Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer; Copy Editor: Clare Morrison; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, October 2013. About Melanoma is sponsored by the New Zealand Dermatological Society Incorporated.
If you find a suspicious looking mole or you’re just not sure about a spot you find on your body, go and see your doctor. This could save your life!
Your doctor is trained to identify suspect moles or spots as potentially melanoma. At your visit be prepared for some or all of the following things:
A good light, magnification and photography help identify melanoma




For most people self skin-checks done every 1–3 months is all that is needed to pick up early signs of skin cancer and melanoma.
However, a detection programme may be useful for those at high risk of melanoma. The term ‘mole mapping’ has been used in several different ways but usually refers to a monitoring programme where:
The mole mapping process is sometimes called teledermatoscopy or digital dermatoscopic surveillance. It is most suitable for people with many moles, especially if they have atypical moles.
The outcome of your first mole map will determine when you have your next one. A follow-up visit in 3 to 6 months may be needed to photograph a mole that is borderline to ensure it is stable.
Otherwise you may have a follow-up mole map every one to two years or at such a time as recommended by your doctor.
A less technical mole mapping procedure is your doctor simply marking spots on a cartoon drawing of a body to indicate the position of moles and spots that might be of concern. Your doctor may examine your moles using a dermatoscope and take photographs for future reference.
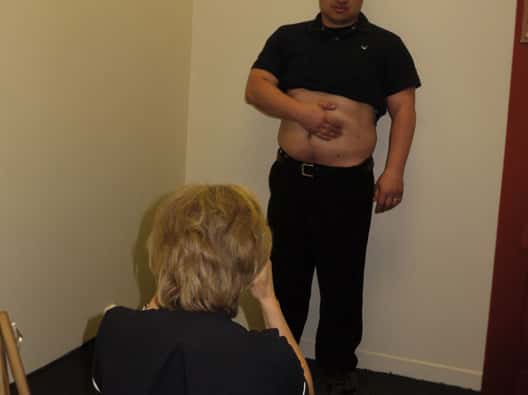
Taking body shots
A mole that's been mapped
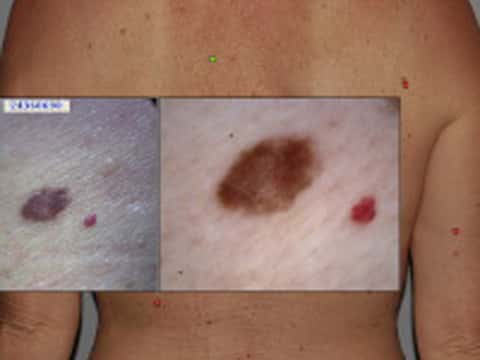
Body shots
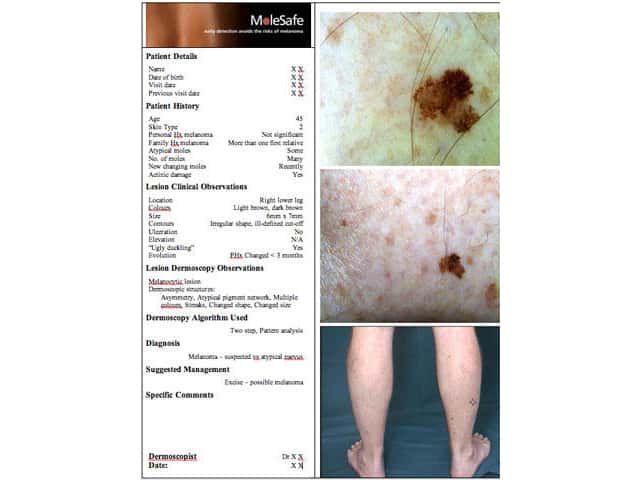
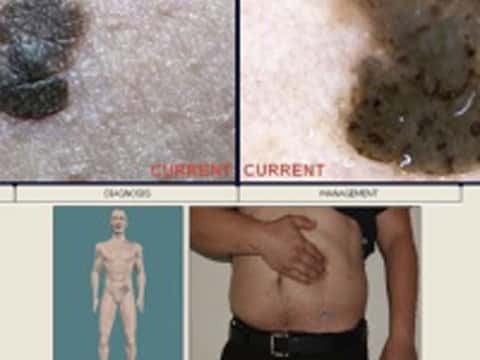
Report for patient and doctor
*Images supplied by MoleMap NZ
If you have a suspected skin cancer, including melanoma, your doctor may arrange to remove it surgically at your usual medical centre.
If your doctor is unsure of the diagnosis, or if your suspicious mole needs the attention of an expert, you may be referred to a specialist. Skin cancer specialists include dermatologists, plastic surgeons and other highly trained doctors.
Previous: Check your skin. Next: Do I have melanoma?
The value of dermatoscopy in the diagnosis of melanoma video (Ken Ip).