Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Dr Alpana Mohta, Consultant Dermatologist, Sharda Multispeciality Clinic, India; Dr Libby Whittaker, DermNet Medical Writer, New Zealand (2023)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Obesity-associated lymphoedematous mucinosis (OALM) is a rare and recently identified form of pretibial dermal mucinosis that affects individuals who are obese. It displays clinical similarities to pretibial myxoedema but occurs in patients without thyroid dysfunction.
OALM has been previously referred to as chronic obesity lymphoedematous mucinosis.
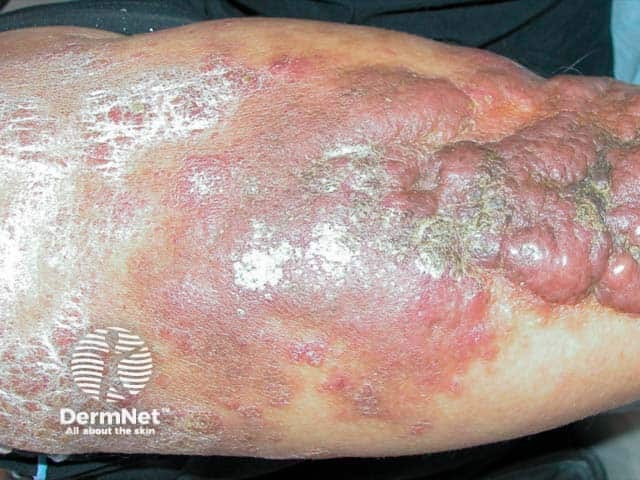
Florid plaques of obesity-associated lymphoedematous mucinosis on the shins (OALM-patient1)
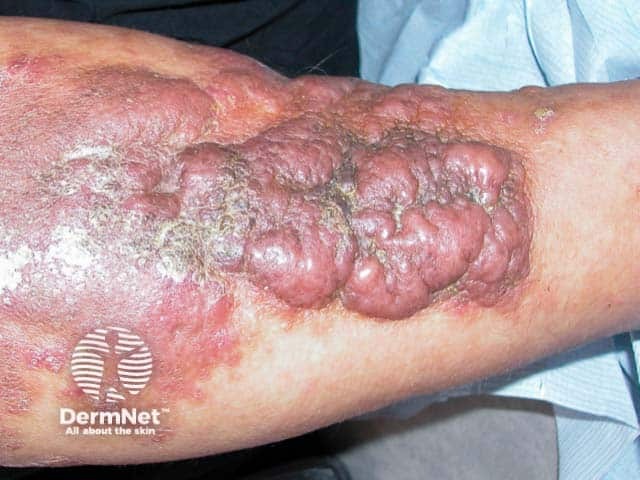
Florid plaques of obesity-associated lymphoedematous mucinosis on the shins (OALM-patient1)
See more obesity-associated lymphoedematous mucinosis images
OALM is strongly linked with obesity.
Euthyroid pretibial mucinosis, the spectrum of which includes OALM, may also be associated with venous insufficiency, lymphoedema, and trauma.
Cutaneous mucinoses involve aberrant deposition of mucin, sulfated glycosaminoglycans (GAG), and hyaluronic acid in the dermis.
The specific underlying pathomechanism of OALM is partially understood.
The clinical signs of OALM include asymptomatic papules and nodules that develop into plaques.
With time, lymphoedema develops in the lower limbs, usually bilateral and sparing the feet and ankles. In severe cases, vesicles may develop.
OALM may be seen in conjunction with stasis mucinosis, which is characterised by blue-violet, partially blanchable plaques and nodules with a smooth, pebbly texture. Often these patients also have other signs of chronic venous insufficiency like telangiectasia. It has been suggested that stasis mucinosis and OALM share a common aetiology, both representing the spectrum of euthyroid mucin depositional disease.
OALM mainly causes cosmetic concerns.
Chronic lymphoedema can predispose to venous eczema and skin infections, eg, cellulitis.
Clinical diagnosis: classical clinical features of dermal mucinosis with obesity.
Laboratory tests do not show hyperthyroidism.
Histochemical staining: for mucin, Alcian blue at pH 2.5 or colloidal iron staining is done; while dilated lymphatics can be visualised with D2-40 staining.
Although there is no universally accepted remedy, the primary approach revolves around weight loss. Hypocaloric diet (1200 calories/day) has been beneficial in multiple case series.
Pressure wraps and compression hosiery can help with lymphostasis and venous insufficiency. In instances of severe vascular deficiency, surgical treatment may be considered.
Other treatment options include:
Usually, the disease runs a benign course and the main concerns are cosmetic. Due to the heterogeneity of cases and the limited consensus on treatment, outcomes can vary. Weight reduction and venous compression strategies have been associated with clinical improvement.