Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Caroline Mahon, Dermatology Registrar, Christchurch, New Zealand, 2011. Acknowledgements: The article was reviewed and improved by the following people: Cara Hafner, RN, IBCLC Lactation Consultant Christchurch Women's Hospital; Marcia Annandale, IBCLC. Independent Lactation Consultant, Christchurch, New Zealand. Updated by Dr Catherin Nelson-Piercy. April 2018. Copy edited by Gus Mitchell. DermNet Update July 2021
Introduction Demographics Causes Common problems Associated mucocutaneous conditions Treatment Outcome
There are many proven benefits for infants and mothers who breastfeed. Breastfeeding should be encouraged and supported wherever possible. Women with longstanding or severe skin conditions should be counselled during their pregnancy about the care of their skin disease postpartum and specifically during lactation.
Women with a lesion on the nipple may find this interferes with breastfeeding or a pre-existing dermatosis localises to the nipples and/or areolae.
Changes in treatment required during pregnancy and/or lactation may result in poor control of a pre-existing inflammatory skin disorder.
Nipple hypersensitivity is common during the first postpartum week. Usually, this peaks at Day 3–6 and then subsides. Unlike nipple hypersensitivity, pain in the first two weeks postpartum is most commonly due to trauma to the nipple secondary to poor breastfeeding technique. This is associated with nipple redness, swelling, and cracking. Injury may range from superficial abrasions to tissue breakdown, a ‘compression stripe’ or shallow fissures, to deep erosions through to the dermis complicated by infection.
A nipple suction injury that does not heal with a change in breastfeeding technique may be a sign of infection. Staphylococcus aureus is the most common infection and may enter the milk ducts via injury to the nipple, leading to infective mastitis or breast abscess.
