Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
UVB phototherapy
Created 2007.
Learning objectives
- Describe a fluorescent low-pressure mercury type of UVB phototherapy unit
- Describe the mechanism of action of UVB on skin diseases
- List safety measures for UVB phototherapy
- Describe how to measure minimal erythema dose
- Describe dose regimens for BB-UVB and for NB-UVB
- List complications of UVB treatment
UVB
Ultraviolet-B (UVB) is the name given to the waveband of electromagnetic radiation ranging from 290 to 320 nm. Solar UVB is responsible for the majority of sunburn and is the main cause of sun damage and skin cancer. It is greatest at solar noon (1.30 pm in summer in New Zealand), at shorter latitudes, higher altitude and on clear days. It is blocked by window glass.
UVB phototherapy is effective in clearing or controlling a variety of skin diseases. It is available at the larger public hospitals and some private dermatologists' offices in New Zealand. Phototherapists are most often registered nurses but may also be physiotherapists or unqualified staff under the supervision of a dermatologist.
Phototherapy units in New Zealand are full-body cabinets containing 6-foot long, 100W fluorescent low-pressure mercury bulbs. Broadband UVB lamps have red identification markings (eg, FS72T12UVBHO) and narrowband lamps have brown markings. Older units supply broadband UVB (BB-UVB) with TL100/12 lamps, but increasingly these are being converted to or replaced by narrowband sources (NB-UVB) with TL100/01 lamps, often with 48 or 56 bulbs in the cabinet. Original 4-bulb Theraktin units are being phased out but may still be in use.
Modern units have integrated dosimetry and the time to deliver the correct dose is automatically calculated. For older units, irradiance is checked manually prior to treatment using a specific UVB dosimeter and the treatment time for a specific dose determined according to a spreadsheet.
Phototherapy units
Bulb markings Photherapy 



Indications for UVB
Psoriasis is the most common skin disease treated with UVB. NB-UVB phototherapy clears about 75% of patients, where clearance is defined as 90% or greater reduction in the extent of psoriasis compared to baseline. The number of treatments required ranges from 10 to 40, delivered two to five times weekly. BB-UVB clears a smaller proportion and a greater number of treatments may be required.
UVB is most likely to be successful with acute guttate and thin plaque psoriasis, especially if there is a history of improvement on exposure to sunlight. It is less likely to be successful with very thick plaques, especially if there is a dense surface scale.
Effect of UVB phototherapy on psoriasis
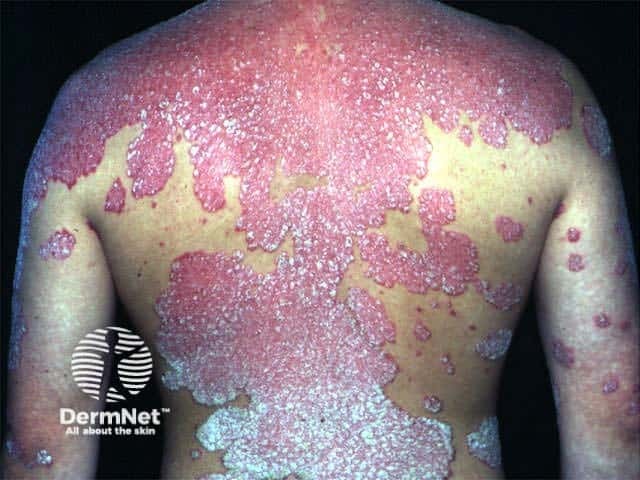
Extensive psoriasis prior to NB-UVB
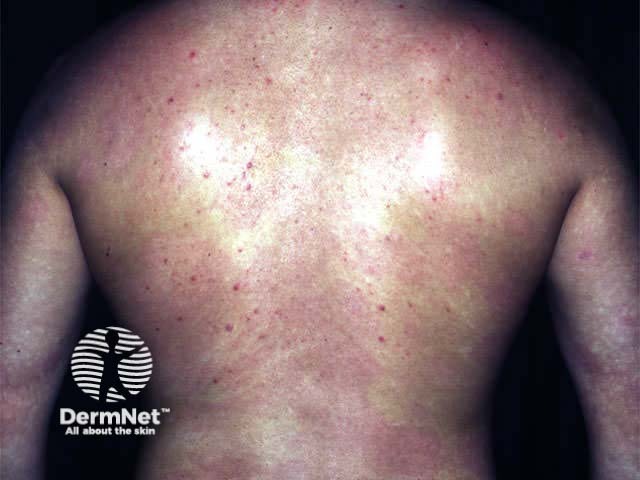
Psoriasis has cleared after 22 treatments
An increasing range of skin diseases is reported to clear or improve with NB-UVB but these respond less predictably and may require a greater number of treatments.
