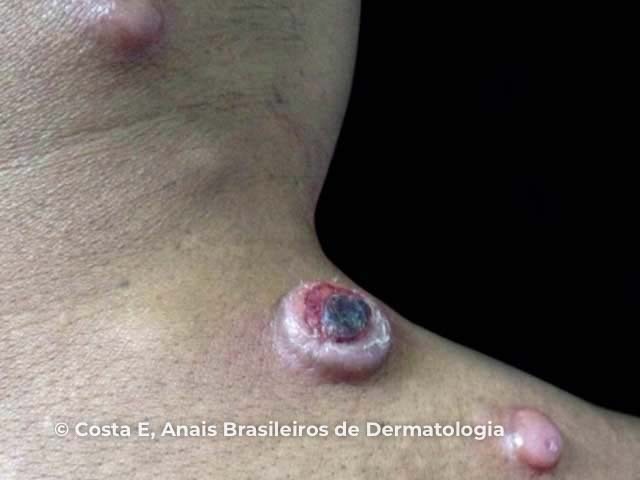
Figure 2
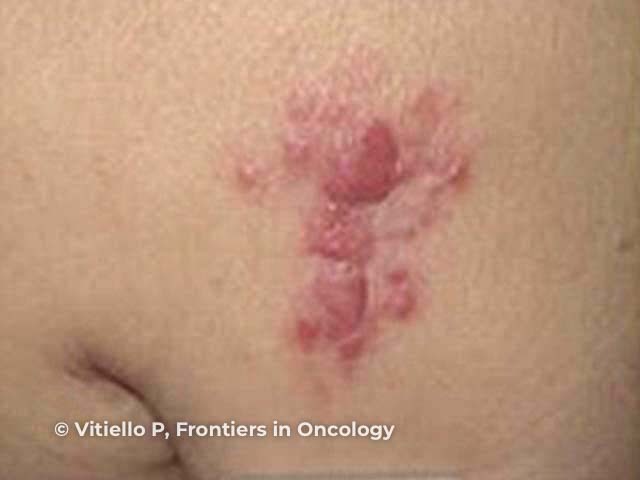
Figure 3
Figures 1&2: Costa EPW, Lucena BD, Amin GA, Bittencourt MJS, Dias LB Junior, Pires CAA. Primary cutaneous follicle center lymphoma. An Bras Dermatol. 2017;92(5):701–3. Figure 3: Vitiello P, Sica A, Ronchi A, Caccavale S, Franco R, Argenziano G. Primary cutaneous B-cell lymphomas: an update. Front Oncol. 2020;10:651.
Primary cutaneous follicle centre lymphoma may be suspected clinically but is usually diagnosed on skin biopsy. Histology, immunohistochemistry, and molecular studies show:
Further investigations may include:
Follow-up should be undertaken every 6 months including complete skin examination and lymph node palpation.
Primary cutaneous follicle centre lymphoma has an excellent prognosis. PCFCL may be stable, but lesions usually gradually enlarge if untreated and become locally aggressive. In rare cases, lesions may regress spontaneously.
The 5-year survival is >95%, or 40% if there is leg involvement.