Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Anoma Ranaweera, Medical Writer, Auckland, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. March 2019.
Introduction Introduction How it works Indication How to use Contraindications Warnings and precautions Dosage modification Use in specific populations Potential drug interactions Possible side effects Immunogenicity
Hereditary angioedema is a rare, autosomal dominant disease that is associated with a deficiency or dysfunction of C1-esterase-inhibitor (C1-INH) activity. Hereditary angioedema causes spontaneous, recurrent, and potentially life-threatening swelling in various regions of the body, including the larynx.
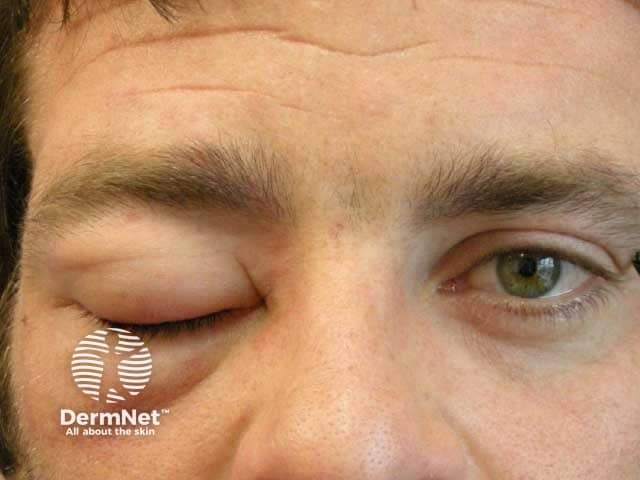
Unilateral lid angioedema
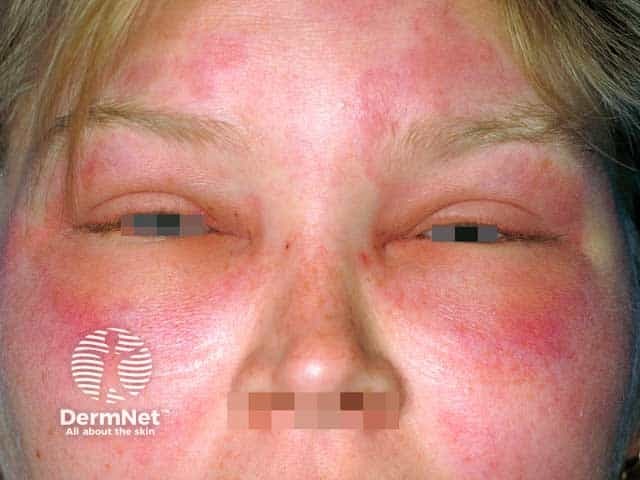
Lid angioedema - there was typical urticaria elsewhere on the body
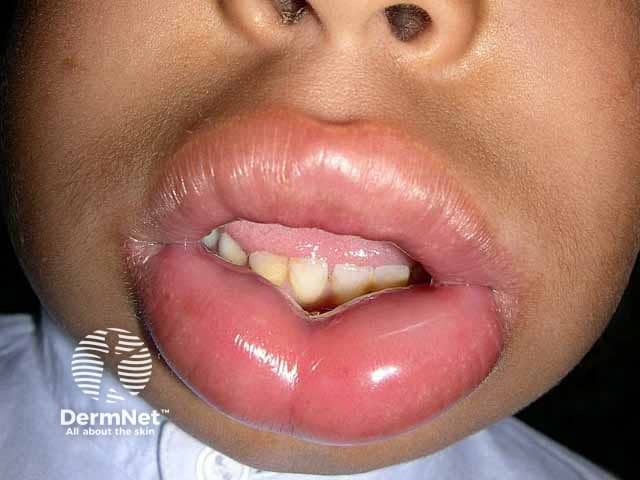
Severe lip angioedema
Lanadelumab (also called lanadelumab-flyo) is a prescription biological treatment used in patients aged 12 years and over to prevent severe swelling attacks due to hereditary angioedema. It is the first monoclonal antibody available for hereditary angioedema.
Lanadelumab was approved by the US Food and Drug Administration (FDA) in August 2018, in Canada in September 2018, and by the European Commission in November 2018. Regulatory applications for marketing lanadelumab are also being considered in Australia. Lanadelumab is not currently available in New Zealand.
Lanadelumab is marketed under the brand Takhzyro™ by Dyax Corp (a subsidiary of Shire) based in Burlington, MA, USA.
