Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Emily Ryder, Specialist Registrar, Department of Dermatology, Oxford University Hospitals NHS Trust, Oxford, UK. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern. May 2017.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment
Acute localised exanthematous pustulosis (ALEP) is the localised form of acute generalised exanthematous pustulosis (AGEP). It can also be referred to as localised pustular drug eruption or localised toxic pustuloderma. ALEP is a rare form of drug reaction. It may occur a few days after starting a medication and usually resolves within a week of discontinuing the medication that triggered it.
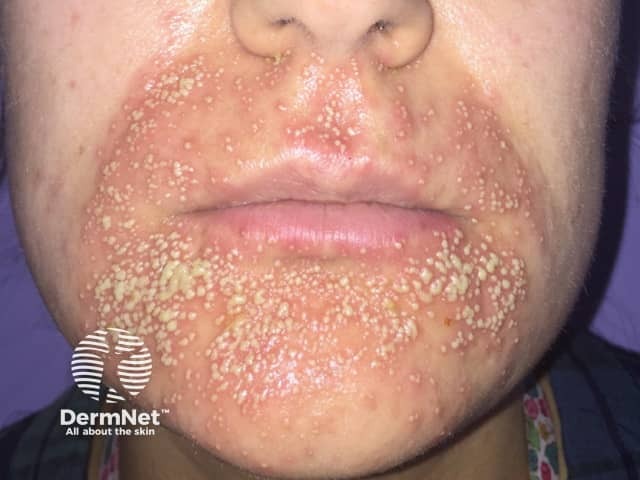
Acute localised exanthematous pustulosis
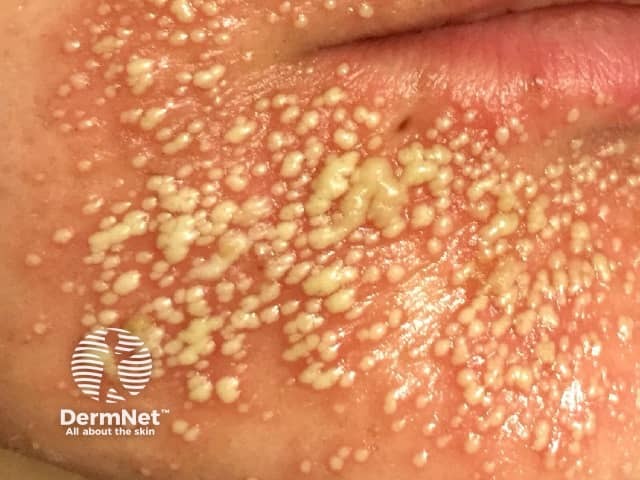
Acute localised exanthematous pustulosis
Acute localised exanthematous pustulosis is very rare and has only been reported in a small number of patients. It has been suggested that younger female patients may be more at risk of developing ALEP, but there is currently not enough information available to confirm this.
Acute localised exanthematous pustulosis may be triggered by various medications. Antibiotics containing amoxicillin seem to be most commonly associated with ALEP. It has also been reported from other antibiotics, non-steroidal anti-inflammatory drugs, antifungal agents, calcium antagonists, antiulcer drugs and pembrolizumab.
Acute localised exanthematous pustulosis has a sudden onset, presenting as localised clustered white or yellow pustules on the surface of a patch of red swollen (oedematous) skin, usually on the face. The pustules are usually superficial and flaccid and have an appearance similar to a localised area of AGEP.
Patients with ALEP usually describe the rash as feeling tight or uncomfortable but the rash is not usually particularly itchy. Some patients with ALEP report feeling tired or unwell; mild fevers have been reported in a small number of patients.
Acute localised exanthematous pustulosis may lead to post-inflammatory pigmentation in the affected area. It is not known whether ALEP may lead to severe adverse reactions to drugs.
A dermatologist may make the diagnosis of ALEP by recognising the appearance of the rash and the timeframe of its development in relation to a medication, such as an antibiotic. Usually the patient has taken the same medication previously without an adverse response.
The resolution of the rash within days of discontinuing the trigger medication can help to confirm the diagnosis.
The removal of the trigger medication usually leads to rapid improvement of the rash. Moisturisers (emollients) may help to sooth the skin but no specific treatment is required.
The skin may heal with residual pigment changes (postinflammatory hyperpigmentation or postinflammatory hypopigmentation) that usually improves after months to years.
Once the ALEP diagnosis is confirmed, the patient should be advised to avoid further use of the trigger medication.