Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2003 by Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand. Latest update by Dr Jannet Gomez, March 2017. DermNet Revision October 2021
Introduction
Demographics
Causes
Clinical features
Diagnosis
Treatment
Oral candidiasis is a fungal infection of the mouth often called 'thrush' because its white spots resemble the breast of the bird with the same name.
Although candida is present in 50% of the normal flora of healthy mouths, it causes infection (candidiasis) when increased numbers of yeast cells invade the mucosa.
Risk factors for developing oral candidiasis include:
Oropharyngeal candidiasis is reported in hospitalised and asymptomatic COVID-19 patients.
The usual organism is Candida albicans, but at least seven other species of Candida can also cause oral candidiasis including C. tropicalis, C. glabrata, C. kruesi, and others. C. dubliniensis is also reported in HIV patients. See Non-albicans candida infections.
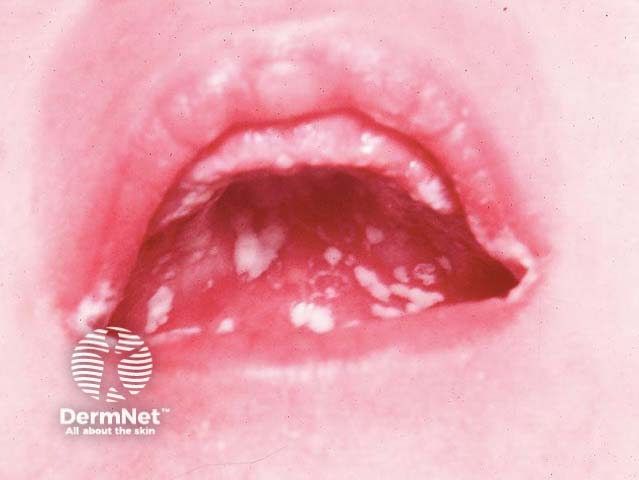
Oral thrush
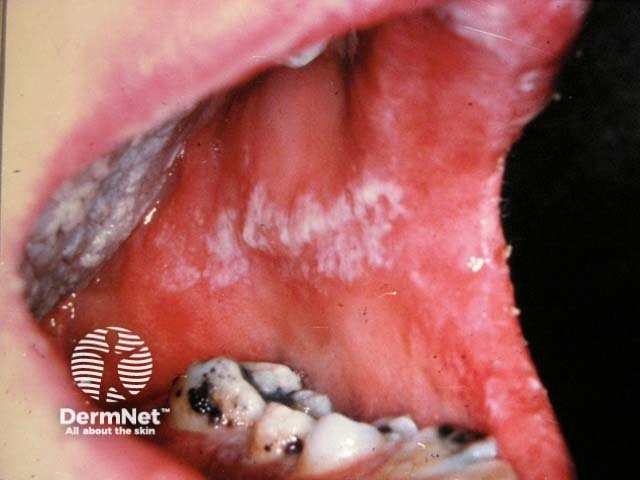
Oral candidiasis
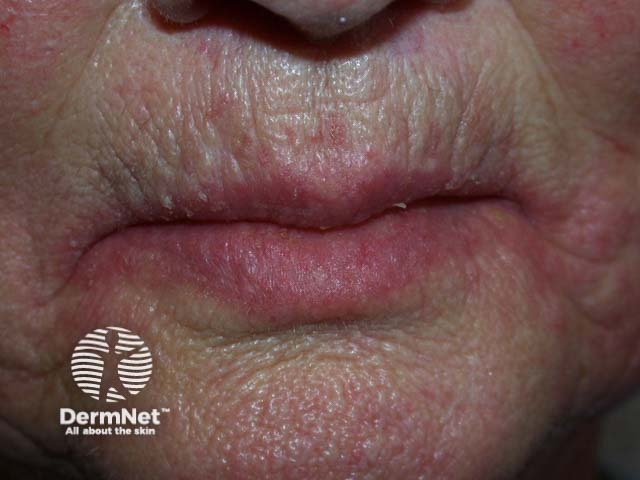
Angular cheilitis
More images of oral candidiasis.
Candida may arise suddenly as an acute infection or persist for long periods as a chronic infection.
Severe infections may extend down the throat (oesophageal infection) and cause difficulty with swallowing.
Microscopy and culture of skin swabs and scrapings aid in the diagnosis of candidal infections. However, as candida can live on a mucosal surface quite harmlessly, clinical correlation is required. It may also secondarily infect an underlying disorder.
In extensive oral candidiasis, endoscopy is performed to see the extent of the lesions into the gastrointestinal tract.
Practice good oral hygiene.
Denture wearers:
Mouthwashes with anti-candidal activity include:
Topical antifungal products for oral candidiasis include:
Treatment should be continued for 1–4 weeks or until symptoms have been clear for 7 days.
Systemic treatments include: