Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Diana Purvis, Paediatric Dermatologist, Auckland, New Zealand, 2011.
Toxic erythema of the newborn (also known as erythema toxicum and erythema toxicum neonatorum) is a common and benign condition seen in newborn infants. It affects as many as half of all full-term newborn infants but is less common in infants born prematurely. There is no known sex or racial predilection, although it has been suggested that it may be under-recognised in infants with darker skin types.
Most cases of toxic erythema of the newborn begin in the first few days after birth, although onset can be as late as two weeks of age.
Toxic erythema of the newborn is evident as various combinations of erythematous macules (flat red patches) papules (small bumps) and pustules. The eruption typically waxes and wanes over several days and it is unusual for an individual lesion to persist for more than a day.
Toxic erythema of the newborn often begins on the face and spreads to affect the trunk and limbs. Palms and soles are not usually affected.
The infant is otherwise well.
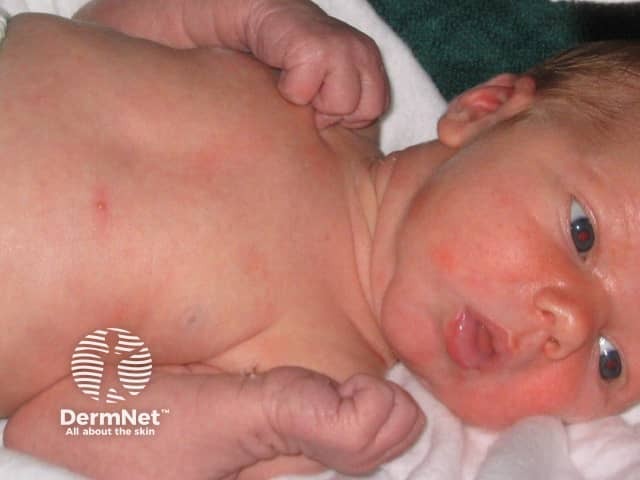
Toxic erythema of the newborn
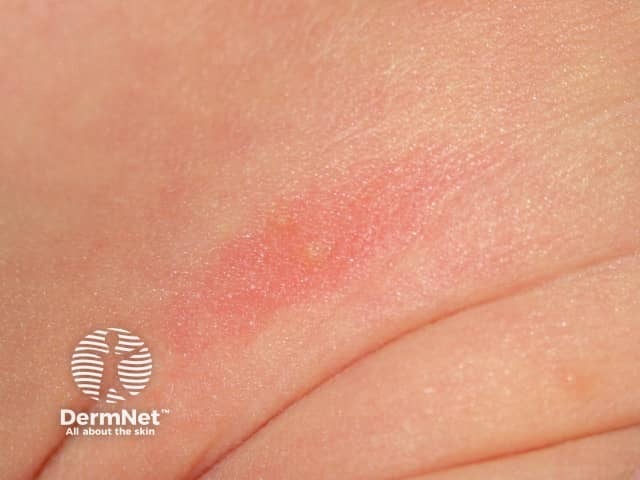
Toxic erythema of the newborn
The diagnosis of toxic erythema of the newborn is usually made on clinical grounds. Histology from skin biopsy samples taken from flat patches shows a diffuse infiltrate of eosinophils and neutrophils (inflammatory cells) in the upper dermis; from papules shows an eosinophilic infiltration around the hair follicle, and from pustular lesions shows perifollicular subcorneal pustules filled predominantly with eosinophils.
How toxic erythema of the newborn arises is unknown. A number of theories have been proposed including that it is a reaction to mechanical and thermal (heat) stimuli, an ‘allergic’ reaction or a mild form of graft vs host disease.
Although toxic erythema of the newborn is benign and requires no treatment, a number of differential diagnoses should be considered. These include:
These usually are recognised by clinical features, although in some cases the diagnosis may be helped by Tzanck smears or skin biopsy.