Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Primary cutaneous CD30+ lymphoproliferative disorders — extra information
Primary cutaneous CD30+ lymphoproliferative disorders
Authors: Dr Germana Consuegra Romero, Dermatologist, Hospital Universitari General de Catalunya, Barcelona, Spain; Prof Pablo Fernández-Peñas, Dermatologist, Westmead Hospital, Sydney, Australia; Dr Jillian Wells, Dermatologist, Westmead Hospital, Sydney, Australia. Copy edited by Gus Mitchell. May 2021
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
What are primary cutaneous CD30+ lymphoproliferative disorders?
Primary cutaneous CD30+ lymphoproliferative disorders (LPD) are indolent-behaving extranodal T-cell neoplasms localised to the skin and characterised by CD30 expression on atypical lymphocytes. Lymphoproliferative disorders account for about 10% of cutaneous lymphomas and 30% of cutaneous T-cell lymphomas (CTCL). CD30+ lymphoproliferative disorders are the second most common form of CTCL after mycosis fungoides.
Primary cutaneous CD30+ lymphoproliferative disorders are classified as:
- Lymphomatoid papulosis (LyP)
- Primary cutaneous anaplastic large-cell lymphoma (pcALCL)
- Borderline or indeterminate lesions where a distinction cannot be made between the above eg, a rapidly growing nodule in a patient with LyP.
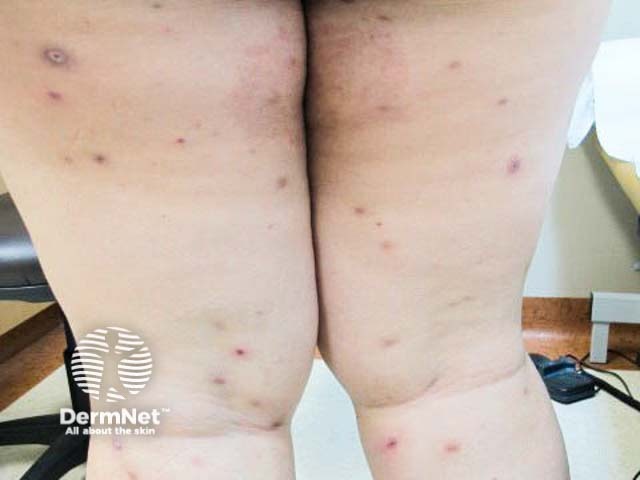
Lymphomatoid papulosis
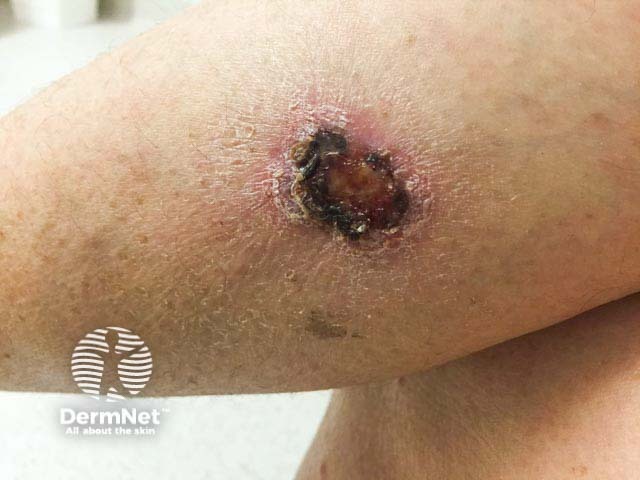
Primary cutaneous anaplastic large-cell lymphoma
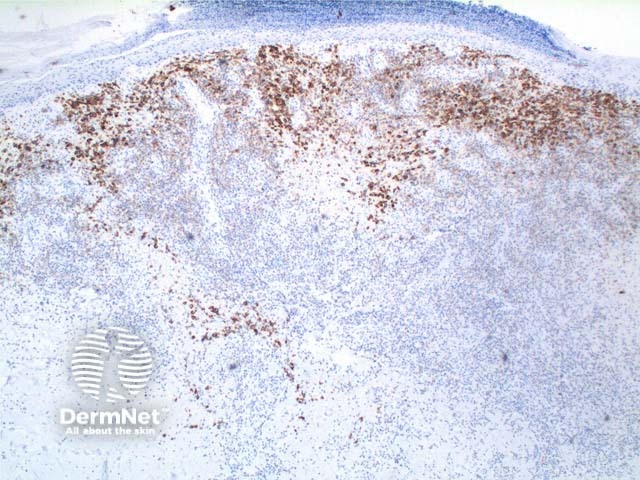
Immunohistochemistry: CD30 positive atypical T-cells in lymphomatoid papulosis
Who gets primary cutaneous CD30+ lymphoproliferative disorders?
Primary cutaneous CD30+ lymphoproliferative disorders are rare. They affect both sexes, all races, and all ages. However, there are some differences in the epidemiology of the various types:
- Lymphomatoid papulosis: male predominance, average age of onset 35–45 years, uncommon in skin of colour
- pcALCL: male predominance (3:1), median age of onset 60 years.
What causes primary cutaneous CD30+ lymphoproliferative disorders?
The aetiopathogenesis of primary cutaneous CD30+ lymphoproliferative disorders remains elusive. CD30 signalling is known to affect growth and survival of lymphoid cells. Some studies suggest restriction of the normal T-cell repertoire in the peripheral blood. Other hypotheses implicate reactive phenomena inducing CD30+ overexpression.