Mechanism of action
The mechanism of action of UVB on various skin diseases but is probably related to the suppression of major components of cell-mediated immune function.
- UVB radiation is absorbed by DNA and urocanic acid.
- It alters antigen-presenting cell activity.
- In psoriasis, it lowers peripheral natural killer cell activity, lymphocyte proliferation and immunoregulatory cytokine production by Th1 (IL-2, IFN-alpha) and Th2 (IL-10) T-cell populations.
UVB results in erythema, which begins 2–6 hours after exposure, peaks at 12–18 hours after exposure and generally persists for 48 hours.
Patient safety
Patient safety is paramount as overdose can result in severe and potentially life-threatening burns.
- Staff should be properly trained and supervised.
- There should be good indications for treatment and no contraindications
- Patients should receive comprehensive information and sign a consent form for treatment.
- Patients should be compliant with instructions and schedules.
- Equipment should be appropriately designed, regularly maintained and calibrated.
- Protect eyes with UV-blocking goggles.
- Face, genitalia and radiation-damaged skin should be shielded unless involved with significant disease.
- Trained personnel must be present throughout treatment and able to communicate with the patient.
- Additional sun exposure should be minimised.
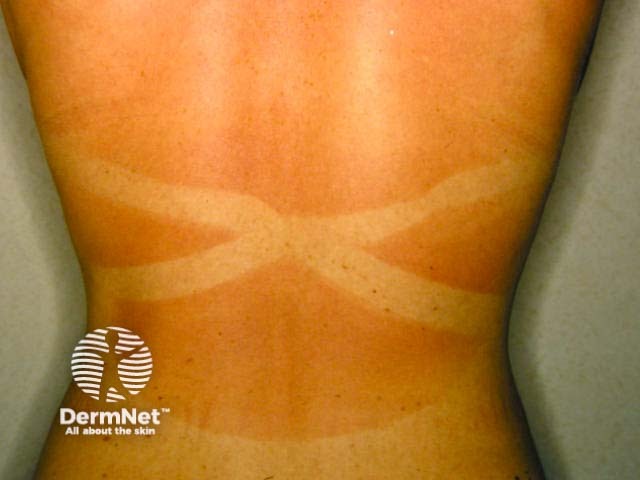

Minimal erythema dose
Individual skin response to UVB depends on skin phototype, prior exposure to sunlight or another source of UV and the presence of photosensitivity. Skin phototypes are determined by carefully questioning the patient but may be assigned incorrectly.
For BB-UVB therapy it is useful to measure Minimal Erythema Dose (MED) in skin types 1 to 4. There is a very wide range of MEDs within each skin type and a substantial degree of overlap in the MED values among different skin types.
MED is typically measured as follows.
- A template with four or five 1 to 2-cm squares is applied to a non-sun exposed area (often volar forearm or buttocks).
- Surrounding skin is protected from exposure.
- The squares are exposed to a series of increasing doses of broadband UV according to estimated skin type, using a 2-foot source.
- Test sites are outlined with a skin marker so they can be identified.
- The response is measured 24 hours later. The MED is the lowest dose that produces pink erythema with distinct borders.
- The test may be repeated using a different range of test doses if either all or none of the test sites have erythema.

MED testing template
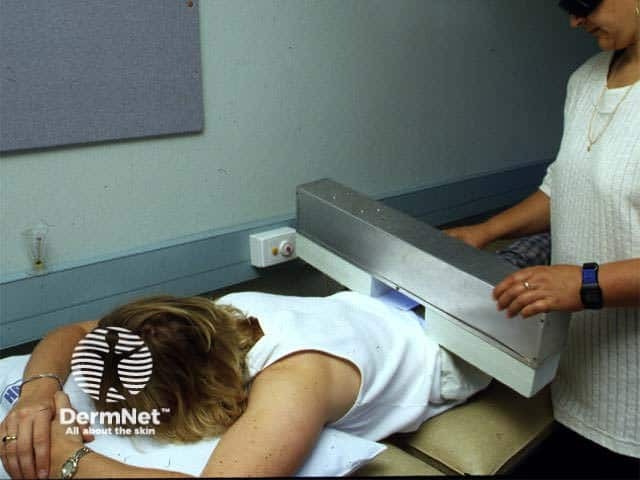
MED testing
Recommended BB-UVB MED test doses (mJ/cm2):
| Skin Type | Square 1 | Square 2 | Square 3 | Square 4 | Square 5 |
|---|---|---|---|---|---|
| 1 | 10 | 20 | 30 | 40 | 50 |
| 2 | 20 | 30 | 40 | 50 | 60 |
| 3 | 30 | 40 | 50 | 60 | 70 |
| 4 | 40 | 50 | 60 | 70 | 80 |
MED is rarely measured in phototherapy departments in New Zealand. The test is somewhat inconvenient and difficult to perform accurately. NB-UVB is only available as 6-foot TL-01 bulbs, which are impractical for testing.
