Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2005; DermNet Update August 2021. Copy edited by Gus Mitchell.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Oral hairy leukoplakia is an Epstein-Barr virus infection of the tongue with a characteristic ‘corrugated or shaggy appearance’ seen most commonly in immunocompromised patients.
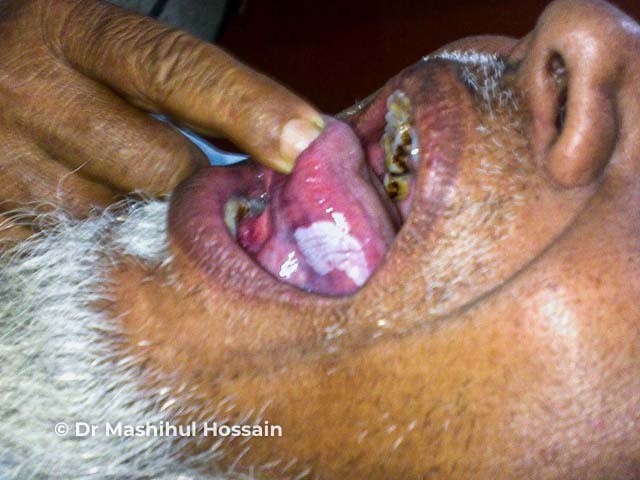
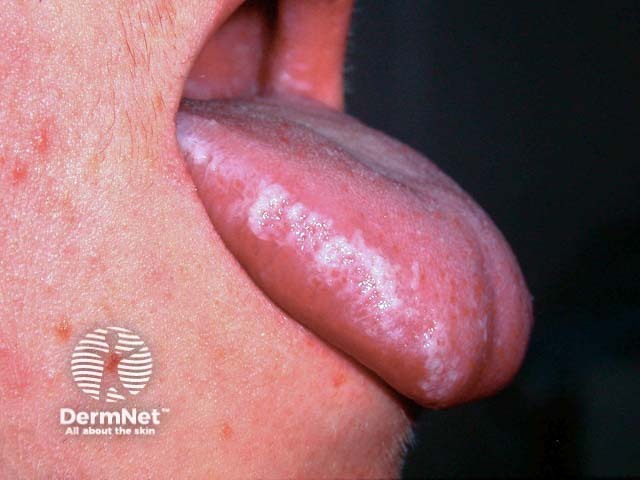
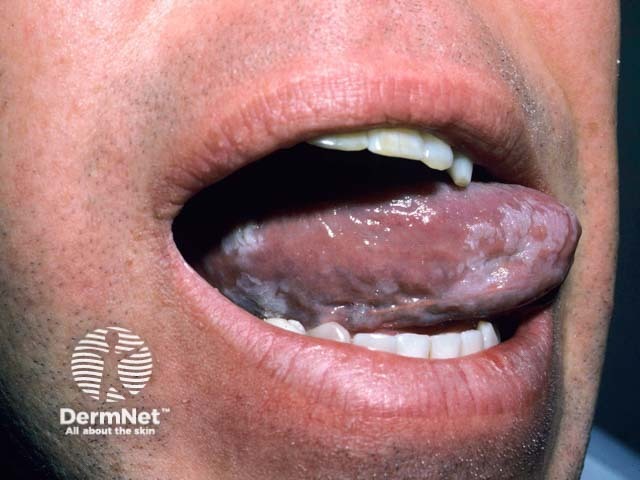
Oral hairy leukoplakia (OHL) was first described in HIV-positive homosexual men, and subsequently seen in all HIV-positive cohorts except for infants. OHL can be the initial indicator of HIV infection, or may suggest poor compliance with or failure of highly active antiretroviral therapy (HAART).
OHL can be seen with drug-induced immunosuppression such as required for organ and bone-marrow transplants, primary blood disorders, and with inhaled corticosteroids for asthma.
Oral hairy leukoplakia is also rarely described in immunocompetent patients. Recent case series report a white male predominance, and mean age at diagnosis of 50-60 years.
Oral hairy leukoplakia is caused by Epstein-Barr virus (EBV) infection of the tongue epithelium where there are few or no Langerhans cells. EBV delays apoptosis resulting in epithelial cell proliferation and hyperplasia. In OHL EBV is seen as intact virions and does not incorporate into the cell genome.
Oral hairy leukoplakia presents as asymptomatic white plaques on the lateral tongue which do not wipe off. It may be unilateral or bilateral. The appearance can range from faint white streaks to a furrowed corrugated surface. OHL is rarely also seen elsewhere in the oropharynx but not on other mucosal surfaces.