Dry, irritated, and itchy nipples are a common problem during lactation. Postpartum women can have increased skin sensitivity to environmental contact irritants and allergens, and those with atopic dermatitis can present with an atopic flare of nipple eczema. Topical steroid ointment should be applied sparingly after a breastfeed.
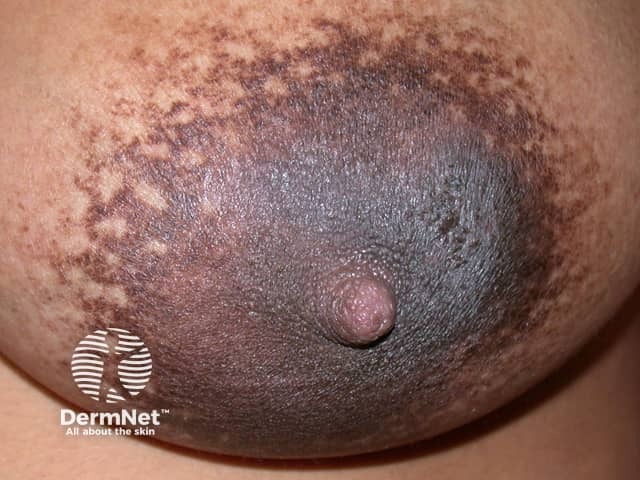
Nipple eczema
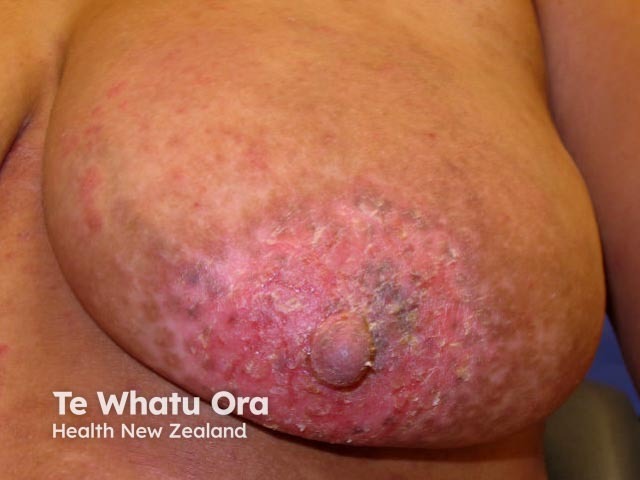
Nipple eczema
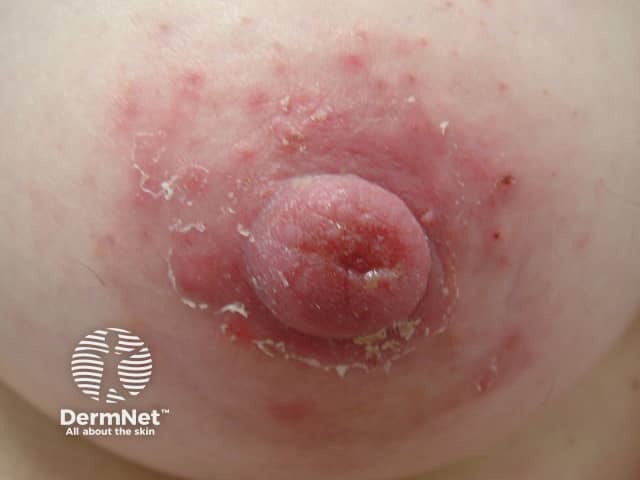
Nipple eczema
This is common in women who are experiencing difficulty with breastfeeding. Vasospasm in the vessels of the nipple results in colour change in the nipple and stabbing shooting pain. This is often triggered by an initial injury to the nipple but may also be a response to cold as a manifestation of Raynaud phenomenon. This can be managed by using warm, dry compresses and avoiding cold. Some women find squeezing the nipple base and massaging forward can restore blood flow and prevent a painful episode.
Montgomery glands are a normal part of breast anatomy. These glands enlarge in pregnancy (Montgomery tubercles) and secrete sebaceous material which lubricates and protects the nipples and areolae in pregnancy and lactation. Mothers should be advised that these should not be squeezed. A small amount of breast milk is also secreted via these tubercles. They may become obstructed, inflamed, or infected during lactation. Warm compresses and massage are commonly all that is required.
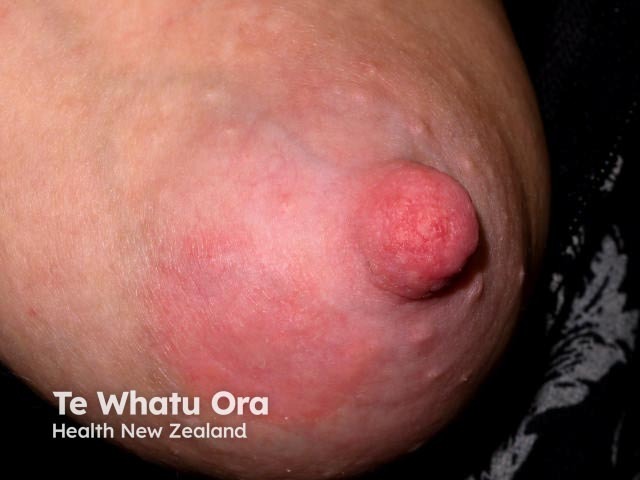
Montgomery tubercles and eczema
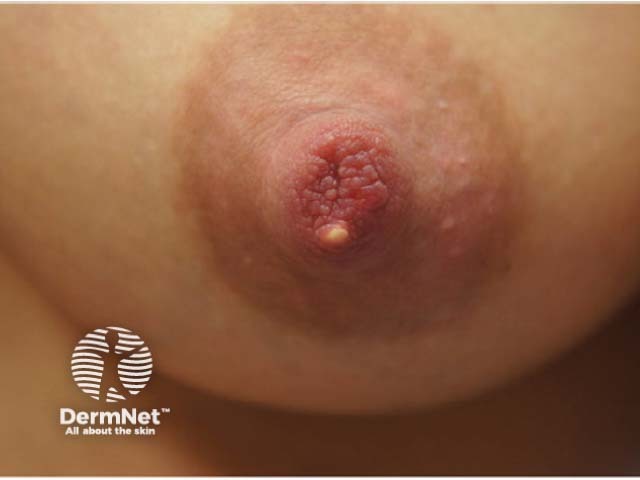
Nipple bleb
Image of nipple blebs reproduced with permission: Mitchell KB, Johnson HM. Breast pathology that contributes to dysfunction of human lactation: a spotlight on nipple blebs. J Mammary Gland Biol Neoplasia. 2020;25(2):79–83.
