Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Drug eruptions are common – think carefully before you prescribe an unnecessary medicine! In hospital patients, rashes are commonly attributed to and often caused by medications. Clinical manifestations are very variable.
About 3% of patients admitted to hospital have rashes due to adverse drug reactions but in others the cutaneous signs are due to the underlying or intercurrent illness (e.g. viral or bacterial exanthemas or internal disease), non-specific reactions to treatment (e.g. sweat-rash due to prolonged bed rest with plastic sheeting) or independent skin disease that has not been recognised by hospital staff. True drug reactions may mimic other skin diseases. In general, the rash improves when the drug is withdrawn. This may occur quickly but in some cases takes weeks or longer.
Adverse drug eruptions can be dangerous, especially toxic epidermal necrolysis (TEN) and drug hypersensitivity syndrome.
Features indicating a potentially serious reaction include:
| Immunological hypersensitivities |
|---|
These represent true allergic reactions.
|
| Non-immunological drug eruptions |
These may be due to idiosyncratic reaction, hereditary enzyme deficiency, dose dependent cumulation, irritancy or toxicity. Examples include:
|
The patient may need to be coaxed to report their drug history. Although adverse reactions are less likely to arise from drugs that the patient has been on for a long period of time, this is not always the case. Suggest these are brought to the clinic for inspection.
Ask about all medications taken in the last three months:
It is not possible to memorise all possible causes of all possible drug eruptions. Standard reference handbooks such as the MIMS and manufacturers' data sheets include rash in the list of potential adverse effects for nearly every drug.
These are often also described as toxic erythema. Features include:
The suspected drug or drugs should be discontinued, and the rash usually subsides within a week. Unfortunately there are no useful in vitro or in vivo tests to confirm hypersensitivity reactions and re-challenge is not recommended (although it sometimes occurs inadvertently at a later date). May cross-react with other drugs in the same class. Sometimes the rash clears despite continuing the responsible drug or re-challenge is tolerated without adverse reaction.
Penicillin-induced rash Leukaemia (ampicillin) 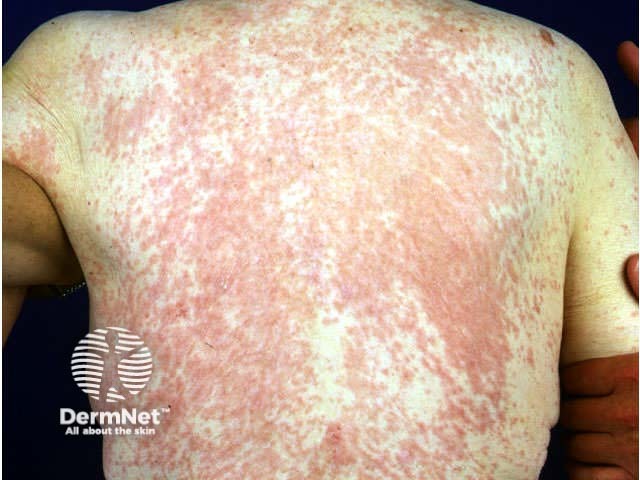
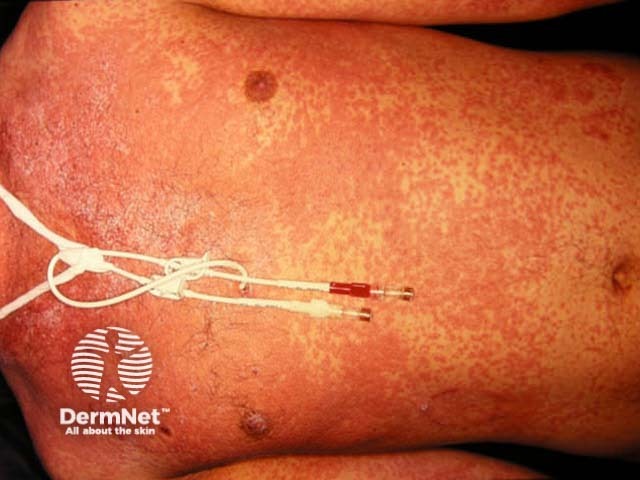
| Drugs that cause exanthematous rashes in >1% |
|---|
|
A morbilliform eruption in association with internal organ involvement and fever indicates possible drug hypersensitivity syndrome (DHS). This has a mortality rate of about 10%.
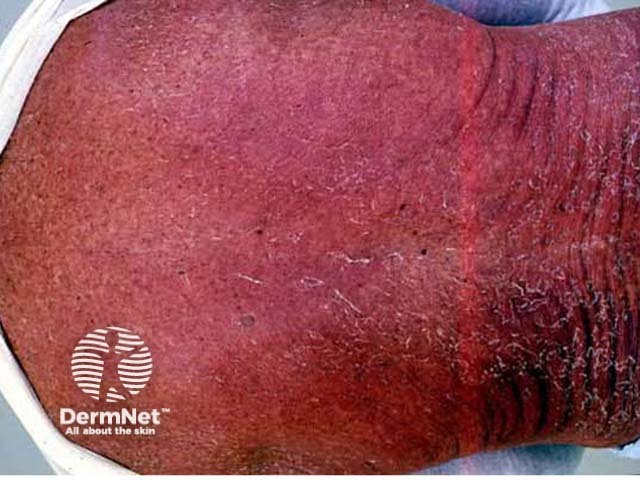
DHS due to allopurinol
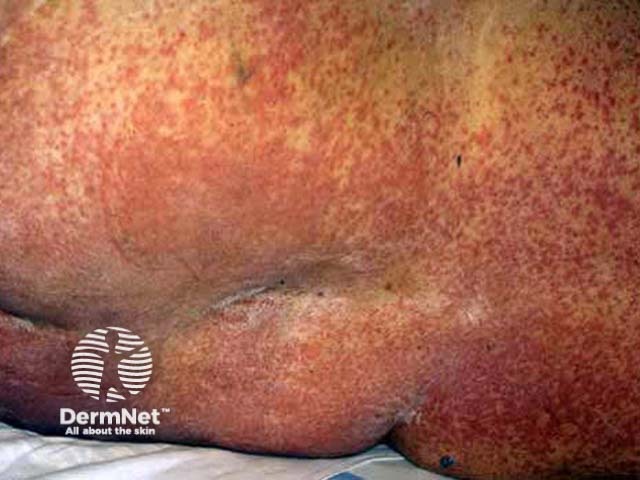
Severe reaction to penicillin
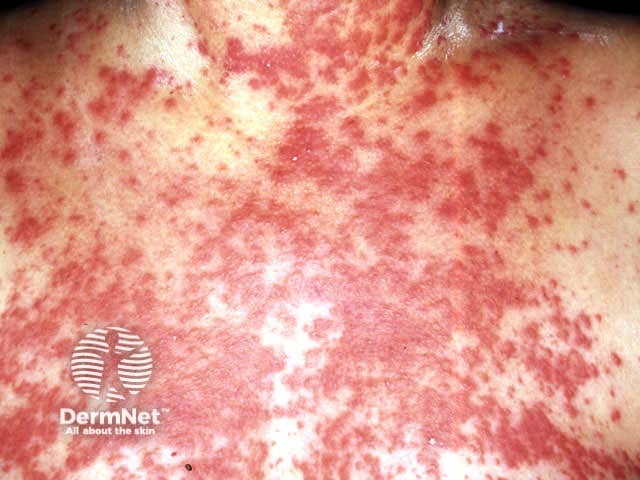
Papular eruption (hydroxychloroquine)
Drug-induced urticaria may occur with or without angioedema. It arises up to three weeks after first exposure (or minutes on re-challenge). It may be due to type 1 hypersensitivity (e.g. penicillin), sometimes in association with anaphylaxis and constitutional symptoms (respiratory distress, vascular collapse and shock).
It may also be due to direct release of inflammatory mediators from mast cells on first exposure to the drug (e.g. opiates, aspirin, NSAID, muscle relaxants).
ACE inhibitors such as captopril and enalapril may cause recurrent angioedema without urticaria, rarely commencing months or years after the drug was first prescribed.
Serum sickness is combination of urticaria, fever and arthralgia (sometimes lymphadenopathy, nephritis, endocarditis) and may be due to antibiotics especially cefaclor.
| Drugs that cause urticaria in >1% |
|---|
|
Fixed drug eruption (FDE) refers to solitary or multiple oval plaques that arise over a few hours and may have central blisters. It frequently affects mucosal surfaces such as the genitals and lips. FDE resolves in a few days leaving purplish hyperpigmentation, then re-erupts in the same site on re-exposure to the causative drug, which is usually a medication taken intermittently such as paracetamol or antibiotics but may also be a food dye.
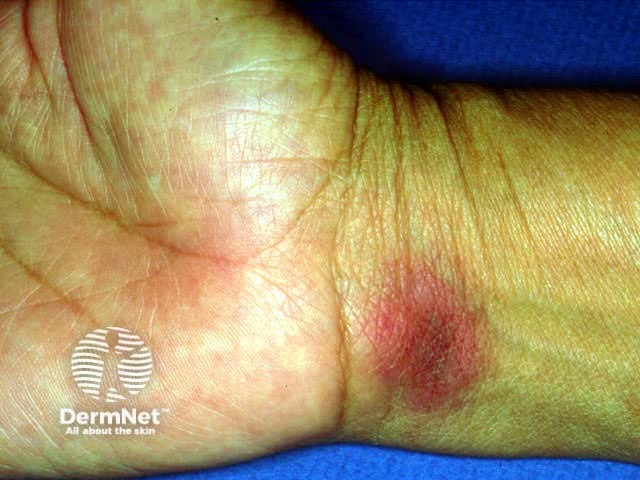
FDE due to tetracycline
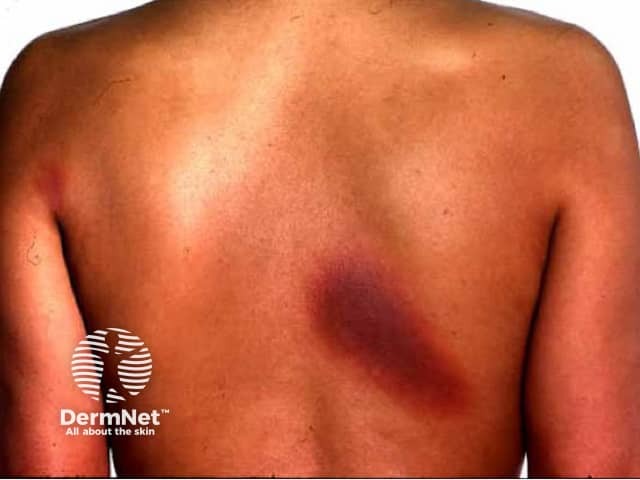
FDE due to cotrimoxazole
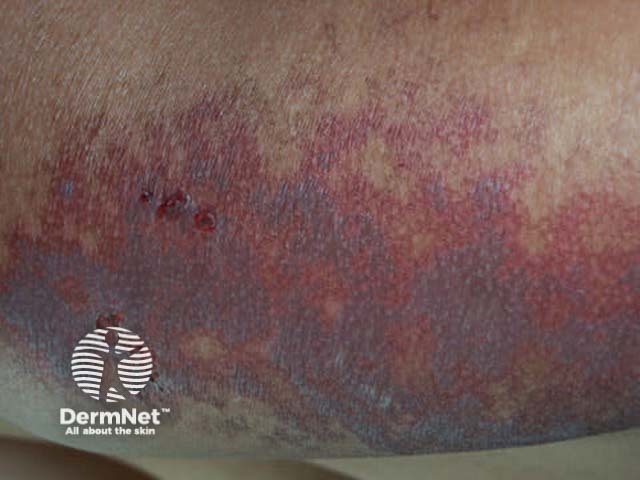
Purpuric FDE
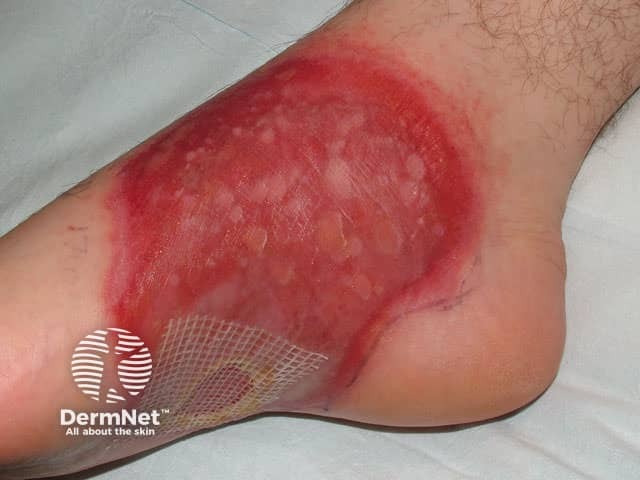
Fixed drug eruption
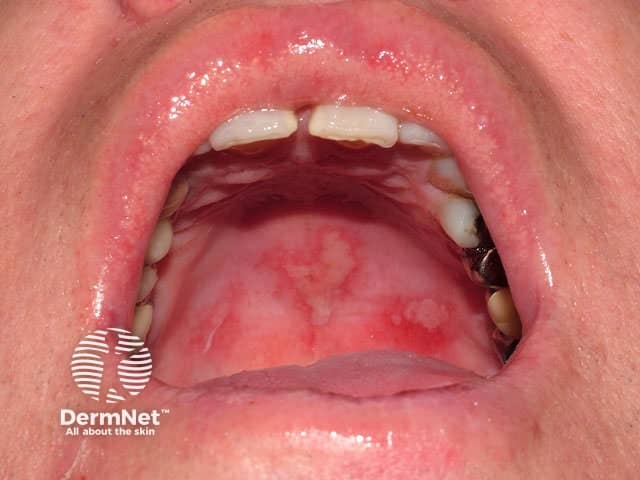
Fixed drug eruption

Fixed drug eruption
Drug-related bleeding into the skin includes:
Photosensitivity may be due to toxic or immunological mechanisms or both, from systemic or topical exposure to the medication. The rash affects sites of light exposure (UVA), but may spare habitually exposed areas such as the face and hands. Phototoxic reactions will affect everyone if the dose is high enough, and appears like sunburn (e.g. doxycycline, chlorpromazine). Photoallergic eruptions are generally eczematous or lichenoid (e.g. quinine).