Dose regimen for UVB
The manufacturer of the equipment may provide recommended starting doses. This may be a standard dose for all patients or may depend on skin phototype or measured MED. Most patients attend three times weekly. Twice weekly is less effective and once weekly is ineffective. Inpatients may be treated five times weekly but this is rarely practicable or tolerated by outpatients. Clearance generally occurs with the same total number of treatments if UVB is delivered three, four or five times weekly.
Patients should receive increasing doses each visit until erythema develops or until a prescribed maximum dose has been reached. The maximum depends on phototype and local protocol.
For most patients, the whole body is treated except the face and genitals.
BB-UVB
Typically, the first treatment is 70% MED when known. It is more cautious for photodermatoses. The time to deliver the total dose will depend on the energy output of the source/irradiance.
Here is a typical chart that uses estimated skin phototypes to determine the initial dose and subsequent increments each treatment, in the absence of erythema.
Recommended BB-UVB doses (mJ/cm2):
| Skin type | Initial dose | Subsequent increase |
|---|---|---|
| 1 | 21 | 10% |
| 2 | 35 | 10-15% |
| 3 | 49 | 15% |
| 4 | 63 | 15-20% |
| 5 | 84 | 20% |
| 6 | 105 | 20% |
NB-UVB
Usually, a standard starting dose of 50–100 (mJ/cm2) is used with increments 10–40% per treatment depending on skin phototype.
Erythema
The development of significant erythema precludes further dose increments. Although undesirable, it is a necessary part of treatment for many patients in order to deliver the most effective dose to clear their skin disease. Suberythemal doses of NB-UVB are however effective in clearing psoriasis.
Phototoxic reactions to narrowband UVB
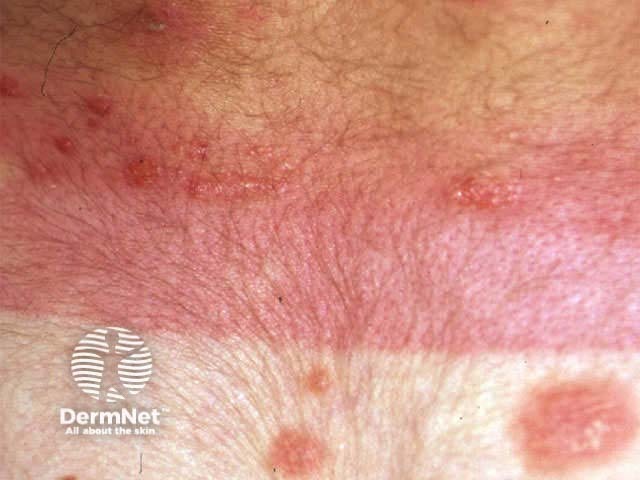
NBUVB burns
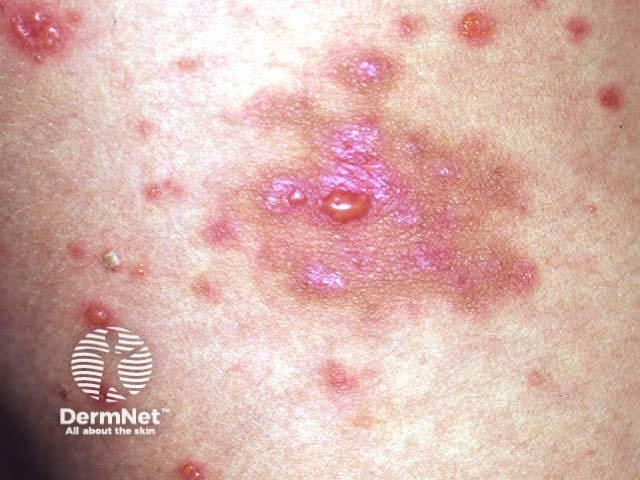
NBUVB blisters
The patient should be examined prior to each treatment. Erythema may be localised or generalised. Localised erythema can be protected allowing incremental exposures to the rest of the body, as scheduled, but generalised erythema should result in changes to the schedule.
- No erythema: dose according to schedule.
- Asymptomatic erythema (pink): hold at the previous dose.
- Symptomatic but subsided erythema (red): reduce by 10%.
- Erythema and tenderness still present: withhold treatment.
- Marked pain or blistering: withhold, and then reduce by 25%.
Phototherapy staff should inform the physician if significant symptomatic erythema arises.