Blebs or white spots on the nipple (nipple blebs) are milk blisters due to sticky breast milk forming a plug within the milk duct. These usually appear as white, clear, or yellow dots on the nipple with pain often focussed at the spot or directly behind it. The obstruction may progress to mastitis. Warm compresses may be sufficient to dislodge the plug. Occasionally a plugged milk duct may require disimpaction using a sterile needle.
Nipple candidiasis is over-diagnosed. Nipple candidiasis is rare, presenting with late onset of new nipple pain and generally coincides with oral candidiasis in the breastfeeding infant. Mother or infant may be asymptomatic. Both infant and mother require treatment.
Psoriasis — may flare during lactation and present on the nipple due to koebnerisation of nipple trauma
Herpes simplex infection — presents as a painful vesicular eruption on the nipple or areola, and can be transmitted to the breastfeeding infant
Scabies — scabietic burrows can be found on the nipple and the mite may infest the baby via skin-to-skin contact
Mammary Paget disease — usually an older woman and involves just one nipple.
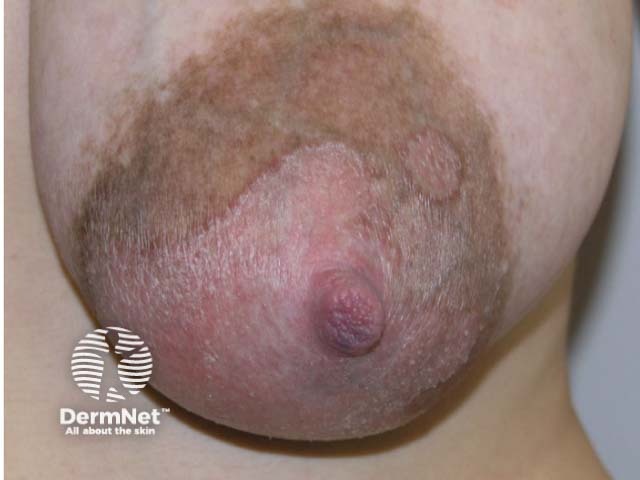
Psoriasis of the nipple
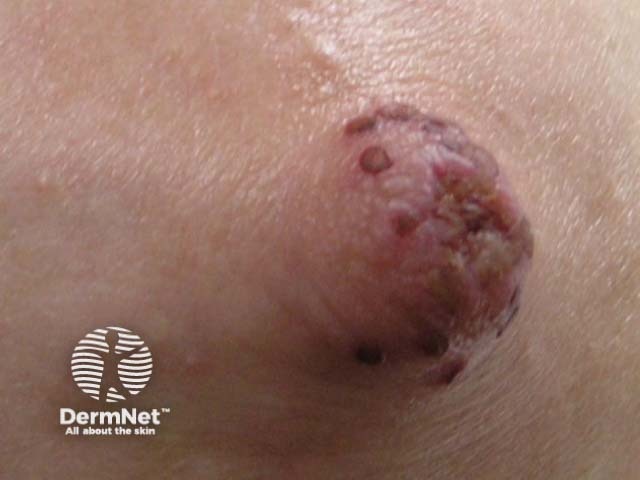
Herpes simplex of the nipple
Images of nipple psoriasis and herpes simplex of the nipple reproduced with permission: Barrett ME, Heller MM, Fullerton Stone H, Murase JE. Dermatoses of the breast in lactation. Dermatol Ther. 2013;26(4):331–6.