Onycholysis may be due to drug-induced photosensitivity.
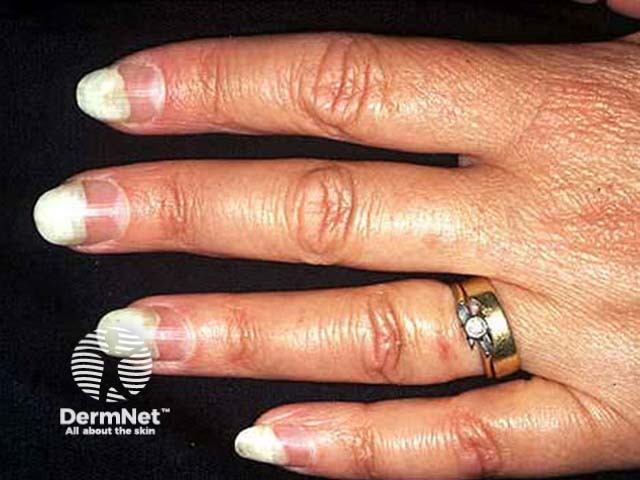
Photo-onycholysis (doxycycline)
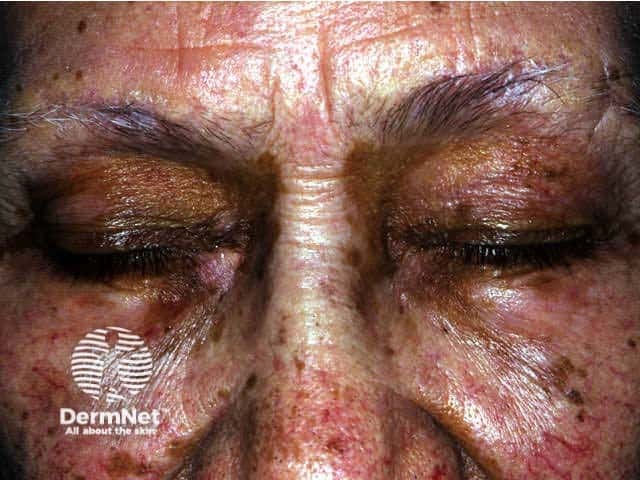
Postinflammatory hypopigmentation (quinine)
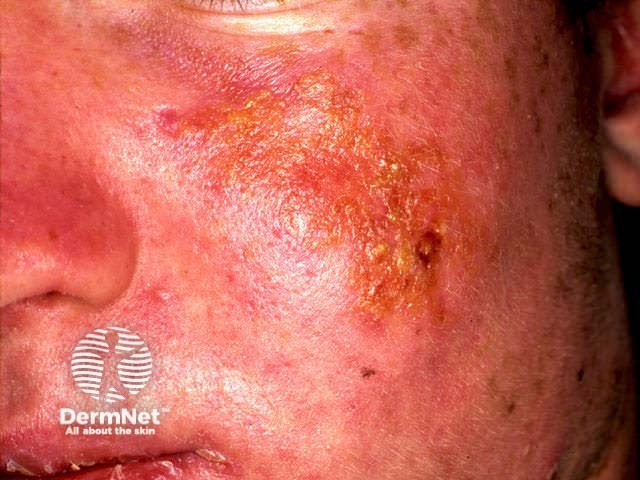
Severe sunburn (isotretinoin)
Several drugs may slowly induce hyperpigmentation of the skin and mucosal surfaces, due to the deposition of melanin (e.g. ACTH, oestrogen/progesterone, phenytoin), haemosiderin (minocycline), exogenous pigment (minocycline) or unknown mechanisms,
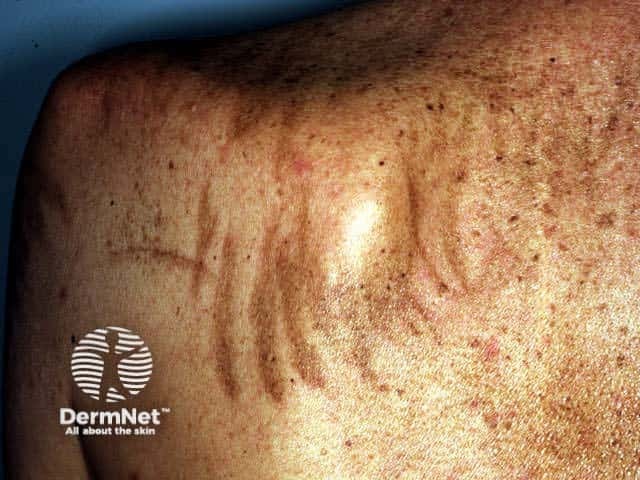
Flagellate pigmentation (bleomycin)
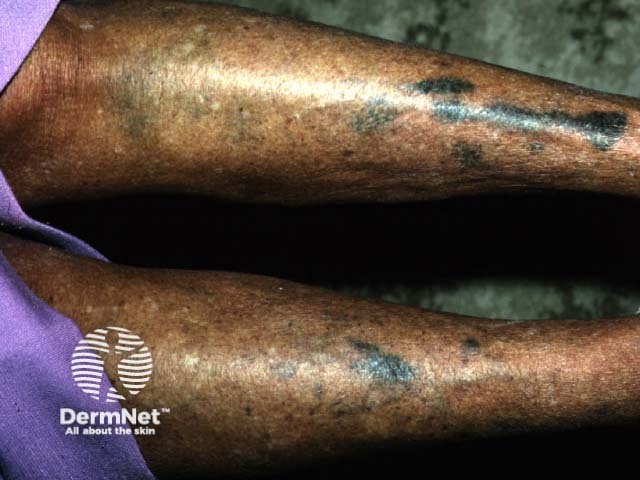
Blue-black pigmentation (minocycline)
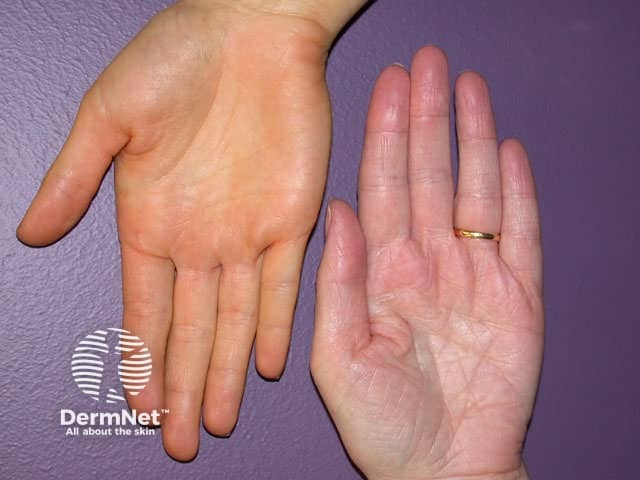
Carotenaemia (normal palm for comparison)
