Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Freya Forstner, medical student, University of Auckland, New Zealand. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy Editor(s): Gus Mitchell, Maria McGivern. July 2017.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Podoconiosis is a form of lymphoedema that affects the lower limbs and occurs in people with long-term exposure to volcanic red clay soil.
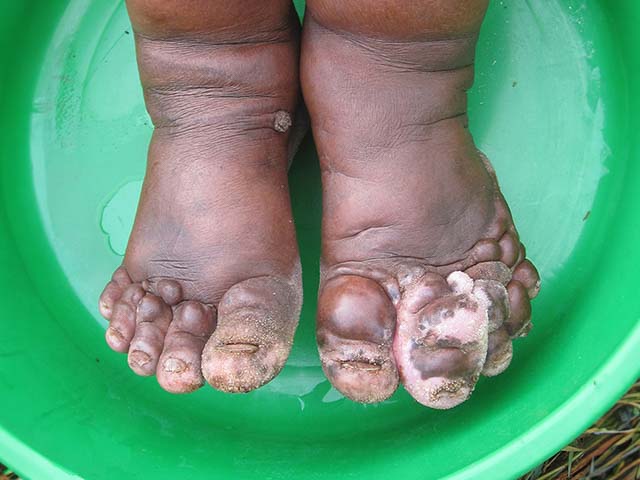
Fasil Ayele, National Institutes of Health, via Wikimedia Commons
Podoconiosis is endemic in tropical regions of Africa, Asia and Central America.
Podoconiosis is a genetically determined abnormal inflammatory reaction to mineral particles derived from volcanic deposits in red clay soils. The suggested pathogenesis is [1]:
No contagious or infectious organism has been identified.
Cutaneous symptoms and signs associated with podoconiosis include [1–3]:
Lichenification of the web space can be identified for using a lymphoedema test called Stemmer sign. This involves pinching and lifting on the skin on the upper surface of the second toe; if the skin is pinched but not lifted, the test is positive
Podoconiosis is a chronic condition that is commonly complicated by acute episodes of lymphadenitis, especially when fibrotic. Acute lymphadenitis presents as:
Podoconiosis presents with ascending lymphoedema.
Podoconiosis has an early prodromal phase prior to the development of elephantiasis.
Acute attacks resolve spontaneously after a few days of rest and elevation. Subsequent episodes typically affect the same limb. Patients have an acute attack on average five times a year [1,2].
The following staging system was designed for use by field workers [3]. Each leg should be staged separately for the:
The swelling is not present when the patient first gets up in the morning.
Complications of podoconiosis include:
Podoconiosis is diagnosed clinically. Diagnosis is based on clinical features, a careful patient history and the exclusion of other causes of lymphadenitis.
The differential diagnosis includes other causes for elephantiasis, such as:
Podoconiosis treatment aims to reduce lymphoedema and to prevent relapse by reducing re-exposure to the causative soil.
Primary prevention requires avoiding prolonged contact between the skin and the soil. This includes:
Treatment after podoconiosis has occurred involves:
More severe disease may require [1, 2]:
Surgical management has been attempted. Shave excision (using a blade to remove the top layers of the skin) of hard nodules has been used with secondary intention healing (where surgical wounds are left to heal by themselves). It should be noted that surgical removal of tissue followed by skin grafting (Charles operation) is unsuccessful, as scar tissue aggravates symptoms [1].
Podoconiosis results in progressive swelling and disfigurement of the limbs. Untreated patients are typically in constant pain and discomfort and may suffer from chronic infections. As a result of social stigmatism, individuals with podoconiosis are often ostracised in their communities [1, 2].