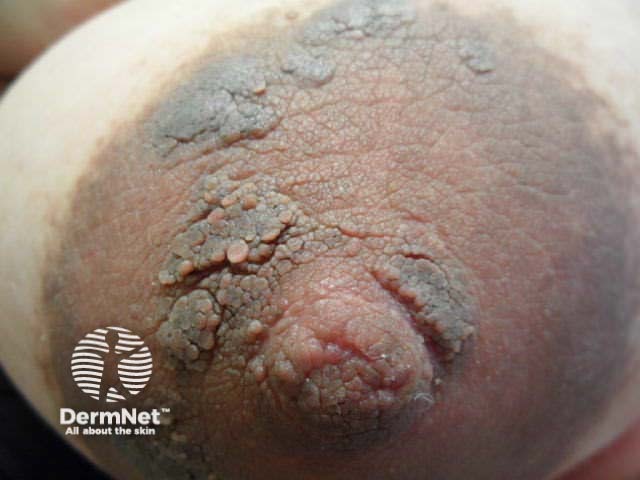
Hyperkeratosis of the nipple
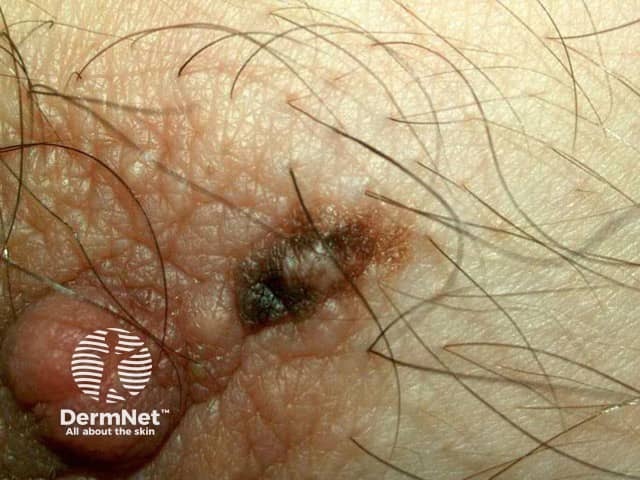
Nipple naevus
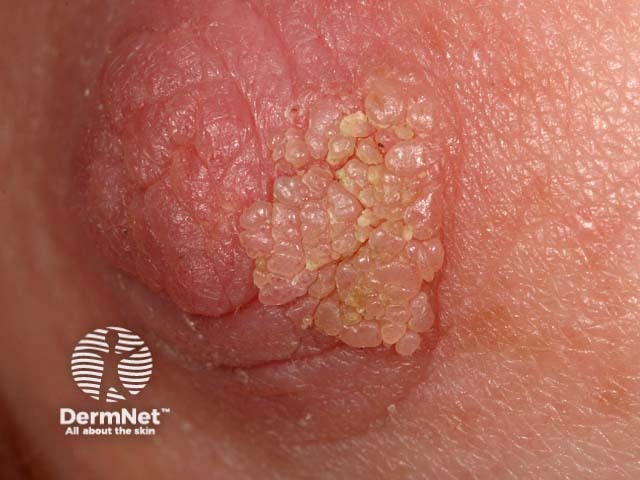
Nipple papilloma
Vaginal dryness with subsequent discomfort is a common problem in the postpartum period (atrophic vulvovaginitis). Intercourse may be painful (dyspareunia) and there may be splitting or fissuring of the posterior fourchette (at vaginal entrance). The use of vaginal moisturisers or water-based or petroleum-based vaginal lubricants can reduce discomfort during intercourse but may cause irritation. Petroleum-based products can cause condom breakage so should be avoided if depending on barrier method contraception.
Mastitis is inflammation of the breast caused by obstruction to milk flow progressing to infection and ultimately abscess formation. Staphylococcus aureus is the most common cause of infective mastitis. In early mastitis, there is breast pain and swelling. Red streaks may be visible in the skin of the breast overlying the mastitis. Systemic symptoms suggesting infection include malaise, fever, and chills. Breast milk may appear grainy or stringy, occasionally with visible mucus, pus, or blood.
Common risk factors associated with mastitis include:
It is important to identify mastitis early and address the underlying cause(s). Recognising risk factors is vital. Progression to breast infection may be averted, and antibiotic therapy may not be required.
It is important breastfeeding continues. Frequent breast milk removal with the infant at the breast and via breast pump is essential in preventing milk stasis. Complete emptying of the breast will assist in recovery.
Assessment with an experienced midwife or lactation consultant for:
Without appropriate expert advice, early cessation of breastfeeding is an unfortunate outcome that could be avoided.