Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Causes
Signs and symptoms
Investigations
Treatment
Variegate porphyria is a subtype of porphyria. It is an inherited disorder characterised by skin photosensitivity (reaction to light), systemic symptoms arising from neurological problems, or both. It is considered very uncommon or rare throughout the world apart from in South Africa, where it is estimated that 1 in 300 of South Africa's white population is affected. This gene mutation is traceable to Dutch immigrants who married there in 1680.
Variegate porphyria is caused by a gene mutation of the protoporphyrinogen oxidase enzyme protein (PPOX). This enzyme is critical in the chemical process that leads to haem production. Haem is the red pigment in blood cells and is an important component of haemoglobin, the molecule that carries oxygen in the blood. In people with variegate porphyria activity of the PPOX enzyme is reduced by 50%. This means there is as build-up of toxic porphyrins particularly uroporphyrin and coproprophyrin, which leads to blistering.
Variegate porphyria is an autosomal dominant disorder. This means that a male or female carrying the gene will pass it on to half of his or her children.
In most people with variegate porphyria signs and symptoms may only become apparent when they are exposed to non-genetic factors such as certain drugs, stress, dieting or fasting, and certain hormones. These factors increase the demand for haem and the enzymes to make haem. The combinations of increased demand and reduced activity of PPOX disrupts haem production and triggers an acute variegate porphyria attack.
Approximately 60% of patients with a PPOX gene mutation will experience no symptoms. In those that are symptomatic, skin photosensitivity occurs 3-5 times more often than systemic symptoms arising from neurological dysfunction. In a few cases, both skin and systemic symptoms occur together. In most cases acute attacks usually begin in adulthood and can often be linked to history of a new medication.
Signs and symptoms of variegate porphyria rarely occur in childhood, however in cases where it does occur it is usually more severe and even debilitating. Children with this condition may have intellectual disability and grow more slowly.
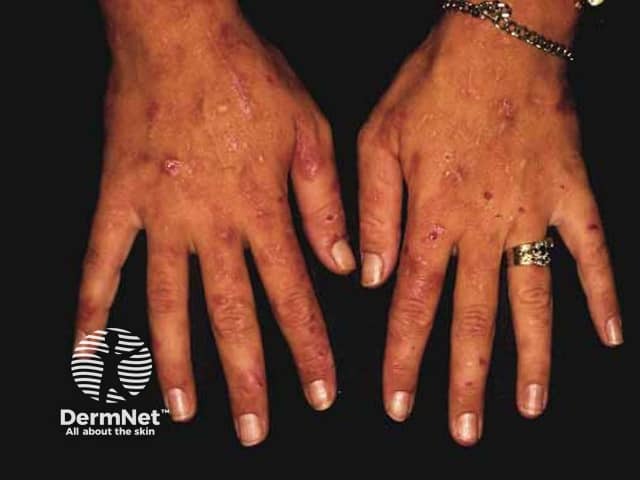
Variegate porphyria
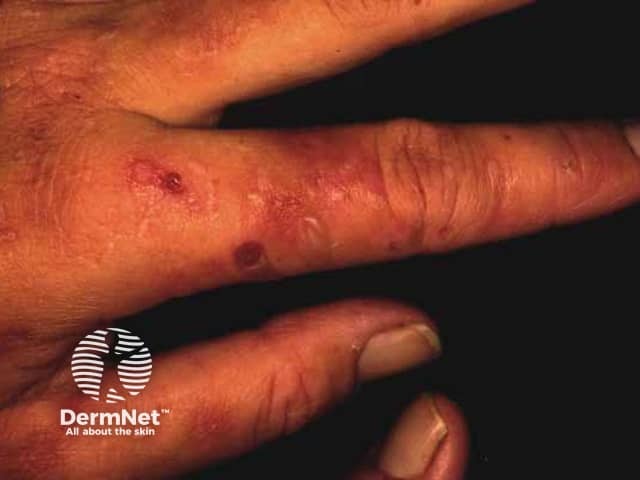
Variegate porphyria
Most people with variegate porphyria have skin that is overly sensitive to sunlight. Areas exposed to the sun often develop blistering, scarring, changes in skin colour and increased hair growth.
Acute attacks cause severe abdominal pain, uncontrolled vomiting, diarrhoea and constipation. Neurological manifestations include muscle and limb weakness that may progress to areflexic quadriparesis (weak arms and legs), seizures, and mental changes such as anxiety and hallucinations. Other symptoms include changes in heart rate and blood pressure, and respiratory distress. Electrolyte imbalance such as low sodium and magnesium levels may be present.
During acute attacks, the diagnosis of variegate porphyria is confirmed by:
These tests should be done by an experienced and quality-assured laboratory as precision is critical.
There is a rapid test kit to identify elevated porphobilinogen if required in an emergency.
The features of a skin biopsy may appear similar to porphyria cutanea tarda. The blister is due to clefting under the epidermis and is not associated with much inflammation. Blood vessel walls and basement membranes are thickened.
Other tests will depend on the general health of the individual and symptoms.
The management of an acute attack of variegate porphyria is the same as for acute attacks of all other porphyria disorders. Management of acute attacks consists of the following:
Patients with variegate porphyria must be informed about the factors that can trigger the acute symptoms of the condition. Whilst most triggers of variegate porphyria appear to be drugs, in some cases the inducing factor is unknown. Hence it is sensible to minimize exposure to risk factors. Patients should adhere to the following management points as much as possible.
It can be difficult to determine which drugs should be avoided by people with variegate porphyria, and tolerance of these can vary between patients. Mimimise drug use and refer to a list of safe and unsafe drugs (see links to other websites below).
An investigational drug, givosiran, is an RNAi therapeutic targeting aminolevulinic acid synthase 1 and is showing promise in the management of variegate porphyria.