Discomfort, burning, or stinging may be reported by the patient.
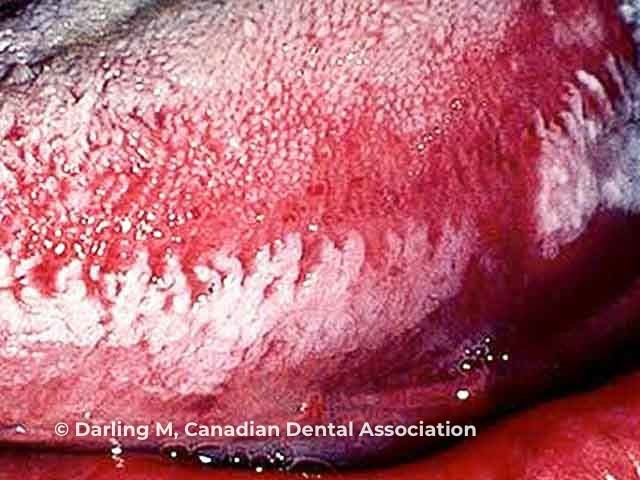
Figure 1
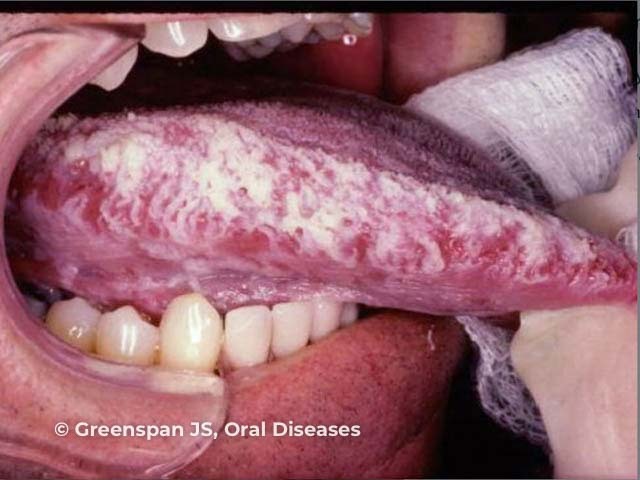
Figure 2
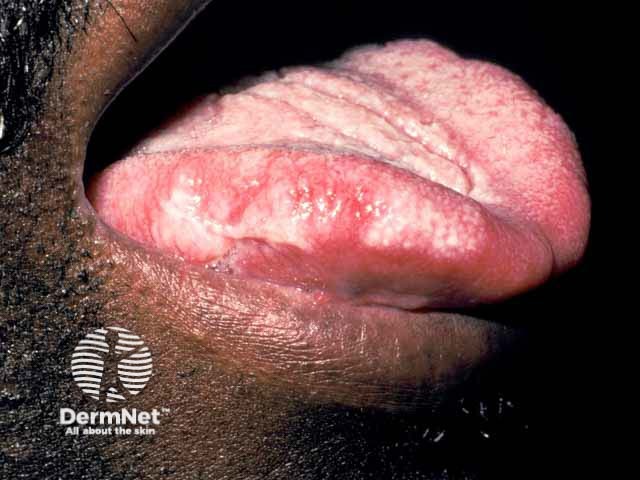
Figure 1 used with permission from: Darling MR, Alkhasawneh M, Mascarenhas W, Chirila A, Copete M. Oral hairy leukoplakia in patients with no evidence of immunosuppression: a case series and review of the literature. J Can Dent Assoc. 2018;84:i4. Image copyright Canadian Dental Association.
Figure 2 used with permission from: Greenspan JS, Greenspan D, Webster-Cyriaque J. Hairy leukoplakia; lessons learned: 30-plus years. Oral Dis. 2016;22 Suppl 1:120–7. Image copyright Prof D Greenspan.
Oral hairy leukoplakia may be suspected in an immunocompromised patient with the typical clinical features and no other cause for oral leukoplakia identified.
The diagnosis should be confirmed on biopsy and virologic studies such as immunohistochemistry, in-situ hybridisation, or electron microscopy [see Oral hairy leukoplakia pathology]. In-situ hybridisation for EBV DNA or RNA can also be performed on a surface scraping or smear.
Treatment is not usually required as oral hairy leukoplakia is asymptomatic and not premalignant.
Oral hairy leukoplakia is not cured by treatment. It may resolve spontaneously. OHL does not progress to oral cancer.