Treatment interruptions
If treatment is interrupted, doses may need to be reduced to the starting dose or as follows:
One week: hold at previous dose
2 weeks: reduce dose by 25%
3 weeks: reduce dose by 50%
4 weeks or more: restart schedule
Interruptions to treatment are the most common reason for the failure of phototherapy. Tanning/keratinocyte hyperplasia may reduce the penetration of UVA, but lack of tanning could result in symptomatic erythema.
End of course
A course is completed when the skin disease has cleared more than 90% compared to baseline, or according to a pre-determined maximum number of treatments, commonly 40. Maintenance therapy is not generally recommended (except perhaps for cutaneous T-cell lymphoma).
Other treatment options should be considered in patients who fail to clear or substantially improve with UVB phototherapy. Plaques of psoriasis should be thinning by 12 treatments and by 30 treatments psoriasis should be 75% improved or better.
Phototherapy may be recommenced on relapse, depending on the severity of the disease, other treatment options and individual factors.
Supplementary treatment
Some areas of skin disease may prove more resistant to UVB than others, often because of prior sun exposure. Commonly, in patients with psoriasis, additional UVB is delivered to the lower limbs. After the whole-body dose has been given, the patient dresses up to protect the rest of the body from further exposure. An extra 50% of the day's dose is delivered to the resistant sites.
Many patients are treated with additional topical or systemic therapy. In some cases, the additive benefit has been demonstrated by clinical trials. For example, adding emollients, coal tar ointment or calcipotriol ointment and/or oral acitretin or methotrexate can reduce the number of UVB treatments required to clear psoriasis. In atopic dermatitis, it may be advantageous to add in UVA as well as topical steroids, emollients and when necessary, oral antibiotics.
Emollients applied to scaly skin immediately before exposure to UVB must not act as sunscreens. Paraffin and coconut oil are satisfactory. Peanut oil should be avoided because of the risk of anaphylaxis.
Complications of treatment
Acute complications include:
- Acute sunburn effect: tender erythema and /or pruritus
- Anti-inflammatories such as aspirin or indomethacin reduce pain and severity
- Topical steroids applied early reduce pain and severity
- Emollients applied frequently to reduce itching
- Ocular toxicity: photokeratitis causing grittiness, pain, photophobia, tearing and blepharospasm
- Frequent application of artificial tears soothe discomfort
- Polymorphous light eruption
- Irritable erythematous papules on the skin that is not usually sun-exposed
- Treat with emollients and topical steroids. Rarely, systemic steroids are necessary for a severe reaction.
- Reduce UVB dose and reduce increments
- Blisters: NB-UVB may rarely cause lesional bullae
- Herpes simplex (treat with aciclovir and cover affected area)
- Worsening skin disease
- Koebnerisation from erythema is treated with more UVB
- If due to photo-aggravation, UVB may have to be discontinued
- Consider other reasons for flare-ups
- Consider other treatment options.
Long-term complications include:
- Photo-ageing:
- Wrinkling, freckling, xerosis, telangiectasia, elastosis and atrophy
- Skin cancer:
- Actinic keratoses, squamous cell carcinoma, basal cell carcinoma and melanoma.
Machine maintenance
A total-body phototherapy unit should include safety features such as proper electrical grounding, accurate dosimetry device, protective shielding of the lamps, handrails for support, viewing window for staff observation, doors that open easily and adequate cooling.
Equipment used to treat patients must comply with New Zealand's stringent electrical regulations.
Records
Phototherapy staff should keep records documenting each patient's treatment including exposure dose, the area treated, extent/severity of disease and degree of erythema. Some units are able to record this information automatically but a hard copy backup is recommended. Treatments that were withheld should be recorded with the reason for it. Record the follow-up arrangements during the course of treatment and after it has been completed.
Records may include:
- Doctor's referral
- Evaluation prior to treatment
- Signed consent form
- Treatment record
- Photographic record of disease
- Progress report for the doctor
- Doctor's follow-up report
- An end-of-treatment summary
- Audit data
Excimer laser
The excimer laser emits radiation at 308 nm and can be used to treat localised plaques of psoriasis. Typically the laser is used three times a week and achieves 90% clearing of plaques in an average of 10 treatments, i.e. more rapidly than other forms of phototherapy. Typically a spot size of 3.5 cm is used at 2 minimal erythema doses and a pulse width of 30 ns. Common side effects include erythema, blisters, hyperpigmentation, and erosions, but they are well tolerated. Excimer laser treatment spares uninvolved skin. Remission rates are similar to narrowband phototherapy.
This treatment is not yet available in New Zealand. However, other forms of targeted UV are available at certain dermatologists' offices including Daavlin T500x.
Activity
Compare and contrast narrowband UVB machines from different manufacturers.
References
On DermNet
Information for patients