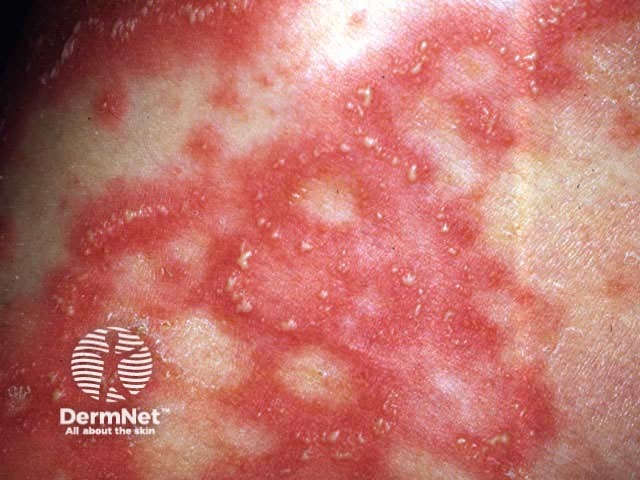
Pustuloderma (amoxicillin)
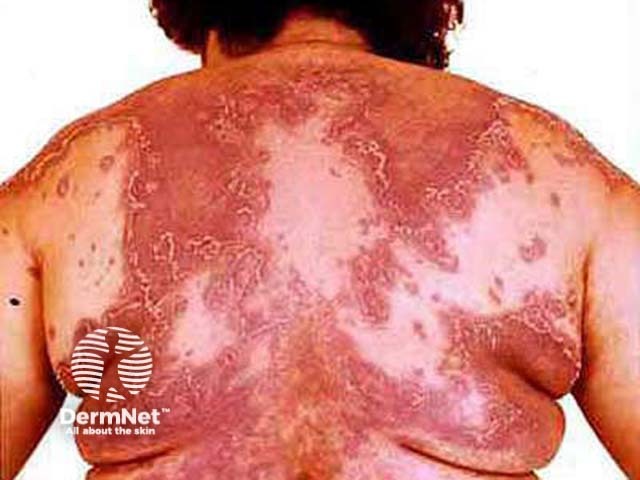
Pustular psoriasis (systemic steroids)
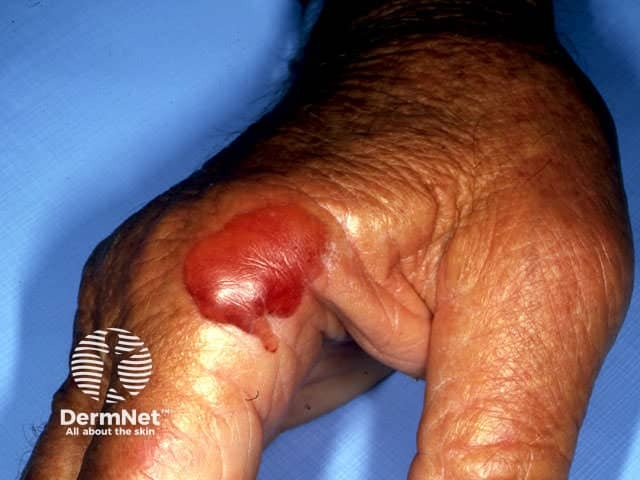
Pseudoporphyria (frusemide)
Adverse reactions to drugs are recognised by being suspicious of them; tests are rarely helpful. However eosinophilia in blood or tissue may be supportive.
Drugs can produce almost any histologic pattern and may appear identical to non-drug induced disorders.
If suspicious of a drug eruption, stop the responsible drug and avoid new ones (especially in the same pharmacological class).
Treat the patient:
Describe the presentation and management of Drug Hypersensitivity Syndrome
Information for patients
See the DermNet bookstore.