Lanadelumab is a fully human immunoglobulin G1, kappa light chain monoclonal antibody that provides targeted inhibition of plasma kallikrein, a critical regulator of hereditary angioedema attacks.
Lanadelumab is indicated to prevent recurrent attacks of hereditary angioedema in patients aged 12 years and older.
Lanadelumab may be self-administered by the patient or administered by a caregiver after undergoing training on subcutaneous injection technique by a healthcare professional.
The main contraindication to lanadelumab is hypersensitivity to the active substance or to any of the excipients.
To improve the traceability of biological medicinal products, the name and the batch number of the administered lanadelumab should be clearly recorded.
Hypersensitivity reactions to lanadelumab have been observed. In case of a severe hypersensitivity reaction, the administration of lanadelumab must be stopped immediately and appropriate treatment initiated.
Lanadelumab is not intended for the treatment of acute attacks of hereditary angioedema. In the case of breakthrough angioedema, individualised treatment should be initiated with approved rescue medication.
There are no available clinical data on the use of lanadelumab in hereditary angioedema patients with normal C1-INH activity.
No studies have been conducted in patients taking lanadelumab who have severe renal impairment. Renal impairment is not expected to affect the exposure to lanadelumab or its safety profile. No dose adjustment is required in patients with renal impairment.
No dose adjustment is required in patients taking lanadelumab who have hepatic impairment. Hepatic impairment is not expected to affect exposure to lanadelumab. There are no studies in patients with moderate or severe hepatic impairment.
No dose adjustment is required for patients above 65 years of age because age is not expected to affect the exposure to lanadelumab.
The safety and efficacy of lanadelumab in children aged less than 12 years have not been established. No data are available.
There are no available data on the use of lanadelumab in pregnant women to inform any drug-associated risks. Monoclonal antibodies such as lanadelumab can cross the placenta during the third trimester of pregnancy with potentially harmful effects on the fetus. Studies of lanadelumab in pregnant cynomolgus monkeys, treated with 33 times the maximum recommended dose for humans, revealed no evidence of harm to the developing fetus.
It is not known whether lanadelumab or its metabolites are excreted in human milk. Because many drugs are excreted in human milk, mothers should discontinue nursing prior to using lanadelumab. Available pharmacokinetic data in cynomolgus monkeys have shown excretion of lanadelumab in milk at approximately 0.2% of the maternal plasma level.
The safety and efficacy of lanadelumab in children under 12 years of age have not been established.
In clinical trials, no overall differences in safety or effectiveness have been observed between patients over 65 years of age and younger patients treated with lanadelumab.
The effect of lanadelumab on fertility has not been evaluated in humans. Lanadelumab had no effect on male or female fertility in cynomolgus monkeys.
No dedicated drug–drug interaction studies have been conducted with lanadelumab. Based on its characteristics, no pharmacokinetic interactions with co-administered medicinal products are expected.
The most common side effects in patients receiving lanadelumab in clinical trials are described below.
At a dose of lanadelumab 300 mg every 2 weeks, the following adverse reactions where seen:
At a dose of lanadelumab 300 mg every 4 weeks, the following adverse reactions where seen:
Adverse reactions of 1–10% in incidence seen with lanadelumab include:
At a dose of lanadelumab 300 mg every 2 weeks, the following adverse reactions were seen:
At a dose of lanadelumab 300 mg every 4 weeks, the following adverse reactions where seen:
Treatment with lanadelumab has been associated with the development of anti-drug antibodies in 10 out of 84 patients (11.9%). All antibody titres were low. The anti-drug antibody response was transient in 20% of subjects positive for anti-drug antibodies; two out of 84 lanadelumab-treated patients (2.4%) tested positive for neutralising antibodies.
The development of anti-drug antibodies, including neutralising antibodies against lanadelumab, did not appear to adversely affect the pharmacokinetic and pharmacodynamic profiles or the clinical response.
Approved datasheets are the official source of information for medicines, including approved uses, doses, and safety information. Check the individual datasheet in your country for information about medicines.
We suggest you refer to your national drug approval agency such as the Australian Therapeutic Goods Administration (TGA), US Food and Drug Administration (FDA), UK Medicines and Healthcare products regulatory agency (MHRA) / emc, and NZ Medsafe, or a national or state-approved formulary eg, the New Zealand Formulary (NZF) and New Zealand Formulary for Children (NZFC) and the British National Formulary (BNF) and [British National Formulary for Children ](http://bnfc.nice.org.uk/ (BNFC).