What are the clinical features of primary cutaneous CD30+ lymphoproliferative disorders?
Lymphomatoid papulosis (LyP)
- Recurring crops of papules that often ulcerate or become necrotic
- Papules heal spontaneously over 3–12 weeks to leave post-inflammatory hypo- and hyper-pigmentation and varioliform scars
- Waxing and waning course lasting months or years before remitting
Primary cutaneous anaplastic large-cell lymphoma (pcALCL)
- Rapidly growing solitary nodule or tumour that often ulcerates; less commonly multiple or generalised lesions
- Partial or total regression occurs in 20–40%
- Patient is systemically well
What are the complications of primary cutaneous CD30+ lymphoproliferative disorders?
- Scarring
- Extracutaneous spread — 10% of pcALCL spread to lymph nodes; visceral metastases are uncommon
- Association with other cutaneous and systemic lymphomas
- Impact on quality of life
How are primary cutaneous CD30+ lymphoproliferative disorders diagnosed?
Primary cutaneous CD30+ lymphoproliferative disorders require careful clinicopathological correlation to make the diagnosis. History, examination, and skin biopsy histopathology/immunohistochemistry must be compatible. Histopathology alone is not diagnostic as similar changes can be seen in other skin disorders.
What is the differential diagnosis for primary cutaneous CD30+ lymphoproliferative disorders?
- Lymphomatoid papulosis (LyP)
- Pityriasis lichenoides
- Reactive lymphoid hyperplasia secondary to insect bites, scabies, medications, infections
- pcALCL
- Primary cutaneous anaplastic large-cell lymphoma (pcALCL)
- Systemic anaplastic large-cell lymphoma
- Transformed mycosis fungoides
- Other systemic lymphomas with secondary cutaneous involvement
What is the treatment for primary cutaneous CD30+ lymphoproliferative disorders?
Lymphomatoid papulosis (LyP)
There are currently no treatments that change the natural history or cure LyP. Treatment is not always required if eruptions are infrequent, produce few lesions, and do not scar. Treatment may be considered to reduce the frequency and severity of crops or accelerate healing for frequent, extensive cropping or where there is an impact on quality of life, but needs to be weighed up against side effects.
Primary cutaneous anaplastic large-cell lymphoma (pcALCL)
- Excisional biopsy of solitary or few lesions
- Radiotherapy
- Methotrexate
Anti-CD30 medications such as brentuximab vedotin (anti-CD30 monoclonal antibody linked to monomethyl auristatin E) are being used increasingly in the treatment of primary cutaneous CD30+ lymphoproliferative disorders.
What is the outcome for primary cutaneous CD30+ lymphoproliferative disorders?
Primary cutaneous CD30+ lymphoproliferative disorders look malignant on histopathology but most follow an indolent clinical course. Five-year survival is estimated to be 100% for lymphomatoid papulosis and 95% for primary cutaneous anaplastic large-cell lymphoma. However, five-year survival of generalised pcALCL may be as low as 50%.
Long-term surveillance and follow-up is recommended as LyP can be associated with other cutaneous and systemic lymphomas in up to 20% of cases, and pcALCL can recur or spread beyond the skin.
Bibliography
- Cerroni L. Lymphoproliferative lesions of the skin. J Clin Pathol. 2006;59(8):813–26. doi:10.1136/jcp.2005.033019. PubMed Central
- Gilson D, Whittaker SJ, Child FJ, et al. British Association of Dermatologists and U.K. Cutaneous Lymphoma Group guidelines for the management of primary cutaneous lymphomas 2018. Br J Dermatol. 2019;180(3):496–526. doi:10.1111/bjd.17240. Journal
- Kartan S, Johnson WT, Sokol K, et al. The spectrum of CD30+ T cell lymphoproliferative disorders in the skin. Chin Clin Oncol. 2019;8(1):3. doi:10.21037/cco.2018.12.03. Journal
- Kempf W, Pfaltz K, Vermeer MH, et al. EORTC, ISCL, and USCLC consensus recommendations for the treatment of primary cutaneous CD30-positive lymphoproliferative disorders: lymphomatoid papulosis and primary cutaneous anaplastic large-cell lymphoma. Blood. 2011;118(15):4024-35. doi:10.1182/blood-2011-05-351346. Journal
- Sauder MB, O'Malley JT, LeBoeuf NR. CD30+ Lymphoproliferative disorders of the skin. Hematol Oncol Clin North Am. 2017;31(2):317–34. doi:10.1016/j.hoc.2016.11.006. PubMed Central
- Shinohara MM, Shustov A. How I treat primary cutaneous CD30+ lymphoproliferative disorders. Blood. 2019;134(6):515–24. doi:10.1182/blood.2019000785. Journal
- Willemze R, Cerroni L, Kempf W, et al. The 2018 update of the WHO-EORTC classification for primary cutaneous lymphomas. Blood. 2019;133(16):1703–14. doi:10.1182/blood-2018-11-881268. Journal
On DermNet
- Cutaneous T-cell lymphoma
- Lymphoma
- Lymphomatoid papulosis
- Lymphomatoid papulosis pathology
- Primary cutaneous anaplastic large-cell lymphoma
Other websites
- Lymphomatoid Papulosis — Cutaneous Lymphoma Foundation
- Lymphomatoid Papulosis — The Australasian College of Dermatologists
- Lymphomatoid Papulosis — JAMA Dermatology
- Lymphomatoid Papulosis — Medscape
- Lymphomatoid Papulosis — Genetic and Rare Diseases Information Center (GARD)
